Obesity has become a main public health problem as the number of obese children and adolescents increases rapidly. It is associated with significant medical problems in adolescence, like hypertension, coronary artery disease, and diabetes mellitus.
Obesity can affect radiology in several ways:
1. The weight of the patient may exceed the imaging equipment limits.
2. Increased body circumference may result in insufficient contrast resolution .
3. Longer exposure to radiation may be necessary to image obese children with the increase in dose.
4. The appropriate dose of contrast material may be difficult to be calculated.
5. Increased body weight gives bad ultrasound images.
Different radiological techniques used nowadays in the evaluation of obesity in Children includes:
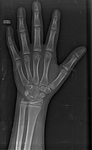
1.Bone age assessment
Obese children have enhanced linear growth, often accompanied by an advanced bone age and a decreased pubertal growth spurt compared to lean children of the same age.
Methods:
- The commonest way to calculate bone age is plain radiography of left hand and wrist. It is done by comparing the left wrist radiographs with the nearest matching reference radiographs provided within an atlas with standard radiographs for different ages. Obese children will show increased bone age.
- Ultrasound seems not accurate in children. MR imaging is noninvasive but it takes more time and bone age assessment using MR imaging is still new.
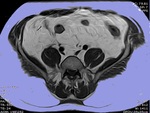
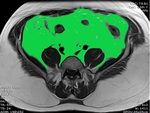
2.Visceral fat assessement:
Visceral fat accurate assessment is very important clinically, as it is associated with metabolic syndrome components.
Methods
Visceral fat can me measured using either MRI, ultrasonography or DEXA:
- MRI: MRI measurment of visceral fat are more accurate than conventional anthropometric indices, with the advantage of low radiation. The precise measurements of regional adipose tissue as well as diffuse fat infiltration of organs, can be done using ‘quantitative fat water imaging’ . The basis of which is the separation of fat and water using Dixon imaging, depending on the differencies of frequencies of protons in fat and water, giving color coded maps for the subcutaneous fat and visceral fat.
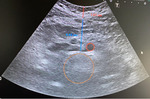
- Ultrasound: Visceral fat thichness is defined as the thickness of fat tissue between the linea alba and aorta, and subcutaneous fat is defined as fat tissue thickness from the skin-fat interface to the linea alba. The procedure is usually done with using 7.5- and 3.5-MHz probes.
- Dual-energy X-ray (DEXA): Uses X-rays with two different energies that can separate the body into two components. The X-ray attenuation depends on both the thickness of the tissue and the tissue’s attenuation coefficient. Output measurements can include total body fat, lean tissue, and bone mineral content. It is more accurate than density-based methods for estimating total body fat. It gives a 2D image in coronal view that estimates regional fat content using anatomic maps.
3. Non-alcoholic fatty liver disease assessment (NAFLD):
Although liver biopsy is the gold standard for diagnosis, non-invasive imaging methods are rapidly developing and may replace biopsy in many circumstances.
Technique
|
Well established
|
New
|
|
Conventional ultrasonography
|
Ultrasound elastography
|
|
CT scan
|
Quantitative ultrasound techniques
|
|
Conventional MR imaging
|
Magnetic Resonance Elastography
|
|
|
Magnetic resonance-based fat quantitation techniques
|
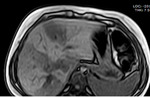
- Ultrasonography:Steatosis appears as hyperechoic liver parenchyma with tightly packed fine echoes and posterior beam attenuation. The severe form shows difficult visulaization of intrahepatic vesseles due to increased parenchymal echogenicity. Severe fatty liver, (containing >30% fat by weight), can be suspected with a very high sensitivity and specificity.
- CT detects hepatic steatosis through the measurement of liver attenuation. Hepatic steatosis is suggested on unenhanced studies when liver attenuation is at ≤10 Hounsfield units (HU) below that of the spleen, by the presence of heterogeneous liver attenuation and by “pseudoenhancement” (relative high density of the hepatic vessels compared with surrounding parenchyma), and on post-contrast CT by a lower attenuation of the liver than the spleen by a difference of >20 HU, or by liver attenuation that is lower than muscle. CT is not sensitive in detecting mild elevations of hepatic lipid content (5% to 30%).
- MRI is a sensitive technique for the quantification of liver fat.
- The most commonly used quantitative method is in- and out-of-phase imaging. Reduced signal on out-of-phase T1-weighted(T1W) images is an accurate proxy of histologic hepatic fat content. An important pitfall is the presence of iron overload that can result in an underestimation of liver fat.
- MR spectroscopy (MRS) has been found to correlate with hepatic lipid content. This technique is sensitive to small variation (≤0.5% change) in hepatic lipid content and has the potential to assess for small changes in steatosis due to treatment.
Different radiological procedures in the postoperative assessment of bariatric surgeries.
Bariatric surgery has emerged as an important option in treatment of obesity.
Radiology plays an important role in the evaluation of the post-operative bariatric patient.
|
Surgery type
|
Roux-en-Y
|
Laparoscopic adjustable gastric banding
|
|
D1 post-operative
|
Ø Initial gastrograffin fluoroscopic imaging study to evaluate for anastomotic leak
|
Ø The gastric pouch size is assessed fluoroscopically for leakage, and for normal contrast passage through the stoma.
-When distended with contrast material the gastric pouch should be from 3 to 4 cm symmetrically and maximally.
-Within 15 to 29 min post administration the stoma diameter measures 3 to 4 mm allowing passage of whole contrast material.
|
|
Complications
|
Ø CT can show:
-Contrast leakage
-intra-abdominal collections or abscess formation.
Ø Fluoroscopy can used to view stricture, or narrowing of the anastomotic site with expansion of the proximal gastric pouch and delayed transit of contrast into the Roux limb.
|
Slippage is assessed by the phi angle, it is the intersection between lines parallel to the spinal column and antero-posterior plane of the gastric band. Normal angle is from 4° to 58° and 4 to 5 cm below the hemidiaphragm. herniation of the distal stomach either anterior or posterior through the band makes the phi angle more or less than normal respectively.
Band system leakage may occur at the level of the band, connector, tubing, or access port. The leak can be detected when adjusting the band diameter under fluoroscopy.
A 99mTc-albumin study can prove useful in locating the leak.
|