Type:
Educational Exhibit
Keywords:
Not applicable, Inflammation, Diagnostic procedure, PET-CT, MR-Angiography, CT-Angiography, Vascular, Arteries / Aorta
Authors:
A. Ribrag1, C. Cholet1, A. mekinian1, O. fain1, L. MONNIER-CHOLLEY1, L. Arrivé2; 1PARIS/FR, 2Saint Mandé/FR
DOI:
10.26044/ecr2020/C-08116
Background
A. Definition
Takayasu’s arteritis (TA) is a rare chronic idiopathic large vessel vasculitis that primarily involves the aorta and its main branches, and less frequently the pulmonary and coronary arteries. TA preferentially affects young women in the second and third decades of life and is most common in people with Asian ethnicity.
B. Pathophysiology
Histopathologic features include granulomatous panarteritis with lymphomonocytic infiltration. Initial intimal inflammation and proliferation, eventually evolving into fibrosis, leads to arterial wall thickening and stenosis. Destruction of the elastic and muscular layers leads to aneurysms and dissection. These lesions may induce organ dysfunction secondary to ischemia.
C. Clinical Features
During early active inflammatory phase, symptoms are usually nonspecific, such as fever, myalgias, weight loss, and arthralgias. In the chronic phase, ischemia and symptoms secondary to arterial occlusion are predominant.
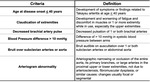
TA diagnosis can be made accurately using the 1990 American College of Rheumatology criteria (Figure 1).

Fig. 1: ACR diagnostic criteria for Takayasu's arteritis included clinical features and angiographic findings.
References: Arend WP et al. The American College of Rheumatology 1990 criteria for the classification of Takayasu arteritis. Arthritis Rheum. 1990;33(8):1129-1134.
D. Treatment Options
Treatment relies on steroids, usually combined with immunosuppressive agents. Anti-tumor necrosis factor agents, tocilizumab and rituximab, are used in refractory cases. When ischemic complications occur, patients may benefit from endovascular interventions or vascular surgery.