Vestibular schwannomas
Vestibular schwannoma is a benign encapsulated tumor that arise from the Schwann cells of the nerve sheaths of cranial and spinal nerves.[5].
The majority (95%) of solitary lesions are sporadic. Bilateral vestibular schwannomas are highly suggestive of  neurofibromatosis type 2 (NF2), a neurocutaneous disorder associated with a mutation of chromosome 22 [6].
neurofibromatosis type 2 (NF2), a neurocutaneous disorder associated with a mutation of chromosome 22 [6].
Symptoms
The typical presentation is sensorineural unilateral hearing loss or non-pulsatile tinnitus. However, the symptom of vestibular schwannomas depends upon the size and location of the tumor: in the intracanalicular stage it may present as a unilateral sensorineural hearing loss, tinnitus, or vertigo; in cisternal stage it worsens the hearing loss, tinnitus, disequilibrium, and possible headache; when tumor progresses further, it compresses the brainstem and trigeminal symptoms may also develop [4]
MR appearance
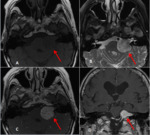
On MR images the schwannoma is a round or tubular mass, growing inside the internal acoustic canal and widening it, forming an acute angle with the petrous bone ("Ice cream on cone" appearance).
On T1-w sequences, they can be Iso- to hypointense with intense homogeneous contrast-enhancement post gadolinium infusion [7].
On T2-w images, they usually become hyperintense, whereas most meningiomas remain hypo- or isointense. However, these signal intensity differents are not pathognomonic for schwannoma.
In larger tumors, intratumoral degenerative changes, like hemorrhagic and cystic areas, may result in an increase in heterogeneity of signal.
Meningioma
Meningiomas are solid, well-circumscribed, globular or lobulated, vascular tumor that are composed arising from arachnoidal cells with a broad attachment to the adjacent dura [8].
Meningiomas occur preponderantly in females(female-to-male ratio 2:1).
The WHO classifies meningiomas into three grades: Benign (Grade I), atypical (Grade II), and anaplastic or malignant (Grade III). Most meningiomas are benign (Grade I) tumors [9]
Multiple meningiomas are commonly associated with NF-2.
Symptoms
Many small meningiomas are found incidentally and are asymptomatic. Often they cause vague symptoms, like headaches.Larger tumors become clinically apparent with paresis, change in mental status and other symptoms due to mass effect depending on their location.
MR appearance
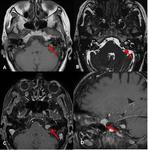
On MR image, the majority of meningiomas is an oval or hemispheric non intracanalicular meningeal mass with broad base, forming an obtuse angle with the petrous bone.
On T1W sequences, they appear iso- to hypointense with intense homogeneous enhancement. On T2W sequnces, about 50% are mildly hyperintense and 50% are isointense to the cortex [10].
Look for the ”dural tail” sign (linear enhancement along the dura matter on either side of the tumor), calcifications and pial vessel flow voids.
Because a major prognostic factor in the recurrence of meningiomas after surgery is the extent of tumor resection, the careful assessment must be made of pre- and post-operative contrast MR images for the presence of a dural tail [5]
Epidermoid cyst
Epidermoid cysts are congenital intradural lesions arising from the inclusion of ectodermal epithelial elements during neural tube closure [12].
Their content comes from desquamated epithelial cells and mimics CFS.
Symptoms
Epidermoid cysts typically present in middle age due to gradual mass effect on adjacent structures: headaches, cranial nerve deficits, cerebellar symptoms and seizures. Rupture can produce aseptic meningitis.
MR appearance
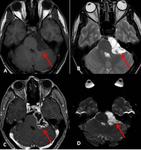
Epidermoid cysts typically show undulating and irregular margins, model their shape to conform to the CPA and grow around nerves and blood vessels.
On MR images they are iso-intense to CFS on T2-w and T1-w sequences. More specifically, the T1W signal intensity tends to vary with the lipid content, with the signal intensity being increased in lesions with a high lipid content.
Diffusion MR imaging sequence is the most important sequence in differential diagnosis: epidermoid cyst shows restricted diffusion on DWI.
Margins are usually irregular and they usually do not enhance with gadolinium (a peripheral enhancement is uncommon) and do not bleed [13].
Other lesions
Arachnoid cyst
Arachnoid cysts are benign, congenital, loculated collections of CSF lesions within arachnoidal membrane [14].
They may be asymptomatic, incidental findings, but they can produce the typical symptoms of a CPA mass, including hemifacial spasm [15]
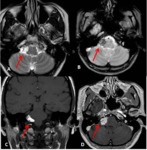
On MRI, arachnoid cysts appear as well-defined nonenhancing intracranial masses that follow CSF intensity on all sequences. Arachnoid cysts and epidermoid cysts may have similar characteristics on T1W and T2W sequences. However, arachnoid cysts follow CSF signals on all sequences, in particular on the DWI, unlike epidermoid cysts that show restricted diffusion on DWI.
Lipoma
Lipomas are anomalously developed masses that arise from abnormal differentiation of the meninx primitive[16].
They often are asymptomatic. When they are along the course of the vestibulocochlear nerve they cause neurosenrial hearing loss.
Signal intensity is similar to the fat on all sequences: hyperintense on T1-w images; intermediate signal on T2-w images; "disappear" on fat-saturated sequences [17]
Aneurysm
Aneurysms of the CPA (dilatation of vertebral or basilar artery) may be manifested with symptoms of brain stem compression rather than with subarachnoid hemorrhage.
They typically show a signal void on all MR images. However, the MR imaging appearance of larger aneurysms can be complex due to flow vortices or internal thrombus (the appearance depends on the age of clot within the lumen). [18]
Intra-axial tumors
Medulloblastoma is hypointense on T1W sequences and hyperintense on T2W sequences, it give intense postcontrast enhancement.
Ependymoma is iso- or hypo-intense on T1-w sequnces with heterogeneous postcontrast enhancement, and hyperintense on T2W sequences; calcifications and hemorrhage are common [4].