Imaging plays a significant role in the diagnosis of PABC. It is a challenging diagnosis since physiological changes seen in pregnancy may limit clinical suspicion imaging techniques utility.
Ultrasound
Ultrasound is the initial image modality with a reported sensitivity of up to 100% and a negative predictive value of up to 100%. 6 Since there is an increase in the nodularity of the gland associated with pregnancy, any mass that persists for more than 2-4 weeks should raise suspicion for malignancy and must be assessed initially by this imaging method. PABC is observed as hypoechoic masses with cystic components due to associated central necrosis. The borders are irregular and may have a posterior acoustic shadow or echogenic halos. 7 When circumscribed margins, oval shape, and parallel orientation are seen in a suspicious lesion, benign pathology may be suggested, and no further evaluation is necessary.8 (see figure 1)

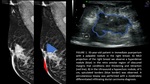
Fig. 1: 35-year-old patient immediate puerperium with a palpable nodule in the right breast. A) MLO projection of the right breast, we observe a hyperdense nodule (blue) in the retro-areolar region of obscured margins that conditions skin thickening and retraction (red line). B) in the usg a hypoechoic nodule of 5 cm, spiculated borders (blue line) was observed. A percutaneous biopsy was performed with a moderately differentiated infiltrating ductal carcinoma.
Mastography
Bilateral mastography is recommended in patients with a clinical suspicion. The sensitivity of mastography PABC is 78-90% (even in dense breasts). Radiation to the fetus is minimal, with an estimated dose of less than 0,03 uGy; therefore, two basic projections are encouraged in patients.8 Suspicion findings include nodules, masses, microcalcifications, asymmetries, distortions in the architecture or thickening of the skin.
Mastogrphy is extremely useful in the evaluation of microcalcification, which is not seen in ultrasound evaluation and in the determination of disease extent (multifocal multicentric and contralateral disease).7 Routine screening mastography must be continued in patients over 40 years 3 months after lactation cessation.7 (see figure 2).

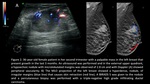
Fig. 2: 36-year-old female patient in her second trimester with a palpable mass in the left breast that presents growth in the last 3 months. An usg was performed and in the upper external quadrant, a hypoechoic nodule with micro-nodulated margins of 2.8 cm was observed. Doppler usg A) shows peripheral vascularity. B) the MLO projection of the left breast shows a hyperdense, nodule, of irregular margins (blue line) that causes skin retraction (red line). A BI_RADS 5 was given and a percutaneous biopsy was performed, with a triple-negative high grade infiltrating ductal carcinoma.
MRI
The use of magnetic resonance imaging in patients with PABC is not used routinely recommended. It is reserved for patients, in whom the cost-benefit is clear. 8 The contrasted agents are classified as type C drugs according to the FDA. Gadolinium crosses the fetus-placental barrier and can be eliminated by the fetal kidneys. In breastfeeding patients, magnetic resonance imaging is safe since gadolinium has a very small excretion through milk (rate of 0.0004%).9 According to the American College of Radiology Guidelines, breastfeeding suspension is not required. 10 Findings include masses with homogeneous, heterogeneous or ring enhancement or non-mass lesions with segmental enhancement. The gland that is in lactation has a rapid physiological enhancement after the administration of contrast medium with an early plateau, associated with the increase in physiological vascularity. These findings should not be confused with malignancy (See figure 3).

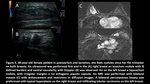
Fig. 3: 38-year-old female patient in puerperium and lactation, she felt nodules since her first trimester on both breasts. An usg was performed. A) In the right breast an isoechoic nodule with ill-defined borders with central vascularity. B) On the left breast, a hypoechoic nodule with irregular margins and no echogenic pseudo-capsule was observed. C) Bilateral MRI was performed with bilateral masses that showed enhancement and restriction in the diffusion sequence. A bilateral percutaneous biopsy was performed with typical hyperplasia on the right breast and infiltrating lobular carcinoma on the left breast.
The prognosis is worse when PABC is associated with lymph node metastasis, larger tumor size and delayed detection.