Type:
Educational Exhibit
Keywords:
Not applicable, Obstruction / Occlusion, Diagnostic procedure, Digital radiography, CT-Angiography, CT, Thorax, Lung, Chest
Authors:
N. Bhatt1, N. Chua2, N. F. Bassett1, S. mcclaggan1, V. H. lopes1; 1Luton/UK, 2London/UK
DOI:
10.26044/ecr2020/C-12772
Findings and procedure details
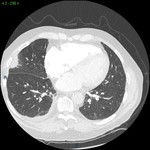
Case 1: 81 year old male with a swollen calf and shortness of breath.
The radiographic equivalent of the ‘Hampton’s hump’ as described on radiography is also seen on CT. Branches of the pulmonary artery supply the lung periphery, occlusion of which gives rise to a broad, pleural based opacification in the shape of a wedge with a truncated apex pointing towards the hilum Fig. 1.
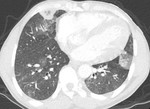
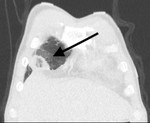
Case 2: 44 year old male with known sickle cell disease.
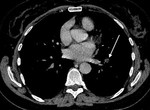
Central air lucencies within the consolidated lung gives the infarct a ‘bubbly consolidation’ appearance Fig. 2 and Fig. 3. This sign is more favourably used to make a diagnosis of infarction amongst observers [2]. However central lucencies within consolidation can also be seen due to underlying lung cystic change or cavitation which the reporter should be aware of.
No convicing thrombus was seen within the pulmonary arterial vasculature by the reporting Radiologist and the consolidation in the right middle lobe was therefore interprereted as infectious consolidation. Images were reviewed in Lung Cancer multidisciplinary team meeting (MDT) by a dedicated Chest Radiologist and recognised as pulmonary infarction. Patient was treated with anticoagulation and subsequent repeat CT confirmed resolution of infarction.
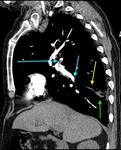
Case 3: 49 year old male with shortness of breath.
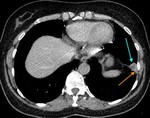
Similar to the appearance of peripheral deep venous thrombosis (DVT), thrombosed pulmonary arteries can be seen to be prominent in calibre Fig. 4. These extend towards the apex of the pleural based consolidation which when seen in conjunction supports the diagnosis of infarction.
Case 4: 47 year old female with unprovoked DVT had a staging CT chest abdomen and pelvis to exclude an underlying malignancy.
Evaluation of the pulmonary infarction on soft tissue windows demonstrate reduced enhancement of the infarcted lung tissue Fig. 5 and sometimes shows corresponding hyperenhancement of the perimeter.
The staging CT scan was performed in portal venous phase. The pulmonary arteries were not opacified and the observer failed to observe the filling defect in a branch of the left lower lobe pulmonary artery Fig. 6. Working diagnosis was a lung malignancy until the images were reviewed at Lung Cancer MDT and a correct diagnosis of pulmonary infarction was made. Follow up CT showed complete resolution of infarction following completion of anticoagulation therapy.