Wernicke's encephalopathy is an acute thiamine or vitamin B1 deficiency neurological syndrome. In most cases, it is related to alcohol consumption, although some cases have been reported in children and adults secondary to pathologies that alter the absorption of thiamine such as starvation, postbariatric surgery, and anorexia/bulimia. [1-2]
Under normal conditions, thiamine maintains the intracellular osmotic gradient, and its deficiency generates cytotoxic oedema in astrocytes and neurons, with the subsequent development of vasogenic oedema and neuronal death. [2]
Its classic triad is ataxia, ophthalmoplegia, and altered level of consciousness, although only 38% of patients presented with this clinical triad, being difficult to diagnose.
In magnetic resonance imaging, the alteration of signal intensity associated with cytotoxic oedema is typical and is classified in two stages: early and late.
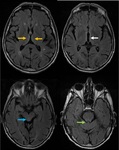
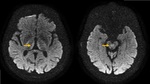
In the early stage, symmetrical hyperintensities visualized in T2, FLAIR, and diffusion distributed in the thalamus, mammillary bodies, hypothalamus, walls of the third ventricle, and periaqueductal gray matter, findings that are reversible after thiamine intake. ( Fig. 1 Fig. 2 ). [1-2].
The enhancement of the mammillary bodies after contrast administration is frequent in alcoholic patients and maybe the only finding.
In the late stage, atrophy of the mammillary bodies and dilation of the third ventricle may be objected [1]
Its differential diagnosis includes ischemic (artery of Percheron infarction, top of the basilar infarction), infectious/inflammatory (ADEM, Creutzfeldt-Jakob disease), and toxic causes (carbon monoxide, heroin, metronidazole-induced encephalopathy) [2]