I. Pathologic Classification of Cystic Lesions (Fig. 2)
Injury/Inflammatory related cysts
- Pseudocysts and walled off necrosis
Neoplastic Cysts
- Serous cystadenoma/neoplasm (SCN)
- Mucin-producing lesions
- - Mucinous cystic neoplasm (MCN)
- - Intraductal papillary mucinous neoplasm (IPMN)
- Ductal adenocarcinoma with cystic features
Endocrine Lineage
- Cystic neuroendocrine tumors
Acinar Lineage
- Acinar lineage cystadenocarcinoma
Undetermined Lineage
- Solid pseudopapillary neoplasm (SPN)
Other Miscellaneous
- Lymphoepithelial cysts
- Squamoid cyst of pancreatic ducts
- Epidermoid cysts within the intrapancreatic accesory spleen
- Abscess
- Intraductal tubular carcinoma
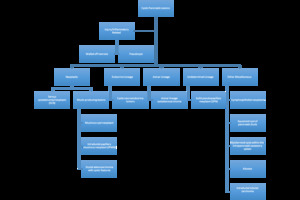
Fig. 2: Pathologic classification of cystic lesions of the pancreas.
References: Augusta/US
II. Characterization
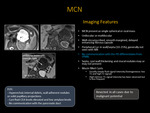
MR is the modality of choice as it provides superior contrast resolution
Cystic lesions characterized by:
- Type of fluid
- Cyst morphology and size (Fig. 3)
- Hemorrhage
- Septation/scar
- Soft-tissue components/nodularity
- Communication with the pancreatic duct
- Appearance of surrounding pancreatic parenchyma
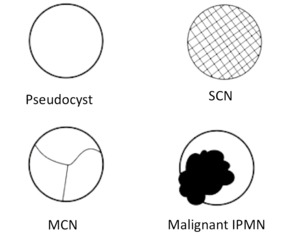
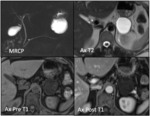
Fig. 3: Cystic changes characteristic of (top left) Pancreatic Pseudocyst: smooth walled cyst with encapsulation of the pancreatic secretions by granulation tissue and a fibrous capsule, (top right) Serous Cystadenoma/Neoplasm: honeycomb appearance (bottom left) Mucinous Cystic Neoplasm: Unilocular or multilocular appearance and (bottom right) Malignant IPMN: Unilocular or cluster of cysts (dilated ducts), lobulated margins.
References: Augusta/US
Patient demographics and clinical history are essential for diagnosis
III. Serous Cystadenoma/Neoplasm (SCN)
III-A. Background
III-B. Demographics/Presentation
- Older women (75% F, classicaly referred to as "Grandmother Lesions")
- Usually incidental and asymptomatic; if larger (>4cm) may cause symptoms of abdominal pain or jaundice (mass-effect/duct obstruction)
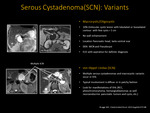
III-C. Imaging Features (Fig. 5, Fig. 6, Fig. 7, Fig. 8)
-
Microcystic lesion separated by fibrous septae radiating from central scar (honeycomb or cluster of grapes) with external lobulations
-
MR shows simple fluid signal intensity on T2-weighted images-lesion
-
Non-capsulated, Septae demonstrate progressive enhancement
-
Stellate, coarse Ca+ can be present in the central scar (30%), with a corresponding signal void - pathognomonic of SCN
-
DWI and ADC depend on amount of fibrous septa or fluid (not of much clinical utility)
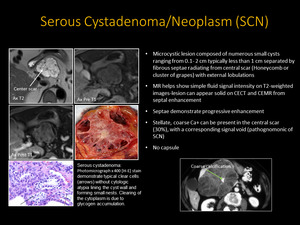
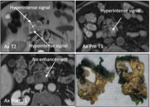
Fig. 4: Serous Cystadenoma/Neoplasm (SCN):
Serous cystadenoma: Axial T2 weighted MR image reveals fibrous septae radiating from a central scar ( white arrows). Coarse calcification visualized within central scar following contrast administration (green arrows).
References: Augusta/US
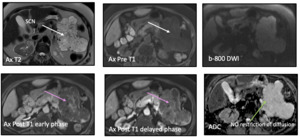
Fig. 5: Serous cystadenoma: 70-year-old female with history abdominal pain. Axial T2 weighted MR image reveals lobulated microcystic, T2 hyperintense and T1 hypointense mass in the tail of the pancreas (arrows). Progressively enhancing septae following contrast administration (pink arrows). On DWI, mass shows high ADC due to no restriction (green arrow).
References: Augusta/US
IV. Mucinous Cystic Neoplasm (MCN)
IV-A. Background
- Mucin producing neoplasm, predominantly affects body and tail
- 10% of cystic neoplasms
- Progesterone and estrogen receptor positive
- All have malignant potential (1/3 harbor invasive carcinoma)
- Cystic fluid high in CEA and low in amylase
- Risk factors for malignancy: (1) advanced age (2) tumor > 4cm (3) cyst wall irregularity (4) mural mass or nodules (5) high CEA
IV-B. Demographics & Presentation
- Exclusively in women, 40-50 years in age ("Mother Lesion")
- 30% of patients asymptomatic
- Symptomatic patients: abdominal pain, palpable mass, weight loss, fatigue, anorexia, and jaundice
- May present with pancreatitis
- Resected in all cases due to malignant potential
- IV-C. Imaging Features ( Fig. 9, Fig. 10, Fig. 11 and Fig. 12)
- Single spherical or oval mass
- Unilocular or multilocular
- Well-circumscribed, smooth margined, delayed enhancing fibrous capsule
-
Peripheral Calcification in wall/septa (10-25%), not seen with MR
-
No communication with the PD differentiates from IPMN
-
Mucin filled Cysts: usually simple fluid signal intensity (homogenous low T1 and high T2 signal)
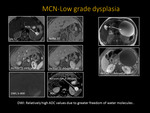
- Relatively high ADC values due to greater freedom of water molecules
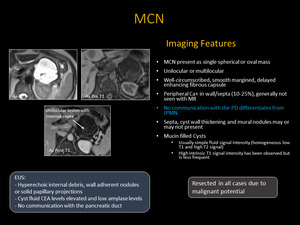
Fig. 10: MCN
References: Augusta/US
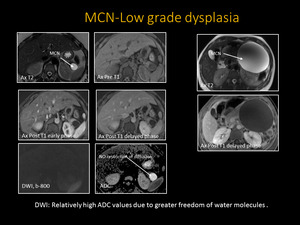
Fig. 11: Mucinous Cystic Neoplasm: Axial T2 weighted MR image reveals homogenous, fluid-filled T2 hyperintense and T1 hypointense mass in the tail of the pancreas (arrows). Axial T1 post-contrast images re-demonstrates the non-enhancing, unilocular lesion. The same mass demonstrates no diffusion restriction and high signal on ADC (arrows).
References: Augusta/US
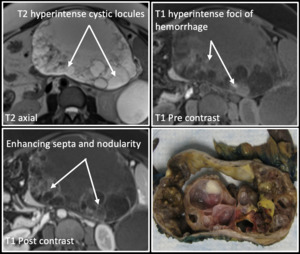
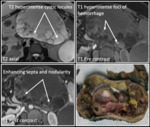
Fig. 12: Mucinous Cystic Neoplasm with Invasive Adenocarcinoma: Axial T2 weighted MR image reveals heterogeneous, T2 hyperintense and T1 hypointense mass within the pancreas containing cystic locules (arrows). Axial T1 images demonstrate hyperintense foci of hemorrhage and septa that enhance with contrast (arrows). A surgically resected specimen demonstrates similar findings.
References: Augusta/US
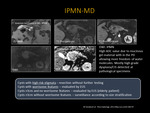
V. Intraductal Papillary Mucinous Neoplasm (IPMN)
V-A. Background
- Mucinous cystic lesions of the main pancreatic duct or side branches
- Usually in the head of the pancreas, 20-30% multifocal, 5-10% diffuse pancreatic involvement
- High CEA in cystic fluid
V-B. Demographics & Presentation
- Mean age 65, 60% male ("Granfather Lesion")
- Most commonly asymptomatic and discovered incidentally on routine imaging, some patients may present with symptoms of pancreatitis.
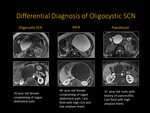
V-C. Classification
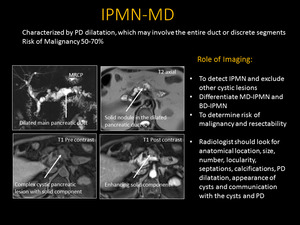
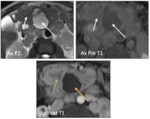
Fig. 13: Main Duct Intraductal Papillary Mucinous Neoplasm: Axial T2 weighted MR image demonstrating a solid nodule within the PD (arrows). Axial T1 weighted MR image re-demonstrates complex, cystic pancreatic lesion with a solid component that enhances with contrast. MRCP showing dilation of the main PD (arrows) representing a main duct IPMN.
References: Augusta/US
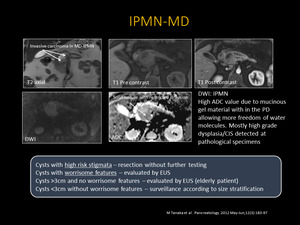
Fig. 14: DWI solid pancreatic nodule with diffusion restriction. High ADC value due to mucinous gel material with in the PD allowing more freedom of water molecules.
References: Augusta/US
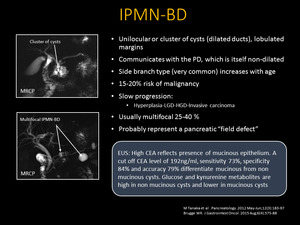
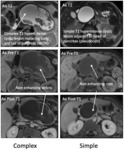
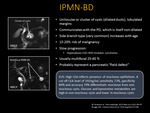
Fig. 15: Branch Duct IPMN: MRCP showing a cluster of cysts (dilated ducts) with lobulated margins that communicates with the PD, which itself is not dilated (top image) 25-40% of Branch Duct IPMNs are multifocal as seen in the bottom image that demonstrates multiple unilocular lesions communicating with the PD in the absence of pancreatic ductal dilation (bottom image).
References: Augusta/US
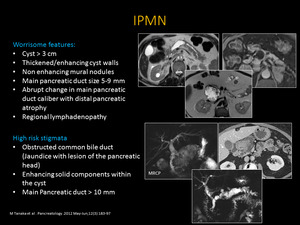
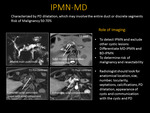
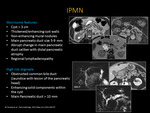
Fig. 16: IPMN
Worrisome features and High risk stigmata
References: Augusta/US
V-D. Imaging Features (Fig. 13, Fig. 14, Fig. 15, Fig. 16)
- T2 hyperintense complex, solid and/or cystic lesion with lobulated margins
- T1 hypointense with solid components that enhance with contrast
- MRCP to differentiate main-duct and branch-duct IPMNs
- High ADC value due to mucinous gel material with in the PD allowing more freedom of water molecules (Fig. 14)
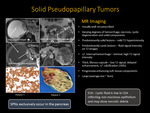
VI. Solid Pseudopapillary Neoplasm (SPN)
VI-A. Background
VI-B. Demongraphics & Presentation
-
Young (mean age is 25), 96% female
-
All suspected Solid pseudo-papillary tumors are managed surgically
VI-C. Imaging Features (Fig. 17 and Fig. 18)
- Usually well circumscribed, large (average size ~9cm)
-
Varying degrees of hemorrhage, necrosis, cystic degeneration and solid components
-
Predominantly solid lesions – mild T2 hyperintensity
-
Predominantly cystic lesions – fluid signal intensity on T2 images
-
+/- Internal hemorrhage – intrinsic high T1 signal intensity
-
Thick, fibrous capsule – low T2 signal, delayed enhancement, +/- calcification (30%)
-
Progressive enhancing soft-tissue components
-
Solid component – Low ADC, Cystic component – High ADC
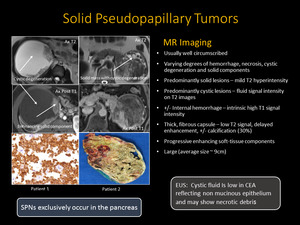
Fig. 17: Solid Pseudopapillary Tumors
References: Augusta/US
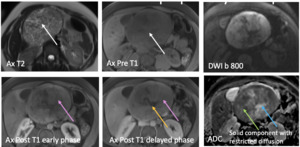
Fig. 18: Solid pseudopapillary neoplasm: 26 -year- old female with history of abdominal pain . Axial T2 weighted MR image reveals predominantly solid mass in the head of pancreas (white arrow) with T2 hyperintense areas due to necrosis/cystic degeneration and corresponding precontast T1weighted image shows intermediate signal (black arrow) . Following contrast administration mass show progressive enhancement (pink arrows) with areas of non enhancement due to cystic degeneration (yellow arrow). On DWI, soild portion of the mass shows low ADC due to restriction (green arrow) where as cystic components show high ADC (blue arrow).
References: Augusta/US
VII. Ductal Adenocarcinoma with Cystic Features
VII-A. Background
- Most common pancreatic neoplasm (85-90%)
- High mortality, overall 5-year survival of 4% (resectable 25%, uresectable 1%)
- Although predominately solid, cyst-like features (cystic degeneration/necrosis, retention cysts, side-branch ductal obstruction or attached pseudocysts) in ~8%
VII-B. Imaging Features (Fig. 19 and Fig. 20)
- Best imaged with MR
-
Hypoenhancing with progressive delayed enhancement
-
Pathology correlates: poorly vascularized, infiltrative, fibrotic tumor with surrounding desmoplastic reaction
-
Location: 2/3 pancreatic head, 5-15% body, 10-15% tail
-
Associated with ductal obstruction, either CBD, PD or both (MRCP & T2WI)
-
Keys to differentiate from other solid lesions with cystic features: (1) Infiltrative pattern, (2) ductal obstruction, (3) vascular invasion
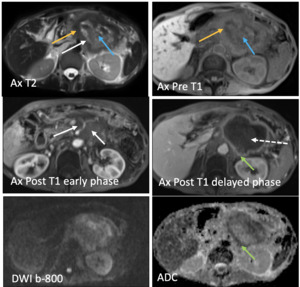
Fig. 19: Pancreatic adenocarcinoma: 79-year-old female with history left upper quadrant pain. MRI of the abdomen demonstrates heterogeneous infiltrating mass involving body and tail of pancreas with central hyperintense T2 and hypointense T1 signal due to necrosis (blue arrows), T2 hypointense and intermediate T1 signal thick rind of soft tissue (yellow arrows) that shows enhancement following contrast administration and restricted diffusion due to dark ADC (green arrows) and no enhancement of central aspect due to necrosis (dashed arrow). The mass encases the celiac axis, hepatic artery and splenic artery by 360 degrees (white arrows).
References: Augusta/US
VIII. Cystic Neuroendocrine Tumors
VIII-A. Background
- Cyst fluid low in CEA and amylase
- Cells positive for chromogranin and synaptophysin
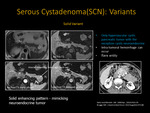
VIII-B. MR Imaging Features (Fig. 21)
-
Small Lesions : Homogenously T1 hypointense and T2 hyperintense
-
Robust arterial enhancement (rich capillary network and vascular supply)
-
Larger lesions have increased heterogeneous appearance (hemorrhage and cystic change)
-
Cystic NET: 90% hypervascular rim, nonfunctional (80%)
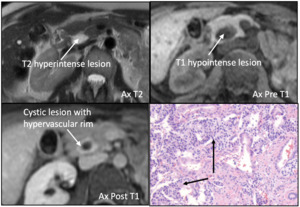
Fig. 21: Neuroendocrine tumor: Axial T1 and T2 weighted MR images show homogeneously T1 hypointense and T2 hyperintense cystic lesion (white arrows). Axial T1 weighted MR also demonstrates a hypervascular rim that enhances with contrast (white arrows).
Photomicrograph x 100 [H-E] stain demonstrates interface between normal pancreas in the lower portion of the slide and neuroendocrine tumor on the top ( black arrows) the tumor cells are forming nests and show monotonous cells with pink granular cytoplasm.
References: Augusta/US
IX. Lymphoepithelial Cysts
IX-A. Background
- Rare (<1% of all pancreatic cysts)
- Benign
-
Usually middle aged men (mean age 55 years, M>F 4:1)
-
Lined by squamous epithelium, filled with keratinaceous debris and surrounded by a band of dense lymphoid tissue
IX-B. MR Imaging Features
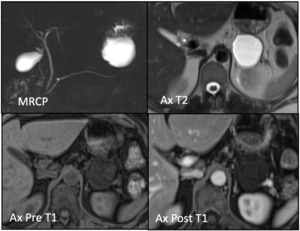
Fig. 22: Unilocular Lymphoepithelial Cyst: Axial T2 weight MR image showing T2 hyperintense and T1 hypointense unilocular cyst in the tail of the pancreas, that does not enhance with contrast. MRCP:
References: Augusta/US
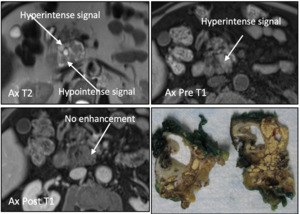
Fig. 23: Multilocular Lymphoepithelial Cyst: Axial T2 weight MR image showing a heterogeneous cystic lesion with T2 hyperintense and hypointense components (arrows). The same lesion demonstrates T1 hyperintensity without contrast enhancement (arrows). Surigcally resected specimen shows a heterogeneous mass filled with keratinaceous debris.
References: Augusta/US
X. Walled off Necrosis/Pseudocyst
X-A. Background
- Occurs in the setting of pancreatitis
- Walled off necrosis - hemorrhagic fat necrosis with encapsulation of the pancreatic secretions by granulation tissue and a fibrous capsule
- No epithelial lining
X-B. Management
- 4-6 week follow-up, should evolve over short intervals (other cysts persist without significant change)
- Can resolve spontaneously
- Complications: (1) hemorrhage, (2) infection, (3) rupture, (4) mass effect
- Complicated or symptomatic cysts may require surgical, percutaneous, or endoscopic drainage
X-C. MR Imaging (Fig. 24)
-
Irregular cyst(s) in/next to the pancreas that evolves within weeks
-
Irregular margin early, well circumscribed later (thick enhancing wall of granulation tissue and fibrosis)
-
Internal blood products (high T1 signal)
-
Dependent necrotic or proteinaceous debris (nonenhancing, low T2 signal)
-
Soft-tissue elements should never enhance
-
Other changes of acute/chronic pancreatitis (e.g. fibrosis, atrophy, dilated PD, SV thrombosis, parenchymal calcification)
-
May dissect along fascial planes to remote sites (e.g. liver, pleura, or even mediastinum)
-
May fistulize with vascular structures
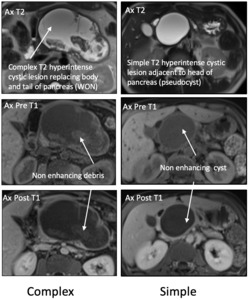
Fig. 24: Complex Walled off Necrosis (Left): Axial T2 weighted MR image showing complex T2 hyperintense cystic lesion replacing the body and tail of the pancreas with T2 hypointense proteinaceous debris (arrow). Axial T1 weighted MR image showing T1 hypointense heterogeneous cystic lesion filled with non-enhancing debris that does not enhance with contrast (arrow).
Simple Pseudocyst (Right): Axial T2 weighted MR image showing homogeneous and well-circumscribed T2 hyperintense cystic lesion. Axial T1 weighted MR image showing homogeneous and well-circumscribed T1 hypointense cystic lesion that does not enhance with contrast (arrows).
References: Augusta/US
XI. Acinar Cell Cystadenocarcinoma
XI-A. Background
- 1-2% of exocrine neoplasms (produce pancreatic enzymes - trypsin and lipase)
- Malignant, frequently metastatic at presentation
- Poor prognosis, 5-year survival of 6%
XI-B. Demographics & Presentation
- Mean age 58, M>F (2:1)
-
Lipase hypersecretion syndrome in 10-15%
-
Elevated lipase levels causing fat necrosis, subcutaneous nodules and polyarthritis
XI-C. MR Imaging Features (Fig. 25)
- Large (>10 cm)
- Hypoenhancing
- Varying degrees of necrosis with cystic change
- Well-marginated with surrounding capsule
- May have intratumoral calcification and hemorrhage
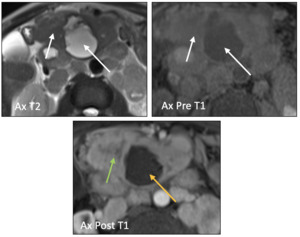
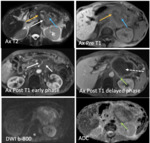
Fig. 25: Acinar Cell Cystadenocarcinoma: 54 -year- old male with history abdominal pain. MR axial T2 and precontrast T1 weighted images demonstrate a large lobulated heterogeneous hypointense and intermediate signal mass, respectively (white arrows), with central T2 hyperintense and T1 hypointense necrosis (black arrows) involving the pancreatic head. Post contrast T1 weighted image shows heterogeneous enhancement of solid mass (green arrow) and no enhancement of central aspect (yellow arrow). Biopsy showed (acinar cell carcinoma.)
References: Augusta/US



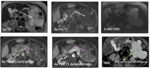

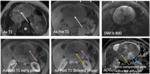
![Fig. 20: Pancreatic adenocarcinoma: 68 -year- old male with history abdominal and back pain. Axial T2 weighted MR image reveals heterogeneous mass in the head of pancreas with cystic degeneration (yellow arrow) and corresponding precontast T1weighted image shows intermediate signal (white arrow). Following contrast administration, the mass shows heterogenous enhancement (pink arrow) with areas of non enhancement due to cystic degeneration (blue arrow). Photomicrograph x 40 [H-E] stain demonstrate haphazard and infiltrative growth of malignant glands, some glands contain necrotic debris, and a back ground of desmoplastic stroma. Black arrow indicates malignant glands, with necrosis in the center. Red arrow indicates desmoplastic stroma.
References: Augusta/US](https://epos.myesr.org/posterimage/esr/ecr2020/155059/media/847043?maxheight=150&maxwidth=150)
![Fig. 21: Neuroendocrine tumor: Axial T1 and T2 weighted MR images show homogeneously T1 hypointense and T2 hyperintense cystic lesion (white arrows). Axial T1 weighted MR also demonstrates a hypervascular rim that enhances with contrast (white arrows).
Photomicrograph x 100 [H-E] stain demonstrates interface between normal pancreas in the lower portion of the slide and neuroendocrine tumor on the top ( black arrows) the tumor cells are forming nests and show monotonous cells with pink granular cytoplasm. References: Augusta/US](https://epos.myesr.org/posterimage/esr/ecr2020/155059/media/847053?maxheight=150&maxwidth=150)