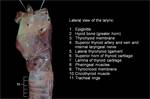
The larynx is the part of the respiratory system where it divides from the digestive tract. Anatomically it is considered the first part of the inferior respiratory system, but clinically it is usually called superior airway from the nasal cavity to the end of the trachea.
Its complexity is derived from its multiple functions:
- Air conduction to the trachea
- Closing of the respiratory system during Valsalva maneuvers
- Phonation
- Protection of the inferior respiratory system from aspiration during swallowing
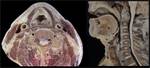
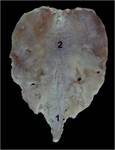
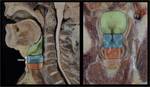
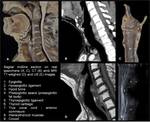
The larynx is located anteriorly inside the visceral space of the neck (figure 2). In adults, it projects in front of C4-C6 vertebrae. In newborns below 12-18 months, it is located higher, anterior to the axis (figure 3).
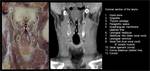
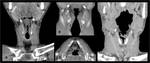
Cranially it attaches with the hyoid bone, at the base of the tongue. It continues caudally with the trachea. Its posterior aspect is enclosed by the laryngopharynx, also called hypopharynx. Anteriorly it is only covered by a few prelaryngeal infrahyoid muscles, fascial layers and the uppermost aspect of the thyroid gland, being easily accessible through palpation (figures 2-5).
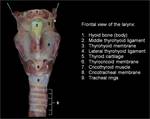
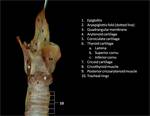
The larynx has a cartilaginous skeleton (figures 6-9), joined by multiple articulations, ligaments and membranes (figure 10). It has intrinsic and extrinsic muscles that activate its movements and an inner mucosal cover that delimitates the internal spaces of the larynx.
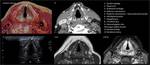
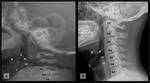
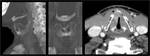
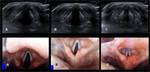
Its cartilages can undergo enchondral calcification and ossify through the life, beginning in the 3rd decade and ending around 65 years (figures 11-12). The laryngeal calcifications present significant anatomical variability adding layers of complexity in the evaluation of tumoral infiltration (figures 13-16). In the absence of calcifications, ultrasound can be used to asses true vocal cord motility (figures 17-19).
Clinically, the larynx is subdivided into three compartments: supraglottis, glottis and subglottis (figure 20). This subdivision is particularly relevant in the staging of laryngeal tumors.
SUPRAGLOTTIS:
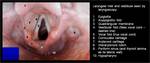
Supraglottis is defined as the space included from the epiglottis to the superior surface of the true vocal cords (at the junction with the lateral wall of the laryngeal ventricle).
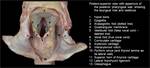
The laryngeal inlet (figure 21 and 22) is the opening formed by the free edge of the epiglottis, the free edge of the aryepiglottic folds and the interarytenoid notch. The inner space of the supraglottis is called laryngeal vestibule. While swallowing, the epiglottis is pulled down to close the laryngeal inlet, at the same time that all the larynx is moved upward increasing the pharyngolaryngeal angle. Then epiglottis serves as a breakwater, to deflect fluids to the oesophagus.
Anteriorly, the epiglottis is attached to the hyoid bone by the hyoepiglottic ligament and to the thyroid cartilage by the thyroepiglottic ligament. The fat-filled space comprised between the lingual surface of the epiglottis, hyoid bone, thyrohyoid membrane and superior aspect of the thyroid cartilage is the pre-epiglottic space (figure 23).
The aryepiglottic folds, which are the supraglottis lateral walls, are formed by the quadrangular membrane (figures 10, 21-22), covered by some muscular fibers (from the aryepiglottic and thyroepiglottic muscles) and the mucosa. The quadrangular membrane is anteriorly attached to the lateral rim of the epiglottis and posteriorly to the corniculate cartilage and apex of the arytenoid cartilage. Its free superior border is the free edge of the aryepiglottic fold and contains the cuneiform cartilage. Its free inferior border forms the vestibular fold (false vocal cord).
Between the false and true vocal cords, there is a little gap where the mucosa protrudes outward, forming the laryngeal ventricle (figure 24). Sometimes it continues upwards between the quadrangular membrane and thyroid cartilage (paralaryngeal space), forming the laryngeal saccule. When it dilates, it forms a laryngocele (internal or simple), which can even herniate through the thyrohyoid membrane (external laryngocele) (figure 25).
GLOTTIS:
The glottis is comprised of the superior surface of the vocal folds to 1 cm below this point.
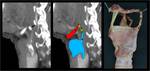
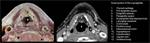
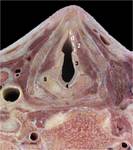
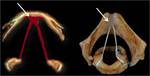
Its lateral walls are formed by the superior part of the conus elasticus (cricovocal membrane), a cone-shaped membrane with its base attached to the cricoid ring and the superior rim forming the vocal ligament, which runs from the posterior aspect of the thyroid prominence to the vocal process of the arytenoid (figures 1 and 27-28). The vocalis muscle surrounds the vocal ligament and the mucosa recovers it, conforming the vocal fold (true vocal cord).
The anterior commissure represents the anterior point of junction of the vocal folds. At this point also joints the thyroepiglottic ligament, forming the Broyle ligament (figure 28). The inner perichondrium is absent at the site at which Broyle ligament inserts into the thyroid cartilage, which makes the cartilage vulnerable to cancer invasion.
Posteriorly, the space between the arytenoid cartilages is called posterior commissure (figures 22, 24 and 26). It contains interarytenoid muscles (oblique and transverse arytenoid muscles) and closes the glottis during phonation.
The fat-filled space comprised between the internal aspect of the thyroid cartilage and the conus elasticus is the paraglottic space (figures 24 and 26).
SUBGLOTTIS:
The superior margin of the subglottis is a histological transition from the vocal cord squamous epithelium to the subglottic respiratory epithelium. Clinically, it is defined to be 1 cm below the joint of the laryngeal ventricle and the superior surface of the true vocal cord (some authors define it as 5 mm below the free margin of the true vocal cord).
Its diameter enlarges as the conus elasticus progress caudally (figure 24). Inferiorly it is bounded by the inferior margin of the cricoid cartilage.
The paraglottic space is still present at the subglottis level, located between the conus elasticus and the thyrocricoid membrane and cricoid cartilage until they joint inferiorly.