Cirrhosis is an advanced chronic liver disease with a wide clinical and pathophysiologic spectrum resulting from repetitive liver injury.
Hepatocellular carcinoma (HCC) is the most frequent malignant tumoral entity which may form in a cirrhotic liver, and it’s often diagnosed based on it’s imagistic appearance (CT and MRI semiology).
Hepatocarcinogenesis. At a molecular level hepatocarcinogenesis is always involving multiple alterations until the normal hepatocyte is transformed into a malignant cell Fig. 1 , meanwhile at a histological level, hepatocarcinogenesis may be multistep as before mentioned or de novo hepatocarcinogenesis which refers to the emergence of HCC without histologically definable precursor lesions (1). In this case, overtly malignant HCC arise without passing through intermediate histological steps.
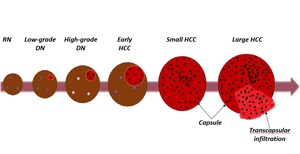
Fig. 1: Multistep hepatocarcinogenesis and its accompanying pathophysiological alterations;
References: Adapted from American College of Radiology: LI-RADS v2018 manual (1)
Mimics of HCC. Of the benign lesions discussed in this paper we mention, arterio-portal shunts which is a potentially reversible cause of portal hypertension represented by abnormal communication between the portal venous system and the arterial system (7). It represents a category of lesions commonly encountered in liver cirrhosis, most often being concomitant with HCC-type tumor lesions, requiring a careful analysis of imaging behavior for a correct diagnosis.
At the opposite end, hemangioma, a benign tumoral lesion is rarely encountered in cirrhotic patients, in most cases with subcapsular distribution. If the lesion existed before, the cirrhotic architectural changes, secondary to fibrosis, it is reduced until disappears (3).
Focal nodular hyperplasia-benign tumor rarely encountered in a cirrhotic liver, and whose diagnosis of certainty is by exclusion of HCC.
Cholangiocarcinoma and biphenotypic tumors are primary malignancies, the former is more frequent, and the latter rarely encountered, sometimes having common imaging features with HCC.
Hypervascular metastases are rare encountered in the cirrhotic liver, easy to confuse with HCC.



