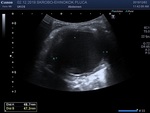
Ultrasound is the primary imaging modality for the diagnosis and evaluation of hydatid disease (fig 3.). It enables localization and evaluation of the cyst content. CT and MRI are essential for establishing a relationship with surrounding structures. They are a modality of the first choice for organs that are inaccessible for ultrasound evaluation. CT is better for detection of calcification of the cyst, which is crucial for determination of the viability of the cyst. This is very important for making an appropriate decision about the treatment. The imaging finding depends mainly on the organ involved, reaction of the host immune system, stage of evolution and maturity of the disease.
Hydatid cyst may appear as a solitary cyst or mutiple cysts, with or without separation, with or without calcification. The presence of a daughter cyst and membranes with internal calcification are important for the differential diagnosis.
Hydatid cyst is classified into four types based on their appearance.
Type 1:
In the initial stage of the disease, the hydatid cyst appears as unilocular cyst without septations. After application of the contrast medium on CT imaging, there is usually a post-contrast enhancement of the cyst wall. On T2-weighted imaging, the pericyst usually appears as the hypointense rim (fig 9).
Type 2:
The multivesicular cyst represents a cyst with multiple sepatations of the daughter cyst, which are usually arranged at the periphery. This type of cyst may be subdivided according to the maturity and arrangement of the daughter cyst within the cyst.
In 2a type, daughter cysts are arranged at the periphery and matrix that is high-density (the wheel spoke appearance). In 2b type, daughter cysts are irregularly arranged, occupying the whole maternal cyst. Type 2c is represented by high density cyst with calcifications and a daughter cyst.
Type 3:
This type represents the hydatid cyst with calcification.
Type 4:
This type represents complications of the hydatid cyst. The most common complication includes rupture or super infection. Age of the cyst, chemical reaction, host defense mechanism or trauma are major causes of the rupture. Imaging finding in the contained rupture is highly specific, and appears as a curvilinear structure or a floating membrane. It represents detachment of the endocyst from the pericyst. Sometimes, a rupture can have a communication with the bile ducts or bronchial tree. Rupture of the endocyst and pericyst will results in direct leakage of the cyst content into the peritoneal or pleural cavity.
Specific sites of involvement:
Lungs
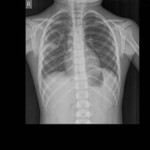
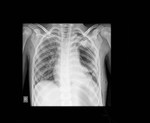
The lung is the most common location of hydatid cyst in children (20 – 25 % of cases). In unilateral form of the disease, there is predilection for the right posterior segments (Fig 1.). This is usually explained by the transdiaphragmatic extension of the disease from the underlying hydatid disease of the liver (Fig.5). Cough, purulent sputum, fever and chest pain are the most common symptoms of plumonary hydatid disese.
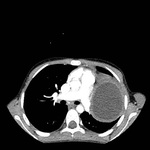
Rapid growth of the cyst is allowed due to the lung tissue and immune system in childhood. In the initial phase of the disease, hydatid cyst manifests as type I cyst (fig 2.) with well-defined borders. On CT imaging, these cysts have density (HU values) similar to fluid (fig 4). Type 2 and 3 cysts are uncommon in the lungs.
Complication of hydatid disease ih the lungs include rupture in the lung parenchyma and pleural cavity.
Liver
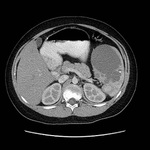
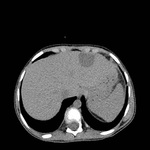
The liver is the second most common location for hydatid disease in children. The right lobe of the liver is more commonly involved. Type 1 cyst is difficult to differentiate from a simple epithelial cyst just by imaging (fig 5.). On ultrasound examination, ehogenic foci that fall into dependent portion of the cyst represent a characteristic finding for hydatid disease. Sometimes, multiple hydatid cysts within the liver may be in different stages.
The cyst may appear as a well-defined cystic lesion with floating membranes within (fig 6.). Type 2 cyst, with multiple septa formed by walls of daughters cysts, gives a characteristic “honeycomb appearance”. Type 3 is presented by ring-like or curvilinear calcifications which involve the pericyst. Death of the cyst is usually presented by a dense calcification.
Type 4 cyst is most commonly presented by perforation in the billiary tree (fig 6.) that may occur through small fissures or a fistula.
Spleen
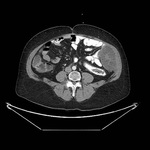
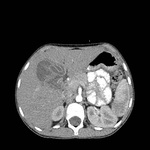
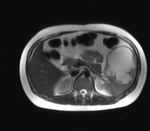
Hydatid disease of the spleen (fig 9.) is uncommon. Hydatid disease of the spleen is usually a result of the intaperitoneal disseminated disease due to rupture of hydatid cyst on the liver. The patients are usually asymptomatic, but sometimes may present with unspecific pain (fig 10.) it the left upper quadrant or splenomegaly.
The imaging findings are similar to those of hydatid disease in other abdominal viscera.
Spine
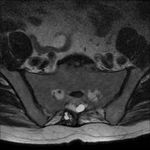
Hydatid disease of the spine (fig 11.) is very uncommon; it occurs in less than 1% of cases. According to its location, it can be divided into following groups: intramedullary, intradural extramedullary, extradural intraspinal, vertebral and paravertebral.
On MR imaging, cysts with signal intensity similar to CSF can be seen. Type 3 cysts are uncommon in the spine.
Peritoneum
Primary peritoneal involement(fig 12.) is uncommon, and is usually a consequence of secondary peritoneal seeding due to rupture of hydatid cyst on the liver or spleen. Most of the patients have a history of previous surgery of hepatic hydatid disease.
Imiging findings are similar to those of hydatid disease located in other abominal viscera. Type 1 cyst in the peritoneum is difficult to differentiate from mesenteric or intestional duplication cyst just by imaging features.
Sypmtoms are unspecific, and usually a consequence of the mass effect of cyst on the surrounding abdominal viscera.