1) TESTIS AND SCROTUM
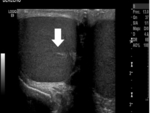
- NORMAL SCROTAL US IMAGING: ( Fig. 1, Fig. 2, Fig. 3 and Fig. 4 )
Testis and scrotum:
A) Scrotal layers: Minimally hyperechogenic or isoechogenic compared to testis. Thickness
B) Testis: Homogenous and intermediate echogenicity.
C) Tunica albuginea: Echogenic rim surrounding the testis and gives rise to hypoechoic septa that extend deep into testicle dividing it into lobules.
D) Tunica vaginalis parietal and visceral: The parietal and visceral layers are separated by physiological hydrocele.
D) Mediastinum testis: Hyperechoic band extending in craniocaudal direction.
E) Rete testis: Network of hypoechoic tubules adjacent to mediastinum testis.
F) Epididymis: Isoechogenic or slightly hypoechoic compared to the testicles. Divided into head, body and tail, located posterolateral to testis.
G) Appendages: There are 4 testicular/epididymal appendages. Appendix testis (most common), appendix epididymis, Paradidymis or organ of Giraldes or Vas aberrans of Haller.
+ Spectral Doppler of intratesticular vascularization: Low-resistance arterial waveform (IR between 0.5-0.7).
+ Spectral Doppler of extratesticular vascularization: High-resistance arterial waveform (IR between 0.7-1).
- PATHOLOGICAL SCROTAL US IMAGING:
A) VASCULAR PATHOLOGY:
I) Torsion testicular (Fig. 5): May occur complete torsion or incomplete torsion.
- Complete torsion:
-> US B mode findings: In early stages testes could be normal, however as ischemia progress become enlarged, heterogeneous and hypoechoic areas. The spermatic cord twisted and thickened (Whirlpool sign). Enlargement of epididymis. Reactive hydrocele. Scrotal layers thickening.
-> Doppler US findings:
+ Complete torsion (>360º): Absence of intratesticular blood flow.
+ Incomplete torsion (<360º): Decreased, absence or diastolic inversion of diastolic curve in intratesticular blood flow. Elevated RI (> 0.5).
II) Torsion of testicular appendage (Fig. 6):
-> US B mode findings: Nodule hypo or hyperechogenic usually located at upper pole of testis. Reactive hydrocele. Scrotal layers thickening. It appears decrease and calcified in chronic phase.
-> Doppler US findings: The nodule is avascular. Increased peripheral flow may be seen. Intratesticular flow is normal.
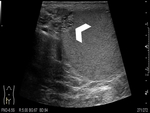
III) Segmental testicular infarction (Fig. 7):
-> US B mode findings: Hypoechogenic wedge-shaped area in the testicle, with the vertex directed to the testicular mediastinum.
-> Doppler US findings: Absence of flow in the hypoechoic area. Remaining testicular parenchyma show normal flow.
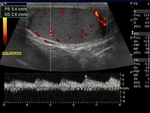
IV) Varicocele (Fig. 8):
-> US B mode findings: multiple anechoic serpiginous and tubular structures (> 2-3 mm). May be seen internal echoes caused by slow blood flow.
-> Doppler US findings: Increase and reverse flow during the Valsalva maneuver.
B) INFECTION PATHOLOGY:
I) Epididymitis and epididymo-orchitis (Fig. 9): Most common causes of acute scrotal pain.
-> US B mode findings: Enlarged, hypoechoic and heterogeneous epididymis (could be seen hyperechoic if hemorrhage is associated). Reactive hydrocele. Scrotal layers thickening.
-> Doppler US findings: Increased vascularity with low-resistance arterial waveform (IR < 0.7 in epididymis and IR < 0.5 in testis).
-> Localization: From epididymis tail to head. Could progress to testis (epididymo-orchitis). Isolated orchitis is rare.
-> Complications: Abscess (avascular hypoechoic area within the epididymis, testis or scrotal layers), pyocele (heterogenous extratesticular loculated collections with detritus) and segmental/diffuse infarction (hypoechoic areas with inversion of the diastolic wave or a complete absence of vascularization).
II) Fournier gangrene (Fig. 10): necrotizing infection of the fascial planes of perineum, scrotum and abdominal wall.
-> US B mode findings: scrotal edema and echogenic foci related to soft tissue gas. Testes and epididymes are normal.
-> Doppler US findings: The scrotal layers depicts increased vascularity.
-> CT Findings: soft tissue inflammatory changes and subcutaneous gas.
C) TRAUMA PATHOLOGY:
I) Hematoma (Fig. 11): Single or multiple in testes or epididymis.
-> US B mode findings: Hyperechoic area In acute phase. In chronic phase it becomes hypoechoic or complex cyst areas.
-> Doppler US findings: Absence of blood flow. Remaining testicular parenchyma show normal flow.
II) Hematocele ( Fig. 11): Collection of blood between the two layers of the tunica vaginalis.
-> US B mode findings: In acute phase appears as an hyperechoic collection. In subacute-chronic phase becomes complex collection, hypoechoic, heterogeneous, and with septa.
-> Doppler US findings: Absence of blood flow in collection.
III) Testicular rupture (Fig. 12): Discontinuity in tunica albuginea.
-> US B mode findings: Disruption of tunica albuginea, extrusion of testicular parenchyma with alteration of the testicular contour and heterogeneous echostructure. Hematocele is usually associated.
-> Doppler US findings: Segmental or complete absence of intratesticular blood flow.
IV) Testicular fracture: Discontinuity in testicular parenchyma.
-> US B mode findings: Hypoechoic line corresponding to an hypoechoic area. It could be associated to discontinuity in tunica albuginea.
-> Doppler US findings: Absence of flow in the hypoechoic area/line.
D) OTHERS PATHOLOGIES:
I) Inguinoscrotal hernia (Fig. 13):
-> US B mode findings: Presence of bowel loop (presence of intraluminal gas and liquid) with peristalsis or omental fat in scrotal sac.
-> Doppler US findings: Hyperemia in scrotal soft tissue could be an indirect sign of strangulated hernia.
-> Complications: Strangulation and incarceration (Dilated bowel loop with diminished peristalsis. High resistance flow in bowel wall).
-> CT findings: It helps to identify complicated signs in case of strangulation, eg: neumatosis, compromise of blood supply...
II) Malignant testicular lesions (Fig. 14): Most of them are Germ cell tumors, which are divided in two groups, the seminomas and nonseminomatous germ cell tumors. Seminomas are most common than nonsemonomatous.
-> US B mode findings: Seminomas usually hypoechoic mass with ill-defined borders. Non-seminomatous tumors frequently are more aggressive, being more heterogeneous, with poorly defined margins and frequent cystic areas of necrosis, hemorrhage, calcification or fibrosis
-> Doppler US findings: Increased flows in the Doppler study. With high resistance arterial waveform.
2) PENIS
NORMAL PENIS US IMAGING (Fig. 15)
A) Corpora cavernosa: There are two corpora cavernosa, located dorsal and laterals with homogeneous mixed echogenicity. A cavernosal artery is located in the center of each corpus cavernosum
B) Corpus spongiosum: One corpus spongiosum ventromedial with mildly hypoechoic compared to the corpora cavernosa.
C) Tunica albuginea: Echogenic rim surrounding the three corporal bodies.
D) Buck fascia: Is an echogenic fibrous layer surrounding the tunica albuginea and is separated into dorsal and ventral sections: The dorsal compartment encloses the two corpora cavernosa, and the ventral compartment encloses the corpus spongiosum.
E) Deep dorsal vein of the penis: Dorsal and deep to Buck fascia.
F) Superficial dorsal vein of the penis: Dorsal and superficial to Buck fascia.
PENILE EMERGENCIES
I) Fracture (Fig. 16): Discontinuity in tunica albuginea of corpora cavernosa.
-> US B mode findings: Disruption of tunica albuginea. An hematoma may be seen deep to the Buck fascia or the skin
-> MR imaging: May be used to evaluate interruption of the tunica albuginea.
II) Mondor Disease: Thrombosis or thrombophlebitis in the superficial dorsal vein of the penis
-> US B mode findings: Noncompressibility of the dorsal vein with caliber increase and internal echoes.
-> Doppler US findings: Absence of flow in the superficial dorsal vein of the penis.