From 1 May to 30 September 26 patients (mean age 61 years, range 38-87 years, M:F 12: 14) underwent biopsy with standard CT guidance (control group) and 26 patients (mean age 57 years, range 31-84 years, M: F 5:21) underwent biopsy with the use of electromagnetic navigation system (navigation group). Data were retrospectively evaluated. Operators were interventional radiologists with more than 5 years of experience.
All procedures were performed using a 64 slice CT scan Prime SP Aquilion Canon Medical Systems Europe B.V. (Tokyo, Japan)
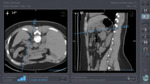
For the conventional CT intervention (control group) the ideal needle path trajectory is defined on the acquired CT scan using the CT console. The needle entry point is identified using CT gantry laser and marked on the patient’s skin, and the sterile area is set up. A local anesthetic is administered, and the radiologist carries out the procedure, iteratively verifying the correct position of the needle by acquiring control scans until the target has been reached. The control scan that shows the position of the needle at the target was considered as the “final control scan”. Any further control scans acquired after the ‘final control scan’ are not counted for this study.
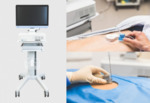
For navigation group procedures were carried out using navigation assistance supplied by IMACTIS-CT. First the navigation system is installed beside the CT scanner and connected to the network. A dedicated electromagnetic generator is attached to the skin of the patient close to the theoretical entry point, and a CT acquisition is performed. An electromagnetic receiver is attached to the non-sterile needle holder, and the images of the acquired CT scan are automatically transferred to the navigation system via the network. Automatically, the arrival of the images are detected, the coherence of the series is verified and the registration of the images is carried out (1).
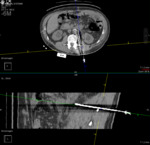
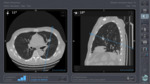
The navigation system enables the radiologist to define the ideal needle path trajectory directly on the patient by using the needle holder to navigate within the acquired CT volume. Once the ideal trajectory has been defined, the entry point is marked on the patient’s skin, and the sterile area is set up. The navigation system is then made sterile by removing the electromagnetic receiver from the non-sterile needle holder, placing the receiver in a sterile cover, and attaching it to the sterile needle holder. A local anesthetic is then administered, and the radiologist carries out the procedure using navigation assistance until the target has been reached. Control scans can be acquired at any moment. A final control scan is acquired that shows the position of the needle at the target before the procedure is continued(1). Any further control scans acquired after the ‘final control scan’ are not counted for this study. (FIG. 2, 3, 4)
In the present study were evaluated and compared between the two groups:
-the diagnostic rate;
-the number of performed scans;
-the total time between the first and the last scan;
-the radiation dose used (TDLP );
-the type of approach (axial vs non-axial).