The histological abnormalities diseases that characterize drug-induced lung injury generally involve the pulmonary interstitium.
Drugs can produce all histopathological patterns of interstitial pneumonia and include diffuse alveolar damage, nonspecific interstitial pneumonia and organizing pneumonia as the most frequent; eosinophilic pneumonia, pulmonary edema o hemorrhage, and hypersensitivity pneumonia are less common.
DIFFUSE ALVEOLAR DAMAGE (DAD)
It is the most frequent manifestation of histologically confirmed lung toxicity.
It is a manifestation of pulmonary toxicity secondary to necrosis of type II pneumocytes and alveolar endothelial cells.
The drugs that most frequently produce DAD are cytotoxic chemotherapeutic agents: bleomycin, busulfan, BCNU, cyclophosphamide, paclitaxel, docetaxel, melphalan although it can also appear with amiodarone, aspirin, cocaine, narcotic analgesics, methotrexate, mitomycin and gold salts.
There are two histopathological phases in DAD: an acute exudative phase and a repair phase. The exudative phase occurs in the first week and is characterized by the presence of edema intra-alveolar membranes. The reparative phase occurs after one or two weeks and is characterized by the proliferation of type II pneumocytes and fibrosis. DAD can progress to fibrosis although it can be reversible.
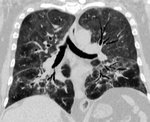
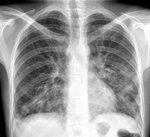
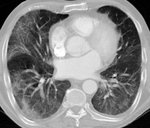
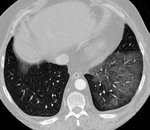
In early drug-induced DAD, the chest radiograph is often normal.
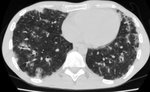
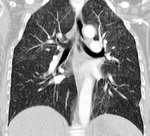
The HRCT initially shows patchy or diffuse bilateral ground-glass opacities that tend to the confluence with or without thickened interlobular septa opacities (crazy-paving pattern) and then consolidations appear in gradient areas. Progressively, fibrosis findings appear as architecture distortion, traction bronchiectasis or honeycomb. The affectation predominates in pulmonary bases.
USUAL INTERSTITIAL PNEUMONIA (UIP)
Cytotoxic chemotherapeutic drugs are the ones most frequently associated with NIU such as bleomycin and methotrexate.
In HRCT initially patchy or diffuse ground-glass areas may appear. Subsequently, there may be findings of fibrosis such as traction bronchiectasis and subpleural thick-walled cystic spaces (honeycomb) of basal predominance.
NON-SPECIFIC INTERSTITIAL PNEUMONIA (NSIP)
It is the most common form of fibrosing pneumonia that is associated with a drug reaction.
NINE is characterized by mononuclear cell infiltrates, mild interstitial fibrosis and hyperplastic type II pneumocytes. The typical histological pattern of NINE is a uniform process. Interstitial inflammation is more cellular and homogeneous than in cases of usual interstitial pneumonia.
The drugs most frequently associated with NINE are amiodarone, bleomycin, methotrexate, and BCNU.
The predominant pattern consists of bilateral patchy ground-glass areas that can associate fine reticulation, traction bronchiectasis, and bronchiectasis. The findings are often diffuse although there may be a baseline predominance. It can progress to fibrosis.
ORGANIZING PNEUMONIA (OP)
It is characterized histopathologically by fibroblastic plugs (Masson's bodies) in respiratory bronchioles, alveolar ducts, and alveolar spaces.
The drugs that are most frequently associated with OP are bleomycin, methotrexate, cyclophosphamide and gold salts.
The HCRT shows as the most common pattern bilateral patchy consolidations of subpleural and peribronchial distribution. They are usually bilateral and asymmetric and usually contain air bronchograms with dilated airways; often they associate nodular opacities and ground-glass with a lobular or mosaic distribution. Nodular ground-glass is typically diagnosed in patients exposed to bleomycin, mainly located in the lung bases.
EOSINOPHILIC PNEUMONIA (EP)
The reaction to drugs is one of the most frequent causes of eosinophilic lung disease. An insidious course with progression over several months is the more frequent presentation but may have an acute course.
Histologically it is characterized by the accumulation of eosinophils and macrophages in the alveolar spaces.
The drugs that are most frequently associated with EP are penicillamine, sulfasalazine, nitrofurantoin, para-amino-amino acid, and non-steroidal anti-inflammatory drugs.
Radiologically, it manifests as subsegmental bilateral consolidation areas, often in the pulmonary periphery and predominantly in the upper lobes. Opacities tend to be migratory.
The negative pattern of pulmonary edema is rare.
HYPERSENSITIVITY PNEUMONITIS (HP)
It is a rare manifestation of pulmonary toxicity by drugs.
An important histological finding of HP is the presence of small interstitial granulomas with some giant cells, caused for example by anti-TNF drugs, methotrexate, and BCG therapy.
The best-known cause is the treatment with low doses of methotrexate although it has also been described in treatments with cyclophosphamide, mesalamine, fluoxetine, amitriptyline, and paclitaxel.
The findings in HRCT are bilateral ground-glass opacities and poorly defined centrilobular nodules. Most patients have lobular areas of decreased attenuation and vascularization on inspiration and air trapping in expiration (mosaic pattern).
The nodular pattern becomes more prominent in the subacute phase. In chronic HP, fibrosis with retraction in the upper lobes, reticular opacities, and honeycomb can be observed.
PULMONARY HEMORRAGY
It is a rare complication but with significant morbidity and mortality. Hemoptysis is not frequent.
The drugs most frequently associated with pulmonary hemorrhage anticoagulants, fibrinolytic, amphotericin B, high dose cyclophosphamide, mitomycin, cytarabine and penicillamine
The chest radiograph shows a disseminated condensation of rapid onset that, with favorable evolution, can disappear quite quickly. HRCT shows bilateral ground-glass opacities, disseminated or diffuse.
The new molecular therapies act specifically against cell membranes and intracellular molecules. They can be used alone or in combination with classical chemotherapy. The toxicity of these therapies is different from classical cytostatics and they differ in clinical and radiological presentation.
The new anti-EGFR drugs can induce ground-glass infiltrates that should not be considered tumor progression.
Treatment with bevacizumab can cause severe pulmonary hemorrhage.
Interleukin 2, interferon and gemcitabine therapies can increase capillary permeability and the differential diagnosis with pulmonary edema should be established since it requires corticosteroid therapy in addition to diuretics.
Docetaxel may cause acute interstitial pneumonitis when used as monotherapy or in combination with gemcitabine causes a higher incidence of UIP or DAD.
Paclitaxel can cause HP. This probability increases if combined with radiation therapy.
The incidence of pneumonitis is higher if irinotecan is combined with paclitaxel or radiotherapy. The combination of cisplatin with irinotecan and radiotherapy increases the likelihood of pulmonary fibrosis.