Gray-scale US
On US images, the normal bowel has a mural thickness measuring up to 3-5 mm and a stratified morphology of five concentric rings, called gut signature.
Each of the rings corresponds to a different layer: the innermost one appears as an echogenic line, representing the interface between the lumen and the mucosa, followed by an adjacent hypoechoic ring (muscularis mucosa), an echogenic ring (submucosa), a hypoechoic ring (muscularis propria), and an outermost echogenic ring (serosa) (Fig.1) [4,5].
During the exam, the wall thickness and the gut signature of the bowel should be assessed, documenting any interruption of the normal layers, which can be better evaluated with a specific “bowel” preset that provides higher contrast images [4,6].
Normal bowel loops are easily compressible and show normal peristalsis, whereas abnormal bowel loops are thickened with reduced or absent peristalsis.
A curvilinear transducer should be used for an initial overview of the bowel to detect thickened loops, lymphadenopathy, inflamed perienteric fat and fluid collections. During the exam, particular attention should be paid to the site of tenderness or pain of the patient [4,5].
The US examination can be subsequently performed with a high-frequency probe to further examine the suspected abnormal loops because it increases the resolution of the bowel wall layers and adjacent tissues. However, the visibility depends on the body habitus of the patient and the depth of the loops [4].
On grey-scale US, an uncomplicated diverticulum appears as a hypoechoic saccular outpouching of the colon, containing heterogeneous echogenic foci, air and fecalith, with distal acoustic shadowing. The surrounding fat has normal echogenicity.
In case of diverticulosis, the hypoechoic muscularis propria layer may be thickened due to muscular hypertrophy.
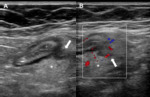
In diverticulitis, the inflamed diverticulum appears as a sac-like outpouching, characterized by hypoechoic thickening of the muscularis propria; a segmental thickening of the colonic wall (>5mm) is usually seen. The adjacent, inflamed, perienteric fat appears echogenic and thickened most of the times (Fig.2A) [4,6,7].
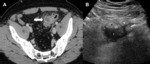
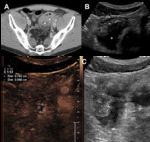
In case of severe inflammation, the normal gut signature may be disrupted (Fig.3A,B) [4]. The bowel loops that appear abnormal in one plane should be assessed also in the orthogonal plane to avoid misinterpretations, and, when an abnormal loop is confirmed, the length of the alteration should be documented [4,6].
In complicated diverticulitis, an abscess or phlegmon can be differentiated from free peritoneal fluid, which easily changes in shape and location with sonographic compression. The differentiation between abscess and phlegmon is instead challenging because both appear as hypoechoic non-mobile masses (Fig.4) [4,6,8].
The ultrasonographic patterns of bowel obstruction are divided into early signs (thin gut, hyperperistalsis, to-and-fro movement) and late signs (aperistalsis, thickened wall). The peristalsis of abnormal loops should be documented using cine US images (Fig.5) [4,6].
Fistula is an abnormal communication between a thickened bowel loop and an adjacent organ. It appears as an echogenic tract, if it contains gas, or a hypoechoic one, if it contains debris [4,6].
Color Doppler US
Information about mural vascularity of the bowel and surrounding fat can be provided by Color Doppler assessment. However, the bowel wall vasculature is characterized by a low-velocity flow, which is not always detectable, and motion artifacts from peristalsis may also occur. Therefore, a careful interpretation of the images is required.
On color Doppler US, hyperemia of the thickened bowel loops and of the surrounding fat may be present due to inflammation [4,6] (Fig.2B).
Contrast agent–enhanced US (CEUS)
CEUS is performed after a bolus intravenous injection of an US contrast agent consisting of microbubbles with a phospholipid shell. The use of this agent increases the US signal and allows the evaluation of the bowel vasculature.
Bowel hyperemia can be assessed by the enhancement of the wall. CEUS also plays an important role in differentiating a phlegmon from an abscess. Both these lesions appear as hypoechoic non-mobile masses on gray-scale US, but have different enhancement patterns: the first, a vascularized area of acute soft tissues inflammation, may show homogenous enhancement, whereas the latter, a non-vascularized loculated fluid collection, may show intense enhancement only in the peripheral area, representing the abscess wall (Fig.3C,6,7) [8].