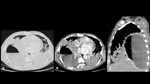
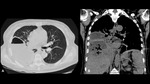
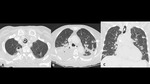
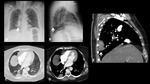
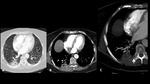
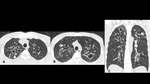
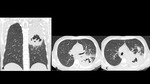
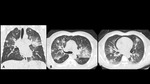
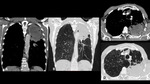
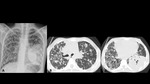
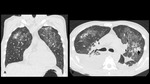
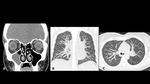
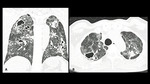
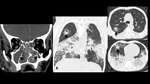
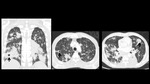
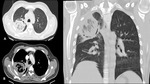
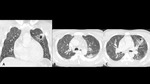
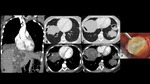
A series of cases of cavitary lung infections will be presented following the next categories:
- Common bacterial infections (Fig 2-6)
- Uncommon Bacterial Infections (Fig 7-10)
- Non-tuberculous mycobacteria
- Fungal infections (Fig 11-19)
- Parasitic infections (Fig 20-21)
1.Common bacterial infections:
Infections caused by bacteria can generate pulmonary cavitations by two mechanisms.
- The first occurs when entering the airway and evading defense cells, causing necrotizing pneumonia (Fig 2) or lung abscesses (Fig 4-5).
- The second mechanism occurs when entering the lung through the bloodstream and cause septic emboli (Fig 6).
The most isolated organisms in lung abscesses in both adults and children are anaerobic and microaerophilic components of the oral flora, and lung abscesses are frequently polymicrobial.
Pulmonary gangrene is a rare condition due to an entire segment of a lung destroyed, commonly by K. pneumoniae.
2. Uncommon Bacterial Infections
Actinomycosis (Fig 7-8), Nocardia, Melioidosis (Fig 9) and Rhodococcus (Fig 10) infections are included in this group. These infections are relevant in patients with a history of transplantation or who are receiving immunosuppressive drugs and in patients with HIV-AIDS, lymphoma or leukemia infection.
3. Non-tuberculous mycobacteria (NTM)
Nontuberculous mycobacteria are present in soil, water, and dust, so pulmonary infection occurs probably via inhalation of infectious aerosols. Mycobacterium avium complex is the most common organism associated with pulmonary disease. A small group of NTM infections are caused by mycobacteria classified as rapid growers, principally the Mycobacterium abscessus complex.
The risk factors for pulmonary infection are immunocompromised with HIV or prior organ transplantation, COPD, silicosis, prior TB infection and cystic fibrosis. Elderly women are also at risk. Imaging findings include signs of chronic airway inflammation (bronchiectasis and small airway disease presenting as branching centrilobular or tree-in-bud opacities mainly in lingula and middle lobe), and fibrocavitary changes and nodules mostly in the upper lobes.
4. Fungal infections
The three endemic fungal infections in Latin America are histoplasmosis (Fig 15-17), paracoccidioidomycosis, and coccidiodomycosis. Nevertheless; aspergillosis (Fig 11-13), mucormycosis (Fig 19), blastomycosis, cryptococcosis (Fig 14), Penicillium infection, and Pneumocystis jiroveci pneumonia can also produce cavitations.
The halo sign and the reverse halo are not pathognomonic for Aspergillosis. It has been found in other non-infectious diseases and in infections such as Mucormycosis. The sign of the crescent air, although it can help in the diagnosis, is usually of late presentation.
Cavitary lung lesions are uncommon in disseminated histoplasmosis, which occurs in immunocompromised patients (Fig 15).
5. Parasitic infections
Parasitic lung infections usually are subacute or chronic diseases. Differential diagnoses are pulmonary hydatidosis (Fig 20) produced by Echinococcus granulosus and Echinococcus Multilocularis, and the paragonomiasis (Fig 21) generally produced by Paragonimus westermani; both infections can occur in previously healthy patients, with no history of importance.
Ingestion of undercooked, raw, or pickled crustaceans is a risk factor for pulmonary aragonimiasis.