IPNBs usually manifest as intra-ductal masses with bile duct dilation (proximal and sometimes distal); which may be tubular, fusiform or cystic. Imaging appearance depends predominantly on two features; papillary proliferation and mucin production.
The detection of these lesions is based on their size; the most dilated bile ducts are usually the ones containing the tumour lesion, even when it is not radiologically recognisable.
Herein we present 3 cases:
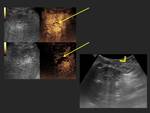
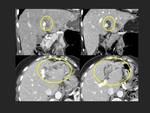
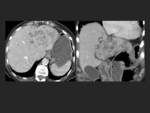
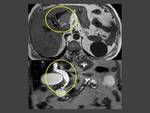
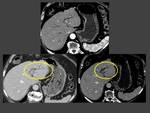
Case 1: (Fig. 1)(Fig. 2)(Fig. 3)
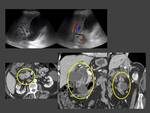
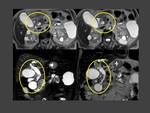
Case 2:(Fig. 4)(Fig. 5)(Fig. 6)(Fig. 7)
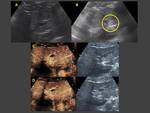
Case 3: (Fig. 8)(Fig. 9)
Tumour imaging:
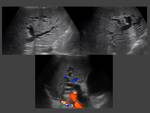
At US IPNB may be seen as a hypoechoic or hyperechoic mass within the bile duct with preserved wall integrity. It may be difficult to identify as the echogenicity of the mass is similar to that of the liver.
Contrast enhanced US may be used to show lesion enhancement and differentiate it from the bile. However, this technique does not allow differentiating benign from malignant lesions.
At CT these tumours generally manifest as segmental and asymmetric thickening of the bile duct wall with enhancing or non-enhancing intraluminal masses.
At MR IPNBs will appear iso- or hypo-intense on T1 weighed images and hyper-intense on T2 sequences. At late arterial phase they will present a iso- or hyper-intensity that will not remain on the venous phase, a characteristic that will help us differentiate this entity from cholangiocarcinomas; which will show progressive enhancement at venous and delayed phases.
Diffusion weighted images can be used to prove restriction of the solid part and the invasive nature of the mass, but cannot be used to evaluate the extent of the tumour.
Mucin appearance:
The capacity of US, CT and MR to detect mucin is limited because mucin has the same echogenicity, attenuation and signal intensity, respectively, as the bile.
MR Cholangio-pancreatography may be capable of detecting mucin as linear and curved hypo-intense stripes in dilated ducts of mucin-secreting IPNBs, feature called “thread sign”.
Sometimes tumours can generate fistulas with adjacent structures, leaking mucin into the peritoneum, which results in pseudomyxoma peritonei. Fistulas can be identified on CT and MR.
Definitive treatment is surgery; IPNBs limited to intrahepatic ducts may be treated with partial hepatectomy; in tumours involving either the extrahepatic or right / left main ducts, resection of common duct with Roux-en-Y anastomosis may be performed. Non-surgical candidate patients, due to extent of the disease, may be given palliative treatment with common bile duct stenting and drainage to alleviate pain and jaundice.