1. UNDERSTANDING CAROTID ENDARTERECTOMY
Endarterectomy (CEA) is an open surgery, in which the Carotid arteries are sectioned longitudinally to expose the arterial lumen, and from inside, remove the intimal layer of the arterial wall along with atheromatous plaque. The arteriotomy is closed after that, by simple suture, or also using a venous (autogenous) or synthetic patch (Dacron, PTFE), to widen the lumen.

Fig. 1: Drawing that shows the technic of endarterectomy with or without patch.
After the procedure, three main obstructive problems can arise: 1) narrowing of the lumen, 2) peristance of residual plaque or 3) neointimal hyperplasia.
2. ULTRASOUND EVALUATION PROTOCOL
In the immediate postoperative period, suturing, clips and bandages can make the exam difficult. In the follow-up study, the patient's already healed scar does not generate technical difficulties.
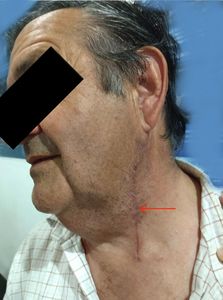
Fig. 2: Endarterectomy scar at lateral neck area.
There should be a mandatory baseline study, at the inmediate postoperatory or in the first month, as a reference for future examinations, where the velocities and types of waveforms must be reported.
Ultrasound control is recommended every 1-2 years in the absence of stenosis, or every 6 months if there are lesions that can evolve to significant stenosis, residual or recurrent ipsilateral stenosis and contralateral occlusion.
Patient positioning: Supine position, with the chin facing the ceiling, slightly lateralized, similar to normal carotid study.
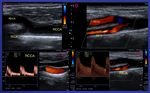
Complete evaluation of Carotid vessels on both sides and vertebral arteries should be scanned in B mode and color Doppler.
The arterial spectral analysis should be performed as in the routine carotid examination, observing normal waveforms or high resistance morphology until reepithelialization of the posterior wall occurs.
Special attention should be given at some points, such as the proximal and distal intimal shelves or upper and lower limits, of the ECA site.
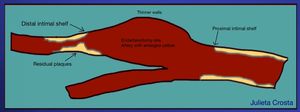
Fig. 3: Drawing of Carotid bifurcation after endarterectomy. It is importante to explore with special detail, the proximal and distal limits or ¨shelves¨of the endarterectomy, where a step is seen, representing the intimal layer. In the ECA site, the walls of the artery are thinner, the arterial calibre is enlarged.
In the distal part of the ICA residual plaques can be seen.
3. ULTRASOUND FINDINGS

Table 1: Sonographic findings that can be found after endarterectomy
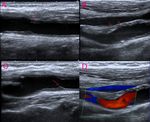
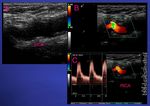
The caliber of the lumen and its shape depend on the type of arteriotomy closure that has been performed, with or without patch. Fig. 4 Fig. 5 Fig. 6 Fig. 7
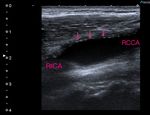
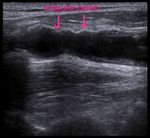
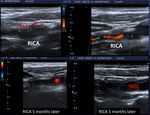
3.1 Intimal shelves or endarterectomy limits: The proximal begining and the distal ending points of the endarterectomized segment are usually visible. The location of the proximal "shelf" is determined by the surgical technique and the severity of the disease in the CCA. Small alterations of the flow can be observed at the distal end point of the endarterectomy, but normally there should be no significantly high velocities or extreme flow disturbances.
Modest flow disturbances observed early may disappear in subsequent studies due to natural vessel remodeling. Fig. 8
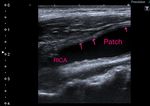
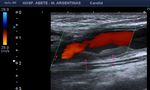
3.2 Patch: The visualization of the patch depends on the type of material used and the time interval after surgery. The autogenous venous patch may not be distinguishable from the native tissue, even in the early postoperative period. However, the patched segment may be recognized by a bulging appearance on the endarterectomy site, and the possible visualization of adjacent sutures. The suture line may be seen in B mode. The suture stitches can be recognized as small, bright, hyperechoic and regularly spaced echoes along the near wall of the vessel. Fig. 9
If it is synthetic patch, it is usually seen as an echogenic material in the arterial wall. PTFE: bright double line interface. Dacron: thick and echogenic.
If it is scanned during the first 48 hours from surgery, a small amount of air trapped inside the PTFE and Dacron material can be observed, which can cause acoustic shadow and difficulty visualizing the vessel's lumen. Fig. 10
4. COMPLICATIONS:

Table 2: Complications after endarterectomy
4.1 Intimal flaps: It is a small disruption in the intimal layer, with a small piece of material protruding and moving into the vessel lumen at the endarterectomized artery, in the intra or postoperative image. It can be limited with no clinical significance or it may be a significant flap with risk of thrombosis or embolia. It can cause elevated velocities and Color flow disturbances. Fig. 11
4.2 Hematomas or infection: Surgical area swelling suggests infection that is associated with synthetic patches but it is not frequent. Patch rupture is associated with venous patches. The presence of perivascular liquid collections may suggest hematomas, pseudoaneurysms or infection. An irregular buckling of patch material along vessel wall, and perivascular fluid collections are associated with infected patch. Fig. 12
4.3 Pseudoaneurysm: Dilated area attached to the vessel, with color swirling ¨yin-yang¨ appearance, with spectral flow ¨to and fro¨ demonstrated at the connection with the native vessel. They are not usually due to ruptures of the patch, but are more frequently caused by dehiscence of the sutures. Fig. 13
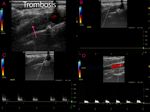
4.4 Thrombosis: Manipulation of the artery can cause thrombosis, also the synthetic patch is more thrombogenic. By ultrasound, the lumen may be occupied with hypoechoic material (thrombus), partial or total. It can cause occlusion with no evidence of flow with Color or Spectral Doppler. In the proximal sites, a preocclusive flow can be seen, with low sistolic velocities, high resistance due to absent diastolic flow. Fig. 14
4.5 Restenosis: It usually happens at the distal arteriotomy, where the artery recovers the intima layer, at the distal ¨shelf¨. However, there are several causes that are listed in Table 3. The incidence rate is 6-14%. They are recognized as a focal area of elevated velocities with post-estenotic turbulence.

Table 3: Causes of restenosis post-endarterectomy
Stenosis within the first postoperative month should be considered a technical problem of surgery. They could be the result of narrowing fo the lumen because of primary arteriotomy, or residual plaque that was nor resected during the procedure.
a - Residual or retained plaque: This refers to a plaque that probably could not be resected because it was very distal or because the neck was short or with difficult surgical access. It's called "shelf lesion." The plaque generates an abrupt slope or step of the arterial wall, which protrudes towards the lumen. This can occur at both ends of the endarterectomy. But at the distal end, it is more frequent. Fig. 15
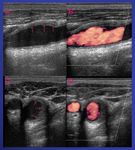
b- Neointimal Hyperplasia: It is an hyperplastic reaction of the artery wall to the surgical aggression that presents during the first 24 months. Sonographically, it is recognized as a slightly echogenic homogeneous lesion in the inner surface of the arterial wall, that can grow within the lumen. Usually, they are asymptomatic and stable. They can involve. Fig. 16 Fig. 17
c- Progressive atherosclerotic disease: After 2 years of surgery, restenosis is considered to be caused by recurrence of arteriosclerotic disease, potentially more problematic. The factors that increase the risk for this area the presence of residual plaque that progresses, the small caliber of distal internal carotid, smoking, hypertension, progression of contralateral disease. Usually it presents with heterogeneous plaque, with calcifications. They are more stable than the primary plaque. They can become symptomatic or evolve to vessel occlusion. Fig. 19 Fig. 20

Fig. 18: Carotid velocity criteria for patients with ECA with patch
References: AbuRahma AF, Stone PA, et al. Proposed duplex velocity criteria for carotis restenosis following Carotid Endarterectomy with patch closure. J Vasc Surg. 2009; 50: 286-291.