PRIMARY DEMYELINATION
Ia. MULTIPLE SCLEROSIS:
Ia (i). Classic type:
It is a chronic persistent inflammatory demyelinating disease of the central nervous system.
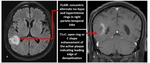
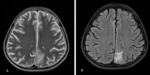
The MR imaging findings in brain include; plaques which are hyperintense on T2 and proton density images. These are round to oval in shape whose major axis is oriented perpendicular to outer surface of the lateral ventricle ranging in size from few millimetres to more than 1 cm. These lesions are discrete and focal in early stages. The more severe the demyelination; axonal loss and irreversible tissue damage is seen as T1 hypointensity which are also called T1 black holes.
The specific locations of involvement are the periventricular white matter supero-lateral to the lateral angles of the ventricles (Dawson’s fingers), calloso-septal interface along the inferior surface of the corpus callosum, cortico-juxtacortical regions the (subcortical U fibres), focal involvement of the periventricular white matter in the anterior temporal lobes (typical of multiple sclerosis), floor of the fourth ventricle, middle cerebellar peduncle and brainstem (contiguous with cisternal or ventricular space). These plaques show incomplete ring enhancement with open border facing the gray matter of the cortex or basal ganglia.
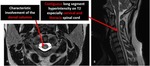
The MR imaging findings in spinal cord have predilection for lateral and posterior white matter columns in cervical cord.
The optic nerve involvement is less common in multiple sclerosis. If involved it is seen as focal thickening which is better appreciated on coronal fat saturated T2 W imaging.
Ia (ii) Marburg disease: Large T2 hyperintense plaques disseminated throughout hemispheric white matter and brain stem.
Ia (iii) Schilder's disease: Large incomplete ring enhancing lesions symmetrical in parieto-occipital regions sparing brain stem.
Ia (iv) Balo concentric sclerosis: Alternating bands of T2 hyperintensity show concentric hyperintense bands(demyelination and gliosis) alternating with isointense bands (normal myelinated white matter) giving floral configuration.
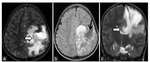
Ia (v). Tumefactive Multiple Sclerosis: Large single or multiple focal lesions within cerebellar hemispheres with minor mass effect showing incomplete ring enhancement and rim of peripheral hypointensity on T2 WI.
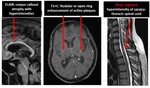
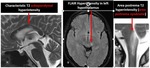
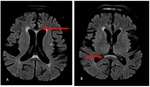
Ib. NEUROMYELITIS OPTICA SPECTRUM DISORDER: The specific locations of involvement in brain include (a) areas rich in AQP4 i.e., subpial, periependymal regions, circumventricular organs, corpus callosum (along ependymal surface giving typical marbled appearance), periaqueductal area, surrounding 3rd and 4th ventricles, thalamus and hypothalamus, (b) non-AQP4 rich region such as cortico-spinal tract (44%). There will be cloud like pattern and pencil thin ependymal lining enhancement.
There is involvement of both the optic nerves with predilection for posterior optic pathway. There is thickened and T2 hyperintense optic nerves with enhancement in acute phase and atrophy in chronic phases.
The spinal cord show T2 hyperintensity in more than 3 contiguous vertebral segments with central gray matter involvement along the central canal.
II SECONDARY DEMYELINATION:
IIa. Due to infectious agent or vaccination:
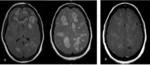
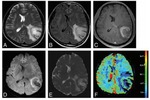
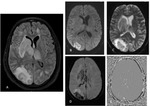
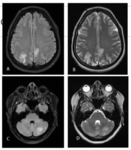
1. Acute Disseminated Encephalomyelitis: It is severe immune mediated inflammatory disorder of CNS triggered by inflammatory response to virus or bacteria or vaccination with a latency of 7-14 days. The MR findings in brain include large patchy, asymmetrical and poorly marginated lesions with specific locations of involvement being subcortical and central white matter, cortical gray - white junction, cerebellum and grey matter of thalami and basal ganglia (symmetrically involved in children).
The spinal cord shows large cord lesion with oedema and enhancement having thoracic spinal cord predilection.
IIa 2. Acute Haemorrhagic Leukoencephalopathy: Multifocal asymmetrical areas of high signal on T2 in cerebral white matter with strict sparing of subcortical U fibres with haemorrhage.
IIa 3. Progressive multifocal leukoencephalopathy: Multifocal ill-defined and asymmetric areas of T2 hyperintensity in subcortical and periventricular white matter with subtle or no enhancement which expand along white matter tracts. The optic nerve and spinal cord are usually spared.
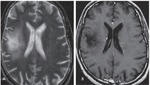
IIa 4. HIV encephalopathy: Diffuse cerebral atrophy; symmetrical, patchy or confluent areas of T2 hyperintensity within periventricular and deep white matter with no enhancement or mass effect.
IIa 5. Subacute sclerosing panencephalitis: T2 high signal areas in periventricular and subcortical white matter with mass effect. Diffuse cerebral atrophy on chronic stage.
IIb. Secondary demyelination due to vitamin deficiency:
1. Central pontine myelinolysis: This is seen when hyponatremia is rapidly corrected. The characteristic MR finding is described in Figure No., 14.
II b 2. Marchiafava-Bignami Syndrome: Corpus callosal (central) hyperintensity in FLAIR and T2 weighted sequence showing enhancement in acute phase and atrophy in chronic phase.
II b 3. Subacute combined degeneration of the spinal cord: T2 hyperintensity in posterior and lateral columns of spinal cord. These lesions are reversible after adequate vitamin B12 administration.
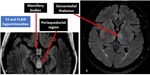
IIb 4. Wernicke's encephalopathy: This is an acute condition caused due to deficiency of thiamine. At MRI, bilateral and symmetrical hyperintensities on T2 and FLAIR in periaqueductal gray matter, colliculi, mamillary bodies, thalami, pulvinar regions, third cranial nerve nuclei and cerebellum. Marked enhancement in mamillary bodies is highly specific finding.
IIc. Radiation and chemotherapy induced demyelination: The radiation effects are more severe in combination with chemotherapy. The chemotherapeutic agents implicated in demyelination are methotrexate, cytarabine, carmustine, cyclophosphamide, cisplatin and fludarabine.
IId. Demyelination due to vascular causes:
IId 1.CADASIL (cerebral autosomal dominant arteriopathy with subcortical infarcts and leukoencephalopathy): Symmetrical hyperintensities on T2 weighted sequence in subcortical and periventricular white matter with microbleeds.
IId 2. PRES (Posterior reversible encephalopathy syndrome): It is a disorder of cerebrovascular autoregulation commonly involving the posterior circulation because of sparer sympathetic supply. At MRI, T2 and FLAIR hyperintensities in regions of posterior circulation. Sometimes, the imaging show acute demyelination plaques mimicking Multiple sclerosis.