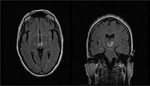
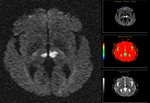
Artery of Percheron infarction: Synchronous infarction of both thalamus, with or without rostral mesencephalic involvement. Prevalence unknown and usually secondary to cardiac embolism. The classic triad of Percheron artery occlusion includes vertical gaze paralysis (65 %), memory impairment (58 %), and coma (42 %). There are four distinct patterns of Percheron artery infarction:
The pattern I: bilateral paramedian thalamic with rostral midbrain (43 %), Pattern II: bilateral paramedian thalamic without midbrain (38 %) ( Fig. 3, Fig. 4 ), Pattern III: bilateral paramedian and anterior thalamic with midbrain (14 %), and Pattern IV: bilateral paramedian and anterior thalamic without midbrain (5 %). [3]
Creutzfeldt-Jakob Disease: Spongiform encephalopathy in most cases of sporadic aetiology, although familial forms have also reported. It is characterized by progressive dementia accompanied by myoclonus, brain atrophy and death. Radiological findings include cortical, white-matter or basal ganglia (putamen, caudate and thalamus) T2 hyperintensities ( Fig. 5 ), which restrict in diffusion. The findings can be uni or bilateral and symmetric or asymmetric. [4]
Deep cerebral venous thrombosis: This is the great mimicker of other diseases. It can occur at any age, but women and children are at a higher risk of being affected. Its clinical presentation may be nonspecific, and in most cases, the clinical onset is less abrupt, and the progression occurs over days mimicking the time course of intracranial infection.
Venous thrombosis typically begins in a dural venous sinus, and it may progress to involve other portions of the dural venous system or extend into adjacent cortical veins.
The use of heparin to dissolve venous clots or endovascular treatment often results in dramatic improvement, so an understanding of the imaging diagnosis is essential.
CT findings are nonspecific and make diagnosis difficult. In MRI, hyperintensity of the thalamus and basal ganglia can be observed, and the absence of flow can be visualized in the venogram. ( Fig. 6, Fig. 7, Fig. 8 ) [4]
Metronidazole encephalopathy: This is a rare entity that can appear at any age with a peak incidence between the fifth and sixth decades of life. It occurs with an average time of 54 days of use of the drug and is characterized by cerebellar dysfunction (dysarthria, ataxia, dysmetria and nystagmus) and/or seizures.
In most cases, signal alteration is observed at the level of the cerebellum, dentate nucleus, corpus callosum, midbrain, protuberance, and medulla.
When the drug is discontinued, most patients cynically improvement. ( Fig. 9 Fig. 10 ). [5]