Carotid cavernous fistulas (CCF) are a subtype of dural arteriovenous fistulas that consist of an abnormal communication between the cavernous sinus and the carotid artery. This communication may be classified either as direct if the defect is on the wall of the internal carotid artery (ICA) or as indirect if the defect is on meningeal branches of the ICA or external carotid artery.
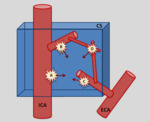
There are other classifications based on the pathogenesis (traumatic or spontaneous), on the flow dynamics of the fistula (high or low flow) and, most importantly, on the angiographic anatomy: the Barrow et al. classification (Fig. 1) [1].
RELEVANT ANATOMY
The cavernous sinus is a paired venous plexus located lateral to the sphenoid bone and the sella turcica that receives blood supply from [2]:
- The superior and inferior ophthalmic veins,
- The central vein of the retina,
- The sphenoparietal sinus,
- The superficial middle cerebral vein,
- Inferior cerebral veins.
The drainage is achieved by means of the superior and inferior petrosal sinuses, which drain to the transverse sinus and then to the internal jugular vein; as well as the pterygoid plexus and the facial vein.
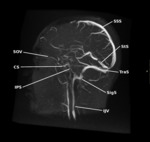
Lastly, both cavernous sinuses are interconnected thanks to the two intercavernous sinuses, which lie anterior and posterior to the infundibulum and lack any valves, ensuring a low pressure and reversible blood flow [3] (Fig. 2, Fig. 3, Fig. 4, Fig. 5).
In regard to the relationship with nervous structures, the lateral wall of the cavernous sinus allocates:
- The oculomotor nerve (CN III),
- The trochlear nerve (CN IV),
- The ophthalmic division of the trigeminus (CN V1),
- The maxillary division of the trigeminus (CN V2),
And it is traversed by the abducens nerve (CN VI), which courses lateral to the ICA [2] (Fig. 6).
The ICA enters the cavernous sinus through the base and exits through the superior wall, being accompanied by sympathetic fibres and giving origin to several arterial branches. It is in this location where the ICA acquires an âSâ shape, thus the name of siphon or sigmoid segment [3,4].
PATHOPHYSIOLOGY
Several causes may produce a dCCF [1,3]:
- Trauma (the most common),
- Aneurysm rupture,
- Collagen vascular anomalies (Ehlers-Danlos type IV, fibromuscular dysplasia, osteogenesis imperfectaâŚ),
- Iatrogenic.
The defect in the wall of the ICA is usually a single hole, but in some cases, there may be more than one or a complete transection of the wall [1]. Due to this defect, a shunting between a low flow venous system and a high flow arterial system occurs, resulting in failure of the drainage of the tributary veins of the cavernous sinus or venous congestion. Depending on the most impaired venous drainage pathway and existence or lack of collaterals, different signs and symptoms may appear [3,5,6]:
- Orbital bruit, chemosis and exophthalmos (also known as the classical triad) due to increased pressure in the superior and inferior ophthalmic veins (anterior drainage).
- Ophthalmoplegia, facial sensory deficits, ptosis and photophobia because of the compression of the cranial nerves in the lateral wall of the cavernous sinus [7].
- Intracranial haemorrhage, venous infarct and headache if the venous pressure rises within the sphenoparietal sinus and in turn into the cerebral cortical veins (rare) [4].
- Posterior draining fistulas to the superior and inferior petrosal sinuses are often asymptomatic, but cranial neuropathy may still be present and infrequently brainstem congestion [8,9].
- Bilateral or contralateral symptoms in case the venous pressure is conveyed to the opposite cavernous sinus via the intercavernous sinuses [3,7,10].
- Ipsilateral cerebral ischemia in patients with poor collateral circulation when the flow of the ICA is diverted completely into the cavernous sinus (steal phenomenon) [1,9].

![Fig. 2: Dural venous sinuses. References: Carter HV, Gray H. Anatomy of the Human Body [Internet]. 1858 [cited 2020 Jan 13]. Available from: https://commons.wikimedia.org/wiki/File:Gray568.png](https://epos.myesr.org/posterimage/esr/ecr2020/155441/media/855349?maxheight=150&maxwidth=150)
![Fig. 3: Figure 3. Tributaries and drainage of the cavernous sinus. References: Timol N, Amod K, Harrichandparsad R, Duncan R, Reddy T. Imaging findings and outcomes in patients with carotid cavernous fistula at Inkosi Albert Luthuli Central Hospital in Durban. South African Journal of Radiology [Internet]. 2018 Jan 25 [cited 2020 Jan 6];22(1). Available from: https://sajr.org.za/index.php/sajr/article/view/1264](https://epos.myesr.org/posterimage/esr/ecr2020/155441/media/855350?maxheight=150&maxwidth=150)
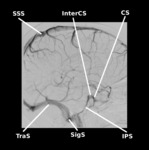
![Fig. 6: Anatomy of the cavernous sinuses. References: Kuybu O, Dossani RH. [Figure, Anatomy of the cavernous sinus. Contributed by Okkes Kuybu, MD and Diana] [Internet]. 2019 [cited 2020 Jan 13]. Available from: https://www.ncbi.nlm.nih.gov/books/NBK532976/figure/article-19034.image.f1/](https://epos.myesr.org/posterimage/esr/ecr2020/155441/media/855353?maxheight=150&maxwidth=150)
