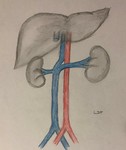
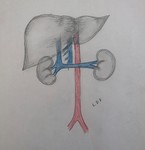
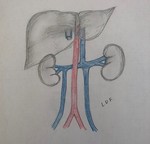
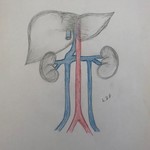
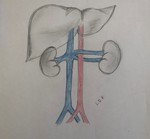
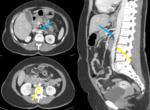
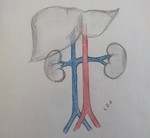
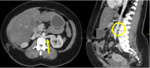
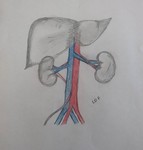
EMBRIOLOGIC DEVELOPMENT
It is important to know the embryogenesis of the inferior vena cava, because the different anatomical variants have their origin in anomalies in the process of regression, persistence or anastomosis of the embryonic veins.
The embryo has three pairs of veins, which are located on both sides of the Aorta. The left veins and the communicating veins involve, and it is from the anastomosis of the following embryonic veins that the inferior vena cava is formed.
- Posterior cardinal vein: it is the first to appear, common iliac veins are formed from the segments that persist.
- Supracardinal vein: the inferior infrarenal vena cava, the azygos and hemiazygos veins derive from this embryonic vein.
- Subcardinal vein: it forms the infrahepatic and adrenal inferior vena cava (prerenal segment).
- Vitelline vein: it is a single vein, which forms the hepatic segment.
The left renal vein is formed from an intersubcardinal communicating vein that crosses anterior to the aorta.
The embryological ureter has an anterolateral path to the supracardinal vein and it is posterior to the posterior cardinal vein.
CONGENITAL ANOMALIES
They are present in approximately 4% of the population. The majority are asymptomatic and diagnosed incidentally.
The radiologist must know the different variants, because the correct diagnosis is important for planning vascular interventions and to avoid future diagnostic errors.
Computed tomography (CT) is the main imaging technique to evaluate the vena cava inferior anomalies. CT is performed with intravenous contrast (100 - 150 ml at 3-5 ml / sec), obtaining a venous portal phase (60 - 70 seconds) which shows enhancement in the inferior vena cava.
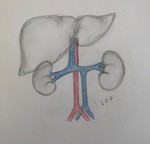
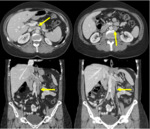
1. Left inferior vena cava.
Regression of the right supracardinal vein with persistence of the left supracardinal vein.
It follows a cranial path to the left of the abdominal aorta and it joins the left renal vein, crossing together anteriorly to the aorta and draining into the right renal vein, to form the normal prerenal segment.
It has no clinical difficulties in the placement of an infrarenal vena cava filter by a transjugular approach must make the radiologists suspect about this venous anomaly.
Differential diagnosis with paraaortic adenopathies.
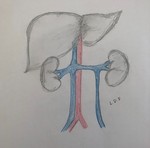
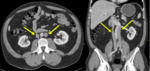
2. Double inferior vena cava.
Persistence of both supracardinal veins forming two infrarenal segments. The left vein joins the renal vein and drains into the normal adrenal segment.
It should be suspected in patients with recurrent pulmonary thromboembolism despite carrying a vena cava filter, the solution is placing a filter into each vena cava.
Differential diagnosis with paraaortic adenopathies.
3. Interruption of the inferior vena cava with azygos or hemiazygos continuation.
There is a failure in the right subcardinal-hepatic anastomosis with atrophy of the right subcardinal vein.
The kidneys drain into the renal segment of the inferior vena cava, which has a posterior path through the diaphragmatic crura and continues in the thorax as the azygos vein, which drains into the superior vena cava.
In the case of the left inferior vena cava, it continues in the thorax as an hemiazygos vein, which crosses at the level of T8 - T9 to drain into the azygos vein.
The liver segment drains directly into the right atrium.
Each gonadal vein drains into the ipsilateral renal vein.
It is associated with abnormalities of situs ambigous / heterotaxy syndromes.
Differential diagnosis with right paratracheal mass and retrocrural adenopathy.
4. Absent inferior vena cava with preservation of the suprarenal segment.
It can be complete or only affect to the infrarenal segment, which is named "with preservation of the adrenal segment".
It is the result of the failure in the complete development of the embrionary vein. There may be significant collateralization, which can simulate paraspinal masses.
There may be more than one anomaly.
a) Double inferior vena cava with retroaortic right renal vein and continuation with hemiazygos.
Persistence of the left lumbar and thoracic supracardinal vein and the left suprasubcardinal anastomosis with failure in the formation of the right subcardinal-hepatic anastomosis. The right renal vein and the right inferior vena cava join and cross posterior to the aorta draining into the left inferior vena cava which continues cranially as the hemiazygos vein. The hemiazigos vein crosses posterior to the aorta at the level of T8 - T9 to drain into the rudimentary azygos vein.
b) Double inferior vena cava with retroaortic left renal vein and continuation with azygos.
Persistence of the left supracardinal vein and the intersupracardinal vein and failure in the development of the subcardinal-hepatic anastomosis.
The left inferior vena cava joins the left renal vein and crosses posterior to the aorta, draining into the right inferior vena cava and continues as azygos vein. ( Fig. 11 )
The differential diagnosis of both anomalies must be done with a mediastinal mass.
5. Circumaortic left renal vein.
It is the most frequent variant.
Persistence of the intersubcardinal and intersupracardinal communicating veins, forming two left renal veins:
- Superior: it crosses anterior to the aorta and it receives left adrenal vein.
- Inferior: it crosses the aorta posteriorly and it receives the left gonadal vein.
Differential diagnosis with retroperitoneal adenopathy.
It is important in patients who undergo a nephrectomy and abdominal aortic aneurysm surgery.
6. Retroaortic left renal vein.
Regression of the intersubcardinal communicating vein with persistence of the intersupracardinal communicating vein.
7. Retrocaval (circumcaval) ureter.
It always occurs on the right side.
Persistence of the right posterior cardinal vein which results in the inferior vena cava.
The ureter courses posterior to the inferior vena cava, right to the aorta and anterior to the right iliac vessels.
Radiologists must suspect this anomaly in patients with hydronephrosis or recurrent urinary infections (partial ureteral obstruction).
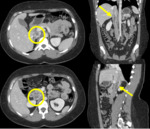
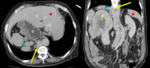
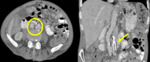
INFERIOR VENA CAVA PATHOLOGY
There are some pathologic entities which are related or can affect to the inferior vena cava, such as extrinsic compressions (different ethiologies), thrombus and malignant tumors arising in adjacent organs and tissues.
Some examples collected in the hospital are the following:
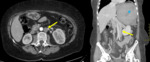
1. Venous thrombosis:
It should be taken into account that when a portal venous phase is performed, contrast-enhanced blood from the kidneys mixes with non-enhanced blood from the infrarenal segment, which can mimic a filling defect producing a false image of thrombus. This pitfall can be solved performing a delayed phase.
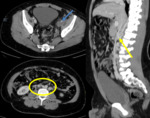
2. Retroperitoneal masses and adenopathies:
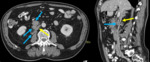
3. Tumor infiltration:
4. Situs inversus and ambiguous (heterotaxy):
It is common to find congenital anomalies of the inferior vena cava in these patients.
5. Inferior vena cava filter: