Type:
Educational Exhibit
Keywords:
Not applicable, Haematologic diseases, Diagnostic procedure, CT, Lung, Chest
Authors:
P. Simkus1, A. Banišauskaitė1, J. Noreikaite2, V. Buroviené1, J. ZAVECKIENE1, M. Arzanauskaite2; 1Kaunas/LT, 2Liverpool/UK
DOI:
10.26044/ecr2020/C-08460
Background
Eosinophils are multifunctional polymorphonuclear leukocytes that serve as an end-stage effector cells and also have specialized roles in the host defense mechanism. They contain several eosinophil-specific proteins in cytoplasmic granules and sometimes can harm the host by releasing specific proteins that are cytotoxic to tissues, resulting in pathologic processes. One of the proteins forms Charcot-Leiden crystals, presence of which in tissues and sputum is typical for eosinophil-related disease.
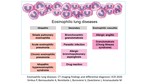
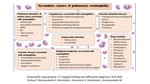
Eosinophilic lung diseases are a heterogeneous group of disorders that have association with tissue or peripheral blood eosinophilia. They can be classified into 3 main groups: idiopathic, secondary and eosinophilic vasculitis (Fig.1, Fig. 2). Eosinophilic lung diseases are commonly airway based, although, may be parenchymal or combination of both. Patient’s medical history, clinical and laboratory findings are of key importance for the diagnosis. Characteristic radiological patterns are very helpful in differential diagnosis of eosinophilic lung diseases. Chest radiography and computed tomography (CT) demonstrate characteristic features of eosinophilic lung disease and can suggest or confirm the diagnoses. While diagnostic difficulties may be caused by overlapping of CT features among the various eosinophilic lung disease forms, knowledge of these findings aids in timely diagnosis and management.
The diagnosis of the eosinophilic lung disease can be established if any of the following criteria is present:
· Tissue eosinophilia confirmed at lung biopsy;
· Increased (>10%) eosinophils in bronchoalveolar lavage (BAL);
· Pulmonary opacities with peripheral eosinophilia (absolute blood eosinophil count >0.5 x 109/L).