Common Imaging Findings
Abdominal wall endometriosis may be identified at different imaging modalities, both in symptomatic as well as asymptomatic patients. Imaging findings combined with clinical history are important for the diagnosis.
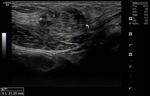
Ultrasound (US) is usually the first imaging examination. However, features are nonspecific and there is wide spectrum of differential diagnosis.
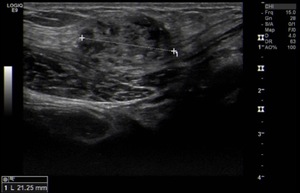
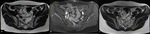
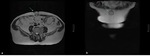
Fig. 1: Anterior abdominal wall solid lesion in a 29-year-old woman with a history of cesarean delivery. It was surgically removed and pathology confirmed an endometriotic implant.
References: Department of Radiology, Hospital da Luz de Lisboa/ Lisboa 2019
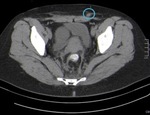
Computer tomography (CT) may help to confirm the presence of a tissue or cystic mass in abdominal wall and defining its extent. Nevertheless, findings may also be nonspecific.
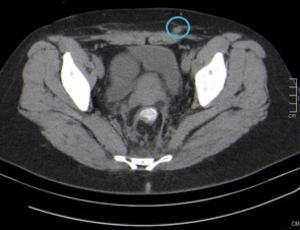
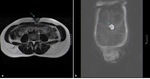
Fig. 2: Anterior abdominal wall solid lesion in a 34-year-old woman with a previous cesarean delivery. It was also investigated with MRI and was compatible with an endometriotic implant.
References: Department of Radiology, Hospital da Luz de Lisboa/ Lisboa 2019
Magnetic resonance imaging (MRI) is the cross-sectional modality of choice. It provides better contrast resolution, being superior for depicting infiltration of abdominal and pelvic wall structures. It can also be used to identify hemorrhagic content associated with endometriotic lesions.
MRI signal characteristics reflect the varying degrees of haemorrhage, fibrosis and inflammation.
Endometriosis lesions most commonly appear as a hyperintense heterogeneous nodule in abdominal or pelvic wall on both T1WI, T1FSWI and T2 WI, due to subacute hemorrhage within the endometriotic crypts and the presence of methaemoglobin. Absence of these high signal on T1 WI and T1 FSWI might be caused by hormonal treatment.
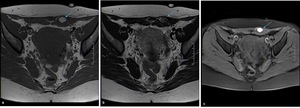
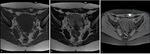
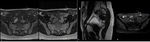
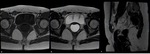
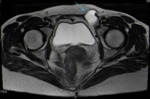
Fig. 3: Anterior abdominal wall endometriotic implant in a 32-year-old woman with a history of previous cesarean delivery and complaining of a lump in the lower abdominal wall. Axial T1WI (a), T2WI (b) and T1 FSWI (c) showing a nodule (blue arrow) displaying the “shading sign”, with high signal on T1WI and T1 FSWI and lower signal on T2WI.
References: Department of Radiology, Hospital da Luz de Lisboa/ Lisboa 2019
Scar endometriosis may also be isointense relative to muscle on T1WI due to fibrosis. In chronic scar endometriosis, lesions may have spiculated margins and low signal intensity on T2WI due to dominance of fibrotic and hemosiderotic components.
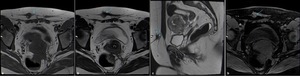
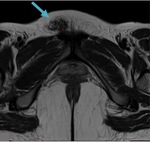
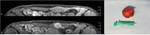
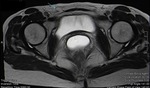
Fig. 4: Anterior abdominal wall endometriotic implant in a 36-year-old woman with a history of a previous cesarean delivery. Axial T1WI (a), axial T2WI (b), sagittal T2WI (c) and T1 FSWI (d) showing a spiculated nodule (blue arrow) displaying isointensity relative to muscle on T1WI and T1 FSWI and also low signal intensity on T2WI, consistent with chronic scar endometriosis.
References: Department of Radiology, Hospital da Luz de Lisboa/ Lisboa 2019
Usually at least a portion of the lesion demonstrates enhancement with gadolinium, most commonly at periphery.
Abdominal Wall Endometriosis
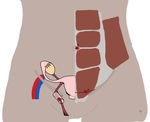
In order to avoid missing AWE, we find it important to pay close attention to the most common locations: cesarean scar, umbilicus, the inguinal region that include Nuck canal. As lesions can also be found on the abdominal wall without a previous surgical procedure, its whole extension should be reviewed.
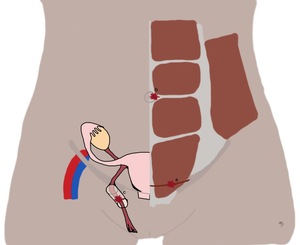
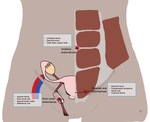
Fig. 5: Drawing of the female abdominal wall showing the most common locations of abdominal wall endometriosis (a – cesarean scar endometriosis; b – umbilical endometriosis; c – Nuck canal endometriosis).
References: Catarina Mira/ Lisboa 2019
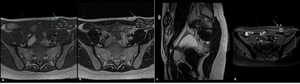
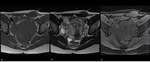
Fig. 6: Anterior abdominal wall endometriotic implant in the left rectus abdominis muscle on a 30-year-old woman with no history of previous surgery. Axial T1WI (a), axial T2WI (b), sagittal T2WI (c) and T1 FSWI (d) showing a nodule (blue arrow) with hyperintense foci on both T1WI and T2WI consistent with an endometriotic implant.
References: Department of Radiology, Hospital da Luz de Lisboa/ Lisboa 2019
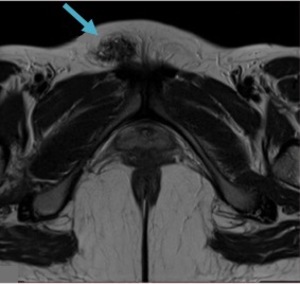
Fig. 7: Prepubic endometriotic implant on the pubic area of a 30-year-old woman who presented with a painful nodule. Axial T2WI shows a heterogeneous irregular nodule in the pre-pubic fat (blue arrow). At surgery it proved to be an endometriotic implant.
References: Department of Radiology, Hospital da Luz de Lisboa/ Lisboa 2019
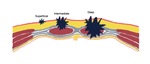
Lesions can be superficial, intermediate, and deep.
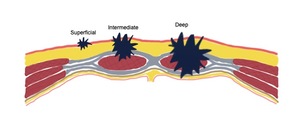
Fig. 8: Scheme of the abdominal wall showing the classification of abdominal wall endometriosis based on the level of infiltration. Lesions can be superficial (in subcutaneous tissue only), intermediate (infiltrating the abdominal rectus muscle fascia), and deep (in the abdominal rectus muscle, below fascia).
References: Catarina Mira/ Lisboa 2020
Cesarean Scar Endometriosis
Cesarean scar endometriosis is the most common type of AWE and is best explained by the iatrogenic direct implantation of endometrial tissue during cesarean delivery.
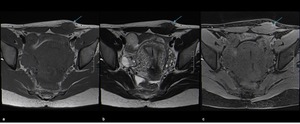
Fig. 9: Anterior abdominal wall endometriotic implant in a 29-year-old woman with a history of a previous cesarean delivery. Axial T1WI (a), T2WI (b) and T1 FSWI (c) showing a hypointense nodule (blue arrow) displaying small hyperintense foci on T1WI consistent with an endometriotic implant.
References: Department of Radiology, Hospital da Luz de Lisboa/ Lisboa 2019
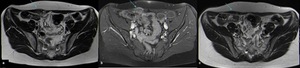
Fig. 10: Anterior abdominal wall endometriotic implant in a 42-year-old woman with a history of a previous cesarean delivery. Axial T2WI (a) and axial T1FS with gadolinium (b) show a heterogeneous nodule on the right abdominal wall infiltrating the rectus abdominis muscle. Axial T2WI (c) after one year of hormonal therapy shows its disappearance.
References: Department of Radiology, Hospital da Luz de Lisboa/ Lisboa 2019
Umbilical Endometriosis
The incidence of umbilical endometriosis has been estimated between 0,4% to 4% of all patients with endometriosis and accounts for up to 30–40% of all cases of cutaneous endometriosis. It is the most common site of primary cutaneous endometriosis, although it is more commonly secondary, due to iatrogenic dissemination.
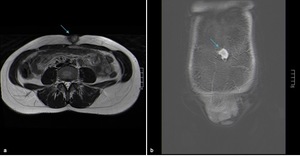
Fig. 11: Umbilical endometriotic implant in a 41-year-old woman. Axial T2WI (a) and coronal T1 FSWI (b) showing a heterogeneous nodule on the umbilicus (blue arrow) displaying the “shading sign” with high signal on T1WI and T1 FSWI and lower signal on T2WI.
References: Department of Radiology, Hospital da Luz de Lisboa/ Lisboa 2019
Nuck Canal Endometriosis
A very uncommon site of AWE is the Nuck canal, an embryological remnant of the processus vaginalis that accompanies the round ligament and extends from the inguinal canal into the vulva. The possible pathogenesis of inguinal endometriosis is direct extension of endometrial tissue along the round ligament.
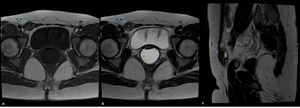
Fig. 12: Nuck canal implant in a 41-year-old woman. Axial T1WI (a), axial T2WI (b) and sagittal T2WI (c) showing a hypointense nodule (blue arrow) displaying small hyperintense foci on T1WI consistent with an endometriotic implant.
References: Department of Radiology, Hospital da Luz de Lisboa/ Lisboa 2019
Differential Diagnosis
A wide range of pathological processes may affect abdominal wall and they can be grouped into traumatic, infectious or inflammatory, iatrogenic and neoplasic lesions.
|
Differential diagnosis of abdominal wall nodules
|
|
Trauma
|
Haematoma
|
|
Infection or inflammation
|
Abscess, endometriosis, sebaceous cyst
|
|
Iatrogenic causes
|
Incisional hernia, suture granuloma, seroma, keloid, retained surgical material
|
|
Neoplasic
|
Desmoid tumor, metastasis, lipoma, linfoma, neurofibroma
|
Table 1 – Differential diagnosis of abdominal wall nodules
The most important differential diagnosis of cesarean scar endometriosis is desmoid tumor. The most most valuable clues include a history of cesarean section, typical imaging findings, as well as the potentially cyclical nature of symptoms. The most common location of abdominal wall desmoid is the infra-umbilical rectus sheath and prior surgery, pregnancy, and hormone replacement are also risk factors. As imaging features may overlap, pathologic confirmation may be necessary.
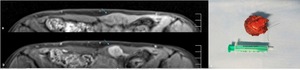
Fig. 13: Anterior abdominal wall lesions infiltrating the left rectus abdominis muscle on a 38-year-old woman. Axial T1 FSWI before (a) and after gadolinium (b) show a hypointense nodule (blue arrow) displaying enhancement after gadolinium. It was surgically removed and pathology confirmed a desmoid tumor (c).
References: Department of Radiology, Hospital da Luz de Lisboa/ Lisboa 2019
Not only benign but also malignant entities can manifest as umbilical nodules. The most common benign entity is the umbilical hernia, while malignant differentials include Sister Mary Joseph node, melanoma, sarcoma and lymphoma. Both imaging and clinical features are usually clarifying.
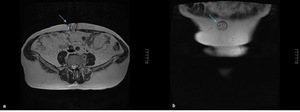
Fig. 14: Umbilical hernia on a 42-year-old woman who felt a lump in the umbilical region. Axial (a) and coronal T2 WI (b) show umbilical herniation of peritoneal fat.
The most frequent differential diagnosis of Nuck canal endometriosis are inguinal hernia and Nuck cyst. Association of symptoms with menstruation is strongly suggestive of endometriosis and imaging findings are also illustrative.
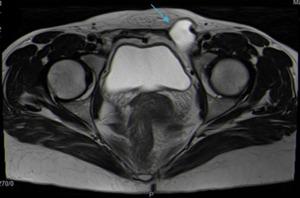
Fig. 15: Nuck cyst in a 40-year-old woman. Axial T2WI shows a thin-walled cystic lesion with proximal part of the lesion extending into the peritoneal cavity along the route of the round ligament and the distal part extending towards the labium majus.
References: Department of Radiology, Hospital da Luz de Lisboa/ Lisboa 2019
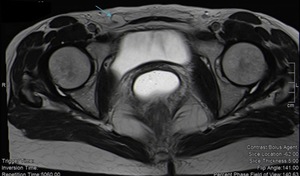
Fig. 16: Inguinal hernia in a 37-year-old woman. Axial T2WI shows right inguinal hernia (blue arrow) with herniation of epiploic fat.
References: Department of Radiology, Hospital da Luz de Lisboa/ Lisboa 2019
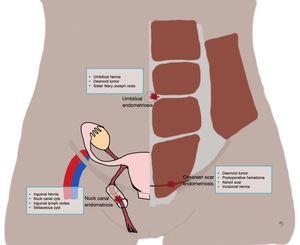
Fig. 17: Drawing of the female abdominal wall showing the most common locations of abdominal wall endometriosis and the most important differential diagnosis.
References: Catarina Mira/ Lisboa 2020