In this educational exhibit, we will review some typical radiological findings in different clinical scenarios, indicating the need for pretransplant NKN.
Massive kidney enlargement: limited space for the graft
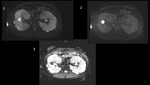
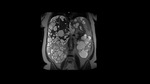
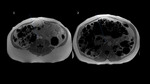
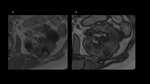
Among ADPKD transplant candidates, there are significant individual differences regarding kidney size.[Fig.1] The remaining space in the abdominal cavity may be insufficient for graft implantation, which poses an obstacle for the surgeon as making the procedure technically difficult or impossible.
The incorrect, negative decision regarding qualification for the pretransplant NKN can contribute to an excessive rise in intra-abdominal pressure after transplantation.[3] Graft compression leads to parenchymal hypoperfusion, resulting in its dysfunction.[4]
Based on images, we can assess how much space is available for the transplant with much greater precision than from physical examination. We can also tell which kidney protrudes lower into the pelvis, which can decide about the nephrectomy side.
Kidney size is best described by height-adjusted total kidney volume(ht-TKV). CT and MR based calculations are equivalently accurate.[5]
In clinical practice, two methods of TKV calculations are mainly used:
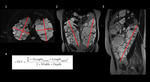
-derived from the ellipsoid equation: for each kidney, the mean length in the coronal and sagittal plane is obtained. Width and depth are measured in the same slice of the axial plane.[Fig.2][6]
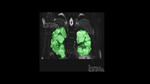
-semiautomated: each kidney boundaries are manually traced using the commercially available software. Volume of interest (VOI) is automatically calculated from the set of slices by multiplying the sum of the area by the slice thickness, with the use of the interpolation method.[Fig.3]
Polycystic liver disease
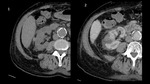
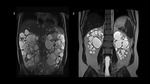
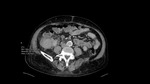
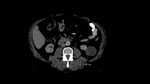
In a coexistence of massive liver and kidneys enlargement, the combined volume should be assessed to predict the need for the pretransplant NKN.[Fig.4]
It is also worth mentioning that right-sided nephrectomy can accelerate an expansion of the liver cysts and contribute to the development of Budd-Chiari syndrome.[5]
IVC compression
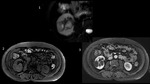
Massively enlarged right kidney, or more often, the liver may exert pressure on the inferior vena cava (IVC),[Fig.5] Long-standing compression of the IVC may lead to the development of thrombotic changes and pulmonary embolism as a consequence. After transplantation, the impaired venous outflow from the graft can contribute to Prolonged Delayed Renal Graft Function.[8]
Infectious/hemorrhagic complications
Complicated kidney cysts are common findings in ADPKD waitlist candidates. They contain blood products or high-protein fluid. These states are often difficult to differentiate based on CT or MR.
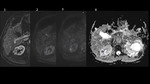
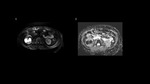
Complicated cysts are hyperdense on CT and hyperintense on T1 MR. They don’t enhance after contrast media (CM) administration and disappear on the MR subtraction. They can show restricted diffusion on DWI – that usually reflects minor intracystic bleeding or inflammation.[Fig.6] Presence of intracystic diffusion restriction is not equivalent of active infection.
Infected cysts
According to a study by Suwabe [9], at least one of four following imaging features was found in all of the infected cysts:
- wall thickening,
- fluid-fluid level,
- intracystic gas,
-high signal on DWI MR.
These radiological findings have to be accompanied by clinical evidence of infection like severe loin pain, body temperature >= 38 °C, elevated inflammatory markers.
Presence of infected cyst indicates the need for pretransplant NKN. Otherwise, the risk of generalised infection is high, especially in the immunocompromised state.
An abscess
Pyelonephritis is an inflammation of the upper structures of the urinary tract due to bacterial infection, most commonly Escherichia coli.[10]
Renal or perinephric abscess formation poses a severe complication of pyelonephritis.
Initially an abscess appears as an ill-defined, hypodense, non-enhancing area. A mature abscess shows as sharply-marginated, complex cystic mass with an enhancing rim. Fascial thickening with obliteration of perinephric fat can occur.[Fig.7] Presence of gas within a lesion is pathognomonic for an abscess.
On DWI MR abscesses show evident restriction. In ADPKD waitlist candidates DWI has an important role to play as contrast medium administration is usually contraindicated.[Fig.8,9]
Haemorrhagic cyst
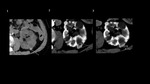
Bleeding into the cyst is often accompanied by gross haematuria and flank pain. Inflammatory markers are within normal ranges. Hemorrhagic cysts contain a high-density mass-like area or show overall high density on CT.[Fig.10]
ADPKD and renal masses
malignant
Unlike in some other congenital cystic kidney diseases, ADPKD is not associated with increased risk for renal malignancy, unless the patient is undergoing prolonged dialysis.[11,12]
RCC’s are usually solid-type lesions, but up to 15% may have a cystic component. There is also a distinct subset, described as “cystic RCC,” accounts for 5% of all.[13] An example of histopathologically confirmed multilocular cystic RCC is presented below.[Fig.11]
If RCC is presented in the kidney with numerous cysts, but the image is not strictly specific for ADPKD, the occurrence of von Hippel-Lindau syndrome should be excluded.[Fig.12]
Contrast-enhanced images are not routinely obtained in the ADPKD transplant candidates due to the risk of nephropathy or nephrogenic systemic fibrosis (NSF). However, its administration is a must when malignancy is suspected. It is essential especially for differentiating complicated cyst from cystic-type RCC.
Bosniak classification is used to stratify the risk of malignancy in cystic renal masses. The classification has been updated in 2019.[14] Update incorporates MRI in addition to CT, establishes definitions for previously vague imaging terms to enable a greater proportion of masses to enter lower risk classes.
Numerous publications confirm the usefulness of ADC derived from DWI for distinguishing benign from malignant renal cystic masses. For the malignant, significantly lower mean ADC values were reported than for benign cystic lesions.[15] Another study has shown that mean ADC values of renal abscesses are significantly lower than of cystic-type RCC's.[16]
DWI may limit the need for intravenous contrast in the discrimination between benign and malignant renal lesions, which is a great advantage in kidneys function impairment.
Benign
Angiomyolipoma (AML) may occur in the course of ADPKD, but misdiagnosed Tuberous Sclerosis should be excluded.[Fig.13,14]