Type:
Educational Exhibit
Keywords:
Not applicable, Tissue characterisation, Pathology, Surgery, Diagnostic procedure, MR, CT, Gastrointestinal tract, Abdomen, GI Tract
Authors:
M. KASSIMI, H. GUERROUM, J. HABI, N. Chikhaoui, M. Mahi; Casablanca/MA
DOI:
10.26044/ecr2020/C-10711
Findings and procedure details
-
The reported age of presentation is 40–70 years old, with an equal male-to-female ratio.
-
The most common presenting symptom includes abdominal pain or a palpable mass, followed by a GI bleed, unexplained anemia, fatigue and malaise.
-
The aim of imaging is to locate the lesion, define its morphological characteristics, evaluate local invasion and detect distant metastasis.
-
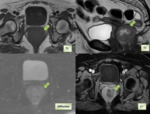
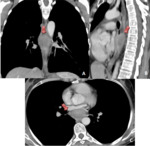
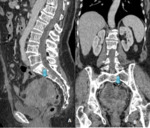
CT is the imaging modality of choice for diagnosing GIST at initial presentation, staging and monitoring the disease during and after the treatment. MRI is particularly useful in cases where CT is contraindicated, in delineating the rectal GIST and defining its relationship prior to the surgical intervention(Fig 3).MRI can better evaluate liver metastasis than CT.
-
Imaging features of GISTs predominantly depend on the size and aggressive nature of the tumor.
-
Useful characteristics frequently found in GIST with high mitotic index are:
- Lesion larger than 5 cm .
- Heterogeneous contrast enhancement .
- Location of the tumor.
- Presence of metastasis .
- Component necrotic-cystic.(Fig 9)
*Typical presentation :
-
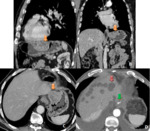
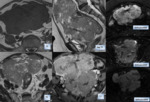
Nodule or mass depending of the wall of the gastrointestinal tract, with exophytic growing (which means towards the peritoneal cavity). (Fig 1)
-
Well-circumscribed borders, with a cleavage plane between the tumour and the abdominal organs next to it .(Fig 11)
-
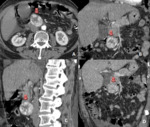
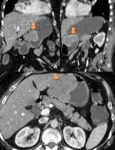
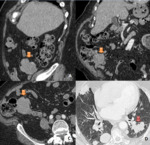
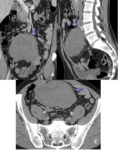
Small tumors tend to show an homogeneous enhancement, Larger lesions (more than 2-3 cm) are seen as heterogeneous masses enhancing peripherally due to central necrosis and haemorragic degenerations which are commonly present in massive lesions (Fig 2).
-
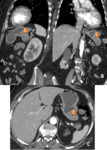
The liver is the most common metastatic site of malignant GISTs, followed by peritoneum. Liver metastasis appears as focal nodular lesions, and they may be homogeneous or heterogeneous depending on their size and the presence of necrotic and/or bleeding areas (as it happens in the primary tumour).(Fig 1). Peritoneal implants are always well defined wich is important to differentiate GISTs and other neoplasms, such as the ovarian carcinoma.
-
GISTS almost never show lymphatic dissemination. This lack of lymph node affectation must be taken into account when considering the diagnosis of GIST
*Atypical presentation
1-Atypical locations
-
Extra-gastrointestinal GISTs :CT findings of GISTs arising in these locations are not characteristic, and they are indistinguishable from other sarcomas including liposarcoma,fibrosarcoma and leiomyosarcoma.
2-Endophytic growth: Gist Typically grow outward, away from the originating bowel lumen, but they may also show endoluminal and intramural growth.(Fig 6)
3-Cavitation : The central necrosis usually seen in these tumours sometimes extends and creates a necrotic cavity and a fistula to the intestinal lumen, allowing food, gas and oral contrast to get inside.
4-Peritoneal haematoma :Seen when the intratumoral bleeding that is so frequent in GISTs extravasates into the peritoneal cavity, appearing in the CT as an heterogeneous collection that impairs the visualitation of the underlying neoplasm.
5-Intestinal intussusception : A condition that a portion of gastrointestinal tract into the lumen of the immediate adjacent intestine, leading to intestinal obstruction in most cases. It is a very rare complication of GISTs.
6-Visceral infiltration :In some atypical cases especially agressive tumours invade the parenchyma of the adjacent organs .
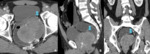
7-Calcifications : are extremely rare finding at the moment of diagnosis and radiologists should think any other diagnosis in the differential diagnosis list, if present .However, after specific chemotherapy calcification is occasionally seen . (Fig 7)
8-Multifocal lesion : Most GISTs occur sporadically and multiplicity is very rare.
9-Lymphatic dissemination /lung /bone metastases: very Uncommon in this kind of neoplasms . (Fig 8)
- Gold standard treatment is surgical resection. Tyrosine kinase inhibitors such as imatinib mesylate are added to adjuvant treatment as targeted therapy to high risk patients .