In this work we review the added value of 3D imaging (STL files, as a virtual model or for 3D printing) in pediatric cases.
The radiological challenges that we are going to analyze are the following:
1. Can I theoretically simulate the end result of surgery?
2. Can I practice with a model that is true to reality?
3. Can I understand the distribution of different structures that are in different planes of space at the same time?
4. Can I have a comprehensive view of different imaging techniques in a single image?
Case 1.
Abdominal tumor (fetus in fetu). 1 y.o. male with prenatal diagnosis of retroperitoneal mass. It has a sub-hepatic mass that does not condition vital commitment. Given the stability, deferred surgery is planned.
In this case, both virtual planning and printing for the operating room were performed. The challenge in this case was that the lesion compressed and significantly displaced major vessels such as cava or renal vein.
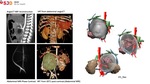
In Fig. 3 we can see the multiplanar coronal reconstruction in MPR that allows the diagnosis of "fetus in fetu".
In Fig. 4 we can see different MIP and VRT representations of CT and MRI as well as an MRI vascular study. Multi-planar projections allow to assess the relationship of the tumor with vascular structures. Although, STL segmentation is what allows us to rotate the problem area in different projections. It also allows to obtain transparencies, so that some areas are "removed" and you can see what structures are on the other side of the lesion. In this case it was helpful to understand the relationship with the cava vein and to know the location of the solid part of the hamartoma.
In Fig. 5 we can see the correspondence between the virtual model, as well as the printed model and the tumor.
Case 2.
6-year-old male patient diagnosed with retroperitoneal grade IV neuroblastoma. Presents retroperitoneal recurrence.
Fig. 6 shows a coronal representation in MPR, VRT and a segmentation of the problem tissues (vascular and tumor) projected in the VRT. These representations allow to have important information of the vascular relations of the tumor and the volume can even be calculated. However, being able to work with the STL model ( Fig. 7 ), allows predicting the percentage of residual disease based on the areas that are resected.
Fig. 8 belongs to another patient. Anatomical reliability must be sufficient. In this case, the thickness of the cut as well as the respiratory movements produce the effect of stairs in the model. However, it was enough for the surgeon to raise the approach.
Case 3. Chaos (congenital high airway obstruction syndrome). Prenatal ultrasound diagnosis of patient affected by airway obstruction.
Gynecologists propose to perform fetoscopy and repermeabilization of the airway with laser.
The radiological challenge was to be able to perform a fetal MRI study to segment the trachea and generate a 3D model. Fetal MRI is a complex technique, where the moving fetus can prevent diagnostic imaging. On the other hand, minimal spatial resolution must be obtained. Finally, we must remember that in this type of surgery time is crucial, so all image steps must be quick and effective.
From the T2 sequences in the coronal plane ( Fig. 9 ), both the trachea and the lungs could be segmented. Later, when reconstructing the model, the engineer generated the appearance of an empty tube to give the most "known" anatomical aspect. Fig. 10 shows the result of fetal MRI segmentation.
For laser surgery by fetoscope, the acting time is very short (minutes). There is also a limitation in the fetoscope itself when it comes to angulation. Therefore, it was necessary to know the angle of entry and also be able to practice if the fetoscope would pass through the canal. Fig. 11 shows the comparison between 2D and STL.
Case 4. Galen vein malformation in a neonate.
This case is particularly illustrative to explain the advantages of using STL models in the case of combining different image techniques. By converting segmented areas into objects, regardless of origin, you can unify all in a single virtual space.
Fig. 12 MR sequences used for the segmentation of the case.
Fig. 13 Combination of sequences in one STL. We can observe the relationship of the arteries with the healthy aneurysm.
Case 5. 11-year-old woman diagnosed with right microtia
In this case, a specular mold of the healthy ear was prepared so that the plastic surgeon could use in the design of the cartilage during surgery ( Fig. 14 ).
Case 6. Right aortic arch.
Segmentation and subtraction allowed to observe a tracheal stenosis. Fig. 15
Case 7. 10-month-old female patient, with a cloaca (ano-rectal malformation).
In this patient, an enema with gadolinium diluted at different concentrations was performed. He was subsequently moved to the MRI. Fig. 16 .
Other challenge was the segmentation itself. Currently, automatic RM segmentation may have certain limitations depending on the software.
Finally, we were able to obtain a virtual 3D study and we were able to calculate the necessary distances for anal reconstruction. Fig. 17 .
Case 8. Unilateral micrognatia (Pruzanski 1). 9 year old woman with Goldenhar syndrome (left hemifacial microsomy).
Orthognathic correction surgery is planned, using conventional facial CT ( Fig. 18 ).
This case of maxillofacial surgery allows us to illustrate two aspects of the use of virtual 3D.
- On the one hand, having "objects" allows non-standard views of structures, such as the upper view of the lower jaw.
- On the other hand, it allows to simulate the final result: creating a "mirror" jaw ( Fig. 19 ) and performing calculations that allow creating osteotomies and even the final position of the bone segments ( Fig. 20 ).