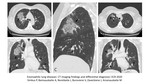
Simple pulmonary eosinophilia (Loeffler syndrome):
Simple pulmonary eosinophilia (SPE) can either be idiopathic or secondary to the presence of parasites, drugs or allergic bronchopulmonary aspergillosis (ABPA) with the most common causes being drugs and ascariasis (Table 1).

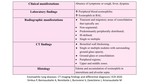
Table 1: Clinical, laboratory and radiological findings of SPE.
References: Shared work of the authors
Diagnostic criteria of SPE are:
- Migrating pulmonary opacities (Fig. 3.);
- Increased peripheral blood eosinophils;
- Minimal or no respiratory symptoms;
- Spontaneous resolution within 1 month.
Acute eosinophilic pneumonia (AEP)
A unique hypersensitivity reaction to an inhaled antigen with reported association between AEP and cigarette smoking, exposure to dust or smoke from fireworks (Table 2).

Table 2: Clinical, laboratory and radiological findings of AEP.
References: Shared work of the authors
There are 6 clinical diagnostic criteria of AEP:
- Acute febrile illness with an onset of less than 5 days;
- Progressive hypoxemia;
- Diffuse alveolar or mixed alveolar-interstitial opacities on chest radiographs (Fig. 4, Fig. 5.);
- BAL fluid consisting of more than 25% eosinophils;
- Absence of parasitic, fungal or other infection;
- Prompt within (24-48 hours) and complete response to corticosteroids and no relapse on withdrawal.
Chronic eosinophilic pneumonia (CEP)
Severe disease of insidious onset that typically is idiopathic, though can be secondary to known causes such as drugs, parasites, radiotherapy for breast cancer. CEP usually occurs in middle-aged patients, predominantly women (2:1 female/male ratio), non-smokers and with a history of atopy, asthma, and allergic rhinitis (Table 3). Response to steroid treatment is excellent, although clinical relapse occurs in 30–60% cases after steroid cessation.

Table 3: Clinical, laboratory and radiological findings of CEP.
References: Shared work of the authors
Diagnostic criteria:
- Respiratory symptoms present for at least 2 to 4 weeks;
- Eosinophilia at BAL >40% or peripheral blood eosinophils >1000/mm3;
- Diffuse pulmonary alveolar consolidation with air bronchogram and/or ground-glass opacities at chest imaging with peripheral predominance (Fig. 6, Fig. 7, Fig. 8);
- Absence of other known causes of eosinophilic lung disease.
Idiopathic Hypereosinophilic Syndrome (IHS)
Idiopathic hypereosinophilic syndrome is a group of heterogeneous disorders, characterized by marked, prolonged idiopathic eosinophilia and by variable organ dysfunction. It can affect multiple organ systems primarily because of the infiltration of mature eosinophils or secondarily to eosinophil-associated tissue damage. This disease mainly involves skin, heart, nervous system and hematological system (Table 4). Rheumatoid arthritis is sometimes associated with eosinophilia, leading to hypereosinophilic syndrome, although rheumatologic manifestations of IHS alone are infrequent (Fig. 9).

Table 4: Clinical, laboratory and radiological findings of IHS.
References: Shared work of the authors
Allergic bronchopulmonary aspergillosis
Allergic bronchopulmonary aspergillosis (ABPA) is a hypersensitivity reaction to Aspergillus antigens that is usually caused by Aspergillus fumigatus. ABPA is typically seen in patients with long-standing asthma or cystic fibrosis. ABPA can be suspected when asthma is accompanied by eosinophilia and suggestive radiological alterations, such as central bronchiectasis or pulmonary infiltrates (Table 5).

Table 5: Clinical, laboratory and radiological findings of ABPA.
References: Shared work of the authors
Diagnostic criteria:
- Presence of asthma with central bronchiectasis or pulmonary infiltrates (Fig. 10, Fig. 11, Fig. 12);
- Peripheral blood eosinophilia;
- Immediate positive skin test for Aspergillus antigens;
- Increased serum IgE levels (>1000 U/l);
Bronchocentric granulomatosis (BG)
A granulomatous disease, which is characterized by a necrotizing granulomatous inflammation of bronchial and bronchiolar epithelium with chronic inflammatory changes in the surrounding lung parenchyma. BG is related to asthma and the spectrum of allergic bronchopulmonary aspergillosis (Table 6).

Table 6: Clinical, laboratory and radiological findings of BG.
References: Shared work of the authors
Eosinophilic vasculitis
(aka Churg-Strauss syndrome) is a systemic disease associated with eosinophilia, asthma, eosinophil-rich and granulomatous inflammation and necrotizing vasculitis. Granulomatous inflammation involves the respiratory tract and small to medium vessels),. This syndrome most commonly affects lungs, followed by the skin. However, any organ can be involved, including the central nervous system, heart, and gastrointestinal tract (Table 7, Fig. 13).

Table 7: Clinical, laboratory and radiological findings of eosinophilic vasculitis.
References: Shared work of the authors
The diagnosis of eosinophilic vasculitis can be made if 4 or more of the following findings are present:
- Asthma;
- Eosinophilia >10% of the white blood cell differential count;
- Neuropathy;
- Migratory or transient pulmonary opacities (Fig. 14, Fig. 15);
- Paranasal sinus abnormalities;
- Extravascular eosinophils revealed at biopsy.
Differential diagnosis:
Differential diagnosis of various eosinophilic lung diseases is challenging due to non-specific clinical symptoms, overlapping CT features and similar laboratory findings (Table 8). While establishing the diagnosis, in order to narrow differential diagnosis, secondary causes of pulmonary eosinophilia must be considered and excluded. Therefore, integration of all the available information is mandatory for the precise diagnosis, including:
- Clinical information derived from the patient’s history, physical examination, duration and nature of the symptoms.
- Laboratory findings, especially the degree of BAL and peripheral eosinophilia. Other laboratory tests, such as stool examination and serologic testing, can be helpful in evaluating patients with specific conditions such as parasitic infection and ABPA.
- Pulmonary function tests are helpful in the evaluation of patients with unexplained pulmonary eosinophilia, while various eosinophilic lung disease demonstrate different ventilation defects.
- Imaging findings, including chest radiographs and CT, which frequently suggest or confirm the diagnoses.
- Lung biopsy may be used to confirm the diagnosis of bronchocentric granulomatosis and eosinophilic vasculitis syndrome. Meanwhile, in cases of other eosinophilic lung disease forms biopsy usually is not required.

Table 8: Differential diagnosis of eosinophilic lung disease.
References: Shared work of the authors