Learning objectives
This audit performed at a single centre in a district general hospital in the UK aims to assess:
Whether CTPA scans are being used appropriately.
The diagnostic yield of CTPA scans.
How appropriate are clinical requests?
Has risk stratification/pre-test probability screening been documented?
Can age adjusted d-dimer be used as a suitable pre-test screening tool?
Background
Significant morbidity and mortality is associated with pulmonary embolism (PE)2
A normal CTPA result can safely exclude PE in all patients2
CTPA is quick to perform, rarely needs to be followed by other imaging, may provide the correct diagnosis when PE has been excluded and is available 24/7 in most centres1.
There is a significant radiation dose and scans need to be targeted to the correct patient population3.
In our centre, requests for CTPA continue to rise annually (approximately 1-3% increase per year) but the...
Findings and procedure details
Audit Standards:
Referrals should be in line with agreed local protocol for referral.
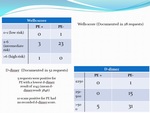
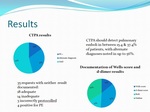
According to published studies conducted at regional centres CTPA should detect pulmonary emboli in between 15.4 & 37.4% of patients, with alternate diagnoises noted in upto 56%2.
All requests should have a documented Wells score, d-dimer result and adequate clinical history.
Target
1. 100%
2. 100%
3.Pulmonary emboli in at least 15%, with alternate diagnoses in at least a further 50%.
Data items collected:
1. Patient age and gender
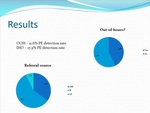
2. Referral source...
Conclusion
Positive detection rate (15%) and alternate diagnosis rate (31%) below the RCR recommendation.
Only 15% of requests provided both a Wells score and d-dimer result with 34% of requests providing neither.
Raising of the locally agreed d-dimer cut-off from 250 to 500 would not have resulted in any missed cases.
Using the age adjusted d-dimer cut-off is highly sensitive.
38% of requests were deemed inadequate or incomplete based on the clinical details provided to justify a CTPA. All of these requests were negative for PE....
Personal information and conflict of interest
N. Mirajkar; Birmingham/UK - nothing to disclose G. Rowe; Herefordshire/UK - nothing to disclose
References
1.iRefer / Making best use of a Department of Clinical Radiology, Guidelines for Doctors, Seventh Edition 2012, The Royal College of Radiologists, London.
2.Mos IC, Klok FA, Kroft LJ, DE Roos, Dekkers OM and Huisman MV. Safety of ruling out acute pulmonary embolism by normal computed tomography pulmonary angiography in patients with an indication for computed tomography: systematic review and meta-analysis. J Thromb Haemost. 2009 Sep;7(9):1491-8. Epub 2009 Jun 22.
3.Venous thromboembolic disease; the management of venous thromboembolic diseases and the role of thrombophilia testing,...