Representative cases
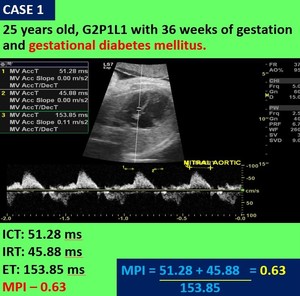
Fig. 3: Case 1 - Case of gestational diabetes mellitus with increased MPI value
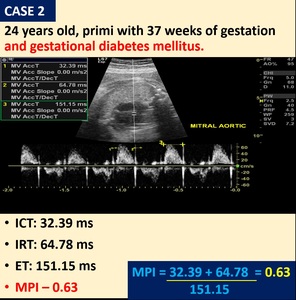
Fig. 4: Case 2 - Mother with gestational diabetes mellitus with increased MPI value
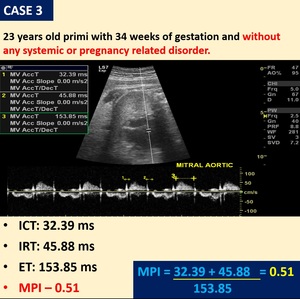
Fig. 5: Case 3 - Primi with no comorbidities having normal fetal MPI values
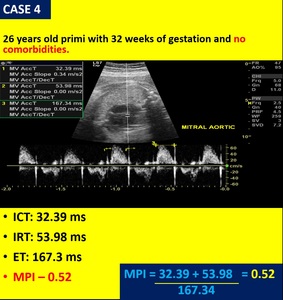
Fig. 6: Case 4 - 26 years old primi with 32 weeks of gestation and no comorbidities having normal fetal MPI values.
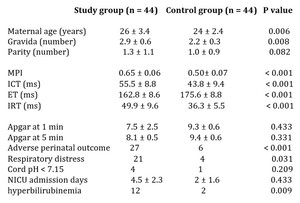
Table 1: Table 1 : Results obtained from our study
Table 1 summarizes the characteristics of the study population. The two groups were similar for maternal age and gestational ages at assessment. From our study it was found that foetal left ventricular Mod-MPI values were significantly higher in the diabetic group compared with the controls (0.65 ± 0.06 vs 0.50 ± 0.07). There was a statistically significant difference between the 2 groups (P<0.001). Table 2
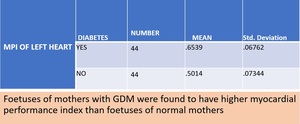
Table 2
Table 3 demonstrates that pregnant women with gestational diabetes mellitus were seen to have more ICT, IRT values than non-diabetic women. Among the individual variables studied, ejection time (ET) was found to be the most significant parameter affected in foetus of diabetic mothers (area under ROC curve – 0.87). Table 3

Table 3
In this study it was found that foetuses with high MPI values are more prone for perinatal complications. Majority of them presented with respiratory distress, hyperbilirubinemia, perinatal acidosis. These babies had a reduction in 1min and 5 min APGAR scores compared to babies of non-diabetic mothers. Among the 44 cases there were 2 still births and 1 perinatal death in our study population.
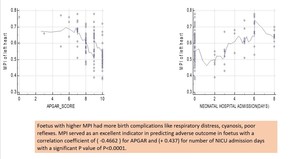
Fig. 7: Correlation regression analysis between MPI vs APGAR score shows, as MPI value increases the 1-min APGAR score considerably decreases.
Correlation regression analysis between MPI vs NICU admission days shows, as MPI value increases number of days of NICU admission increases.
Figure 7 demonstrates the correlation between MPI vs APGAR score & MPI vs NICU admission days. Almost all babies with MPI value >0.58 were having adverse perinatal outcome (sensitivity of 100% & specificity of 90% with 95% confidence interval.) Fig. 7
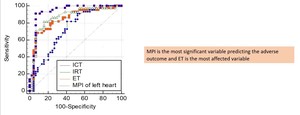
Fig. 8: ROC curve analysis shows that MPI is the most significant variable predicting the adverse outcome and ET is the most affected variable
Mod-MPI serves as a good predictor of adverse perinatal outcome in foetus of diabetic mothers (Area under ROC curve – 0.932) Fig. 8
In our study, we investigated the association between foetal left ventricular mod- MPI and maternal diabetes, either pregestational or gestational. It was found that MPI values in diabetes patients were significantly higher than the control group. It means that there is an impairment of global cardiac function of left ventricle. There was no statistically significant correlation between MPI values of foetuses and maternal age. Also, there was no significant difference in MPI values for foetuses of pregestational and gestational diabetes mellitus. So, these results support the use of foetal left ventricular MPI for the prediction of adverse perinatal outcomes in pregnancies with diabetes. The increased incidence of respiratory distress may be due transient tachypnoea because of diastolic dysfunction, indicated as an increase in IRT. Two cases of still births with high MPI values (0.69 and >0.71 respectively) may be due to severe myocardial dysfunction. Our study showed that MPI >0.58 was associated with some kind of adverse perinatal outcomes.
Bhorat et al 10 stated that left ventricular MPI value > 0.52 was reported with a sensitivity of 100% and a specificity of 92% for the prediction of adverse perinatal outcomes, including one stillbirth and one neonatal death.
Sanhal CY 11et al found that foetal left ventricular MPI values were significantly higher in the diabetic group compared with controls (0.56 ± 0.09 vs 0.36 ± 0.04, P < 0.001), whereas E/A ratio was lower (0.66 ± 0.11 vs 0.69 ± 0.09, P = 0.049). The adverse perinatal outcome rate was also higher in the diabetic group.
The differences in complications and complication rates between our study and these two studies may be a result of the characteristics of the study population (South Indian) and the available management strategies.
De Assuncao et al. 12-13 recently reported that worsening foetal anemia was associated with a reduction in the left ventricular MPI value. They concluded that left ventricular performance not only remained preserved but also was augmented in cases of moderate and severe anemia.
Limitations
Our study is a case control study with small sample size. A prospective cohort design with larger number of participants could be more valuable.
To clearly understand the utility of perinatal MPI, long-term postnatal follow-up of the cardiac status of the baby would be helpful.










