We retrospectively analyzed all the cases of parasitic diseases that we had diagnosed in our radiology department. After careful analysis of the relevant radiological imaging data we selected prototypical images of the parasitic diseases which represent some of the characteristic appearances as reviewed in the current literature. The typical co-existing spectrum of findings which in the background of relevant clinical history should raise high index of suspicion were also noted.
3.1 PARASITIC DISEASES OF THE ABDOMEN
Some of the common parasitic diseases of the abdomen with their characteristic findings on imaging are as listed below.
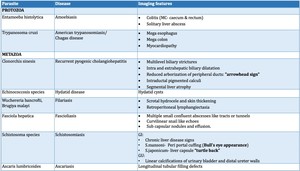
Fig. 2: Parasitic diseases of abdomen with salient imaging features
PRE CANCEROUS PARASITES
| Chaga's disease |
Oesophageal carcinoma |
| S.japonicum |
Gastric and liver carcinoma |
| Clonorchiasis |
Cholangiocarcinoma |
| Opisthorchiasis |
Cholangiocarcinoma |
| S.hematobium |
Bladder cancer |
1. AMOEBIASIS
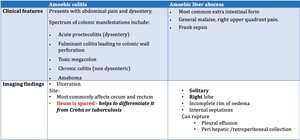
Fig. 3: Clinical and imaging features of Amoebiasis
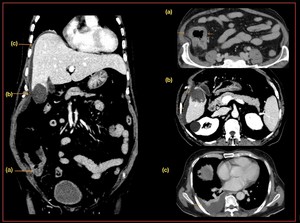
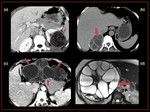
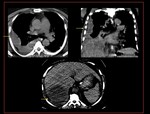
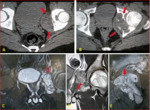
Fig. 4: Amoebic colitis with ruptured amoebic liver abscess.
Coronal and axial CT scan demonstrates,
a-Circumferential oedematous wall thickening with mucosal irregularity (ulceration) and adjacent fat stranding in the caecum
b-Ruptured liver abscess with peri hepatic collection
c-Extension of abscess into pleural space with mild right pleural effusion and sub segmental collapse of basal segments.
2. HYDATIDOSIS
Layers of hydatid cyst
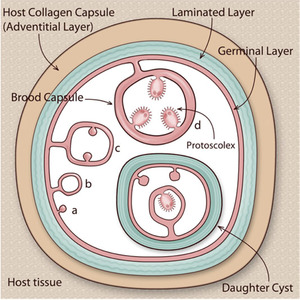
Fig. 5: Layers of hydatid cyst
References: Díaz A. Immunology of cystic echinococcosis (hydatid disease). [Internet]. Semanticscholar.org. 2020 [cited 14 January 2020]. Available from: https://www.semanticscholar.org/paper/Immunology-of-cystic-echinococcosis-(hydatid-D%C3%ADaz/2f1b2d733f4461d6301efda59d922675c9c62abb/figure/0
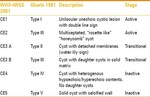
Classification of hydatid cysts
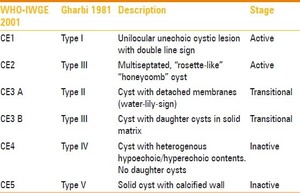
Fig. 6: Classification of hydatid cysts
References: http://www.ijri.org/article.asp?issn=0971-3026;year=2012;volume=22;issue=1;spage=23;epage=26;aulast=Corona
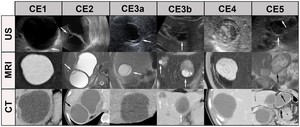
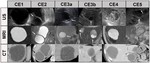
Fig. 7: Classification of hydatid cysts
References: https://journals.plos.org/plosntds/article/figure?id=10.1371/journal.pntd.0001880.g005
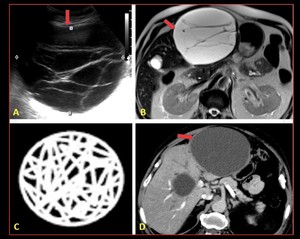
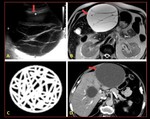
Fig. 8: Hydatidosis : (A) USG image, (B) axial T2 MRI (C) representative pic (D) Axial CT demonstrating cyst with a predominantly thick membranes.
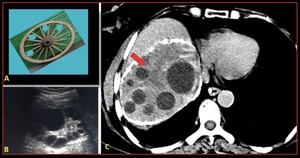
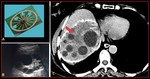
Fig. 9: Hepatic hydatid with cart wheel like appearance. Axial CT scan of liver and USG demonstrates hepatic hydatid cyst with multiple daughter cyst giving cart wheel like appearance with partial cyst wall calcification
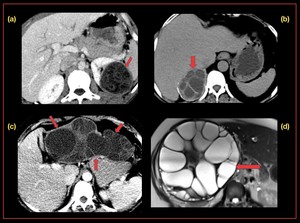
Fig. 10: Hydatidosis: Axial CT scan demonstrates, hydatid cyst in the (a) left kidney, (b) right adrenal gland, (c) intraperitoneal hydatid cyst, axial T2w MRI demonstrates (d) hepatic hydatid cyst
3. RECURRENT PYOGENIC CHOLANGIOHEPATITIS
Clinical features :
- Recurrent right upper quadrant pain
- Fever
- Jaundice.
Imaging features:
Dilatation of first and second order ducts.
Disproportionate extra hepatic duct dilatation. |
| Abrupt tapering of peripheral ducts with decreased arborisation of biliary tree- arrow head sign |
|
Multiple intra hepatic strictures
|
|
Intra ductal calculi
|
|
Parenchymal atrophyà left lateral segment > right posterior segment
|
|
Enhancement of bile duct walls- acute cholangitis
|
|
Complications:
•Hepatic abscess
•Biloma
•Portal vein thrombosis
•Malignancy
|
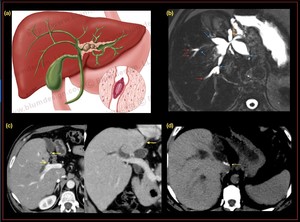
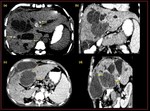
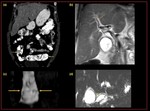
Fig. 11: Recurrent pyogenic cholangiohepatitis : (a)Representative image demonstrating infestation of Clonorchis sinesis causing biliary duct strictures with calculi (b) Axial T2w MRI demonstrating, strictural narrowing of the extra hepatic biliary tree at porta hepatis (orange arrow), multifocal short segment intrahepatic biliary strictures with proximal intrahepatic biliary dilatation (blue arrow), arrow head sign (red arrow),(c) axial CT demonstrates, complete atrophy of segments II, III, IV b and near complete atrophy of segment IV a of left lobe of the liver with thinning and attenuation of the left portal vein, (d)dilated biliary duct/ biliary diverticulum with dependent calculi seen along the anterior border of the caudate lobe
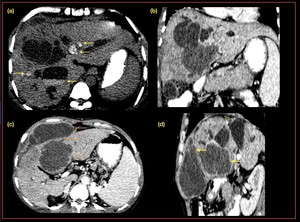
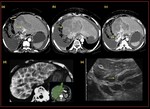
Fig. 12: A case of Recurrent pyogenic cholangiohepatitis with cholangitis and ruptured cholangitic abscess. (a),(b) Axial CT demonstrates, asymmetrical saccular and fusiform dilatation of the intrahepatic biliary radicles, predominantly in the right lobe of liver with calcific densities within, (c), (d) Cholangitis abscess with rupture and adjacent encapsulated peri hepatic collection.
4. FILARIASIS
Clinical presentations include:
- Microfilaremia
- Acute lymphangitis
- Lymphadenitis
- Limb oedema
- Genital swelling
- Tropical pulmonary eosinophilia.
Imaging features:
Fig. 13: Filariasis: Scrotal USG demonstrating filarial dance sign
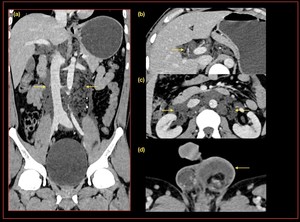
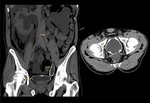
Fig. 14: A case of filariasis. Coronal and axial CT demonstrating, (a) retro peritoneal lymphangiectasia, which is insinuating into the porta hepatis (a), renal hilum (c) without any mass effect/ infiltration,(d) scrotal hydrocele and skin thickening.
5. FASCIOLIASIS
Clinical features
- Right upper quadrant pain
- Fever
- Weight loss
- Fatigue, pruritis
- Vomiting

Fig. 15: Imaging features of Fascioliasis
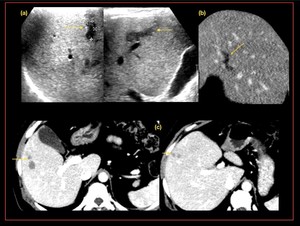
Fig. 16: Case of hepatic fascioliasis, (a) USG demonstrates, irregular tubular serpiginous hypo echoiec structures in segment V n VIII of right lobe of liver (b) Sagittal CT demonstrates,confluent abscess detected as tract, (c) Axial CT demonstrates, sub capsular and parenchymal hypodense,non enhancing nodules
6. SCHISTOSTOMIASIS
Clinical features:
- Portal hypertension signs and symptoms, including splenomegaly, gastroesophageal varices, hematemesis, and ascites.
Imaging features:
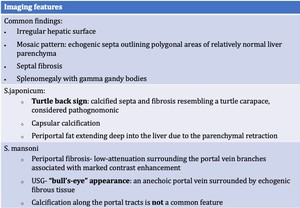
Fig. 17: Imaging features of Schistostomiasis
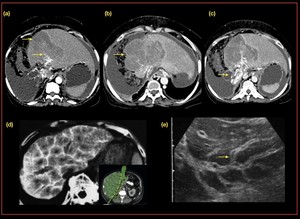
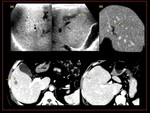
Fig. 18:
Schistostomiasis- Axial CT demonstrates, (a)(b)(c)
-Significant atrophy of the right lobe of the liver with hypertrophy of the lateral segment of the left lobe of the liver
-Hypodense poorly enhancing area involving the residual right lobe, caudate lobe and medial segment of left lobe extending into the lateral segment of left lobe and the hepatic hilum.
-Multiple parenchymal calcifications, linear vascular areas of calcification, calcification around porta tracts.
-(d) Turtle back sign
-(e)Peri portal fibrosis (bull’s eye appearance)
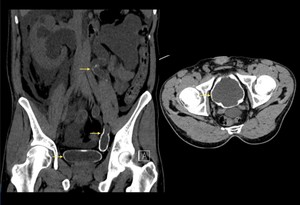
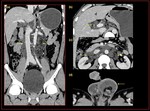
Fig. 19: Genito urinary Schistostomiasis, Coronal and axial CT demonstrates, (a) Extensive calcification of the urinary bladder and proximal ureter wall, with marked tortuous hydroureters and hydronephyrosis more at the left.
References: https://radiopaedia.org/cases/schistosomiasis
7. ASCARIASIS
Clinical features:
Gastrointestinal manifestations are due to adult worms, it includes:
- Most common complication of ascariasis is mechanical small bowel obstruction caused by a large number of worms.
- Volvulus or intussusception.
- Acute appendicitis
- Pancreatitis
- Acute cholecystitis
- Liver abscess
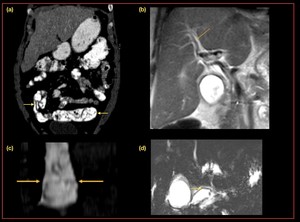
Fig. 20: Ascariais- adult worms can be seen as longitudinal tubular filling defects.
(a) and (c) Coronal CT images with oral contrats demonstrating, gastro intestinal ascariasis, (b) and (c) MRCP images demonstrating,biliary ascariasis.
3.2 PARASITIC DISEASES OF THE CENTRAL NERVOUS SYSTEM
- Imaging plays a significant role not only in diagnosis but also in the follow up for treatment response.
- Some of the common parasitic diseases of the central nervous system, with their characteristic findings on imaging are as listed below:
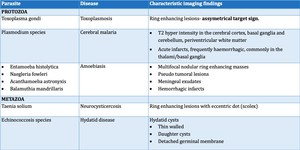
Fig. 21: Parasitic diseases of central nervous system with salient imaging features
1. TOXOPLASMOSIS
Toxoplasmosis can be categorized into 4 groups:
- Acquired in the immunocompetent patient
- Acquired or reactivated in the immunodeficient patient
- Ocular
- Congenital.
Clinical features:
|
CONGENITAL
|
ACQUIRED
|
- Chorioretinitis
- Intracranial calcifications
- Hydrocephalus
|
- MCC of cerebral abscess in HIV patients
- Symptoms are vague and indolent.
- Development of new neurological symptoms in these patients should raise high suspicion of cerebral toxoplasmosis.
- Encephalitis
|
Imaging features:

Fig. 22: Imaging features of congenital toxoplasmosis
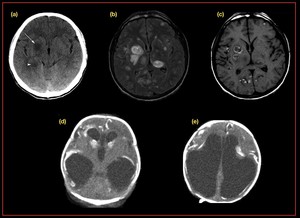
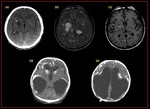
Fig. 23: Congenital toxoplasmosis:
(a, b,c) Axial CT,FLAIR and post contrast images demonstrate show hypodense, hyperintense, ring enhancing lesions in the basal ganglia and left thalamus. Numerous hyperintense lesions also are seen around the gray matter–white matter junctions, findings indicative of a hematogenously disseminated process.
(d,e) CT shows markedly dilated lateral and third ventricles with ventricular wall calcification,severe cortical thinning with multiple parenchymal and deep nuclear calcifications along with the ventricular wall calcifications
References: https://pubs.rsna.org/doi/full/10.1148/rg.294085205, https://radiologykey.com/infection-and-inflammatory-diseases-of-the-central-nervous-system/
ACQUIRED TOXOPLASMOSIS
Imaging features:

Fig. 24: Imaging features of acquired toxoplasmosis
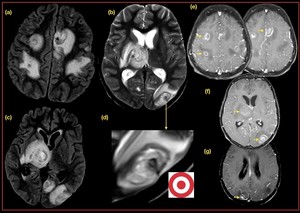
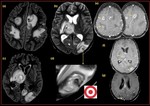
Fig. 25: Acquired toxoplasmosis: (a,b,c,d,e,f,g)
There are multiple T1 and T2/FLAIR heterogenous lesions with significant peri lesional edema, of varying sizes seen in bilateral cerebral hemispheres, right thalamocapular region, right cerebral peduncle, superior vermis and right inferior cerebellum.
(d)Target sign with multiple concentric T2 hypo intense rings.
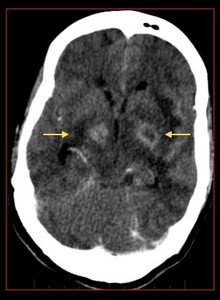
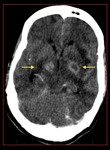
Fig. 26: Cerebral toxoplasmosis with ring enhancing lesions in bilateral basal ganglia
2. CEREBRAL MALARIA
Neurological symptoms on a background of malarial infection.
Clinical features:
- Headache,
- Altered state of consciousness
- Seizures
- Backache
- Vomiting, nausea
Imaging features:

Fig. 27: Imaging features of cerebral malaria
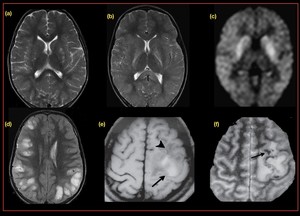
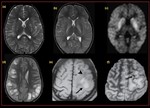
Fig. 28: Cerebral malaria- Axial T2 FSE image (a,b,c) demonstrate, T2 hyper intense lesion in bilateral basal ganglia which demonstrates diffusion restriction.
(d) Patchy areas of cortical T2 hyper intensity.
Another case of cerebral malaria (e, f), Axial T1W image demonstrates a T1w image demonstrates, hyper intense signal (arrow) in the high left frontoparietal region with surrounding hypo intensity (arrowhead). The gradient image shows blooming (arrow) within the T1 hyperintense area
References: https://www.semanticscholar.org/paper/Acute-brain-MRI-findings-in-120-Malawian-children-Potchen-Kampondeni/23d5b203af973473c8bc7e1bc292d5a3c7d06885/figure/1, https://www.ncbi.nlm.nih.gov/pmc/articles/PMC2747424/
3. NEUROCYSTICERCOSIS
STAGES OF NCC
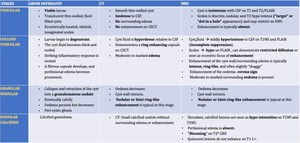
Fig. 29: Stages of Neurocysticercosis
WHAT TO LOOK FOR IN EACH SEQUENCE?
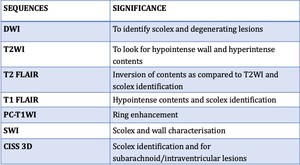
Fig. 30
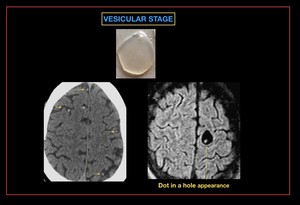
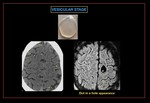
Fig. 31: Neurocysticercosis- VESICULAR stage
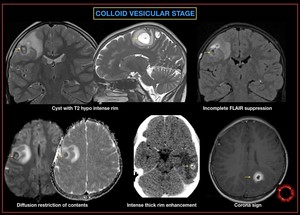
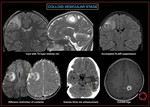
Fig. 32: Neurocysticercosis- Colloid vesicular stage
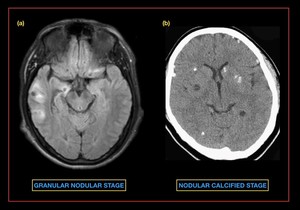
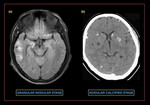
Fig. 33: (a)Nodular-granular stage neurocysticercosis - Axial flair image demonstrates, shrinking cysts with minimum mass effect and surrounding gliosis. (b) Calcified granulomas.
References: https://www.sciencedirect.com/science/article/pii/S2352621115000030
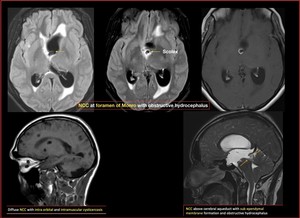
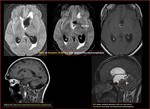
Fig. 34: Neurocysticercosis
MRI IMAGING CRITERIA FOR NCC
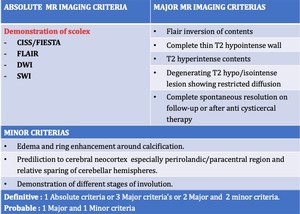
Fig. 35: Diagnostic criteria for neurocysticercosis
4. CEREBRAL AND SPINAL HYDATID CYSTS
Clinical features:
Symptoms and signs include:
- Focal neurological deficits
- Headaches
- Increased intracranial pressure
- Hydrocephalus
- Papilledema and loss of vision
- Altered mental status
- Seizures (rare)
TYPES
Intracranial hydatid cysts can be classified into:
| Primary hydatid cysts |
Secondary hydatid cysts |
- Occur as direct invasion of larva that managed and filtered via liver and lung to the brain
- Usually solitary but may be multiple
- Is fertile
|
- Occur as a result of rupture of primary cysts in others organs then reaching by embolization to the brain
- Usually multiple
- Infertile
- Do not have brood capsule or scolices
|
Imaging features:
- Site-Mostly located in supratentorial structures in the vascular territory of middle cerebral artery
- Well-defined circumscribed spherical non-enhancing intra-axial cystic lesion
- Cyst fluid is isointense with CSF in all pulse sequences
- No calcification or and typically no surrounding oedema
- Presence of perilesional oedema usually indicates complication as rupture or secondary infection
|
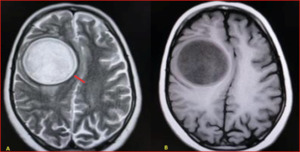
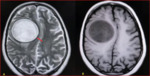
Fig. 36: Cerebral hydatid cysts
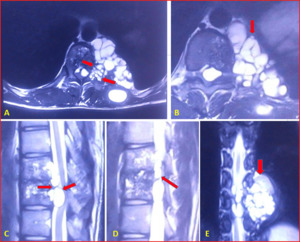
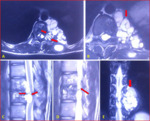
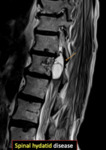
Fig. 37: Spinal hydatid cysts
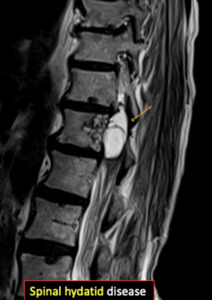
Fig. 38: Spinal hydatid cysts
3.3 PARASITIC DISEASES OF THORAX
Some of the important parasitosis of the thorax with their salient imaging features are listed below:
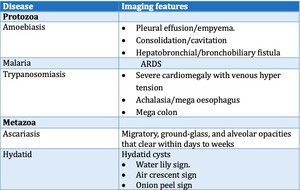
Fig. 39: Parasitic diseases of thorax with salient imaging features
1. AMOEBIASIS
After liver abscesses, pleuropulmonary involvement is the most common manifestation of extra intestinal amebiasis
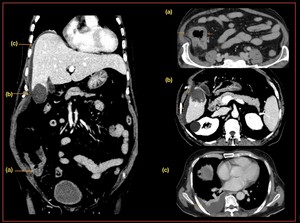
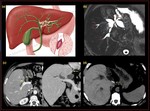
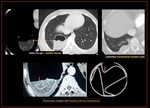
Fig. 40: Amoebic colitis with ruptured amoebic liver abscess. Coronal and axial CT scan demonstrates, a-Circumferential oedematous wall thickening with mucosal irregularity (ulceration) and adjacent fat stranding in the caecum b-Ruptured liver abscess with peri hepatic collection c-Extension of abscess into pleural space with mild right pleural effusion and sub segmental collapse of basal segments.
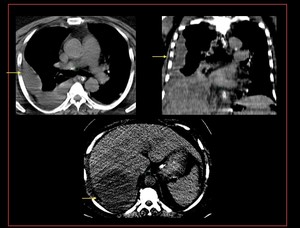
Fig. 41: Ruptured amoebic abscess with loculated pleural effusion (possibly empyema) : Non contrast axial CT demonstrates, loculated pleural effusion. The axial section of the abdomen demonstrates hypodense lesion lesion contigous with the pleural effusion.
2. MALARIA
Adult respiratory distress syndrome (ARDS) is the primary manifestation of malaria in the lung
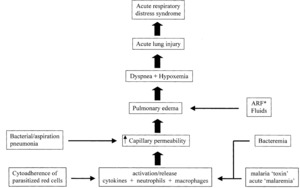
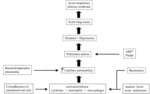
Fig. 42: Pathogenisis
References: https://posterng.netkey.at/esr/viewing/index.php?module=viewing_poster&task=imagegallery&pi=143416&mediafile_id=768770&backURL=index.php%253Fmodule%253Dviewing_poster%2526task%253Dviewsection%2526pi%253D143416%2526ti%253D515309%2526si%253D1720
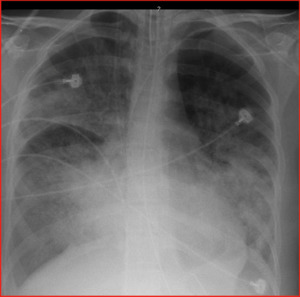
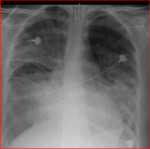
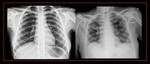
Fig. 43: A case of malaria in acute respiratory distress syndrome. Chest radiograph demonstrates bilateral predominantly peri hilar confluent air space opacification.
3. TRYPANOSOMIASIS
Acute manifestations of trypanosomiasis are uncommon and include a febrile illness with facial or unilateral palpebral oedema (“Romaña sign”) and acute myocarditis.
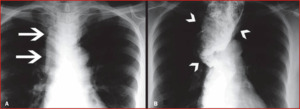
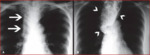
Fig. 44: Grade IV megaesophagus. A: Posteroanterior X-ray showing widening of the superior mediastinum (arrows). B: Barium swallow examination demonstrating a dilated and tortuous esophagus (arrowheads)
References: http://www.scielo.br/scielo.php?script=sci_arttext&pid=S0100-39842016000600358
4. HYDATID
Clinical features:
When pulmonary hydatid cysts rupture and communicate with bronchioles, patients are described to cough up 'grape skin' like material.
Imaging features :
|
Site- Predominantly found in the lower lobes
|
- Multiple or solitary cystic lesion (most common)
Uncomplicated cysts are characterized by:
- Round or oval masses with well-defined borders showing post contrast enhancement
Complicated cysts may show:
- Meniscus sign or air crescent sign
- Cumbo sign or onion peel sign
- Water-lily sign
- Consolidation adjacent to the cyst (ruptured cyst)
|
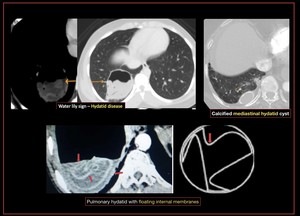
Fig. 45: Pulmonary hydatid cysts
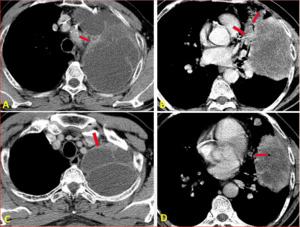
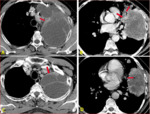
Fig. 46: Pulmonary hydatid with intrabronchial communication (A,B,C), Image D showing air within cyst secondary to bronchial communication
5. ASCARIASIS
Clinical features:
Loeffler’s Syndrome- is characterized by fever, cough, sputum, asthma, eosinophilia, and infiltrates seen at chest radiography.
Imaging features:
- Migratory, patchy alveolar infiltrates that characteristically clear within 10 days.
- Lobar consolidation and alveolar haemorrhage have also been described
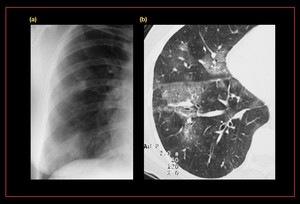
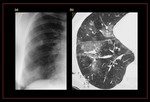
Fig. 47: Ascariasis in a 35-year-old man with migratory infiltrates. (a) Chest radiograph shows areas of ground-glass increased opacity in the right lower and middle lobes. (b) High-resolution CT scan shows areas of ground-glass attenuation that correspond to the findings in a. The resolution of radiologic findings 1 week later demonstrated the transient nature of the disease. Larvae and eggs of A lumbricoides were found at bronchoalveolar lavage and in a fecal smear, respectively, during the acute stage.
References: https://pubs.rsna.org/doi/full/10.1148/rg.251045043#F14A
3.4 PARASITOSIS OF THE MUSCULOSKELETAL SYSTEM
1. CYSTICERCOSIS
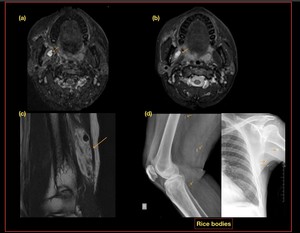
Fig. 48: Myocysticercosis
(a,b) T2 hyper intense cystic lesion with eccentric nodule.
(c) Myocysticercosis in the triceps muscle (d) Rice bodies
2. HYDATID BONE DISEASE
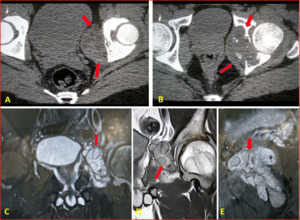
Fig. 49: Bone hydatid cyst: Axial CT scans demonstrates partial destruction of the acetabulum with adjacent soft tissue component with cystic areas within. (C,D,E) MRI images in same patient demonstrates Cystic lesion with daughter cysts within suggestive of bony hydatid cyst
3. DRACUNCULIASIS
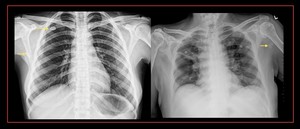
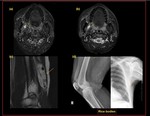
Fig. 50: Calcifications seen in the right axilla and in the right infraclavicular region suggestive of parasitic (dracunculiasis)/nodal calcification.



![Fig. 5: Layers of hydatid cyst References: Díaz A. Immunology of cystic echinococcosis (hydatid disease). [Internet]. Semanticscholar.org. 2020 [cited 14 January 2020]. Available from: https://www.semanticscholar.org/paper/Immunology-of-cystic-echinococcosis-(hydatid-D%C3%ADaz/2f1b2d733f4461d6301efda59d922675c9c62abb/figure/0](https://epos.myesr.org/posterimage/esr/ecr2020/154829/media/868072?maxheight=150&maxwidth=150)