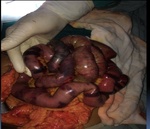
Sclerosing encapsulating peritonitis (SEP) is a rare form of peritoneal inflammation which involves both the visceral and the parietal surfaces of the abdominal cavity. SEP is characterized by a fibrous thickening of the peritoneum and is reported to complicate peritoneal dialysis, certain drugs, and infectious peritonitis.It is also called abdominal "cocoon" owing to its appearance. (FIG 1). SEP has been reported in a wide range of ages, with the youngest patient in our study being a 28 year old boy and the oldest patient being an 90-year-old woman.
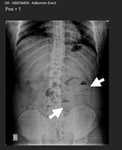
- RADIOGRAPH: The findings are usually normal but may sometimes show multiple fluid levels if there is associated bowel obstruction. Images from small-bowel follow-through studies show the bowel loops conglomerated in a concertina-like (FIG 2) fashion with a serpentine arrangement in a fixed U-shaped configuration.
- ULTRASOUND: demonstrates a “cauliflower” appearance of bowel with a narrow base, as well as a “trilaminar” appearance depicted especially with use of high-resolution US probes.
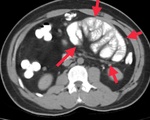
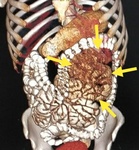
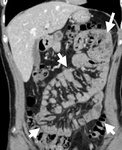
- CT is the imaging modality of choice and allows identification of the thickened contrast enhanced abnormal peritoneal membrane and the encapsulated clumped bowel loops giving a “cocoon” like appearance. In addition, CT can potentially help identify the cause of SEP (omental granuloma in tuberculosis), as well as the complications of SEP (bowel obstruction). Although nonenhanced CT may depict calcification slightly better, routine portal venous phase CT after intravenous administration of contrast material is usually sufficient to give adequate information. Administration of positive oral contrast material may help in better bowel delineation.With thin isotropic voxels and multiplanar reformation, it has now become possible to routinely depict the encapsulating membrane. The normal peritoneum is a thin, smooth, barely perceptible structure with discontinuous enhancement.In SEP, the peritoneum is thickened, with marked continuous enhancement. Assessment of peritoneal thickening is usually subjective, and no optimum threshold has been described, although a thickness greater than 2 mm appears to be a reasonable cutoff. The small-bowel loops appear congregated toward the center of the abdominal cavity and are encased by a mantle that demonstrates soft-tissue attenuation.Volume-rendered CT images are found useful in depicting the intraintestinal positive oral contrast with altered bowel configuration (Fig 8).In addition to the altered position and placement of the bowel in the abdomen, CT also helps depict changes in the contour and caliber of the bowel. Bowel thickening may or may not be demonstrated. A few of the bowel loops may appear dilated or prominent. Usually, no obvious transition point is seen. Angulation, kinking, and tethering of the bowel loops indicate extensive interbowel adhesions, which portend a poor prognosis. This information about interbowel adhesions is also important to the surgical team, as well as the anesthesia team, because the surgery is expected to be difficult and prolonged. Such interbowel adhesions are usually common in SEP with a tuberculous cause, in which case additional findings such as omental caking, mesenteric and retroperitoneal necrotic lymph nodes, and serosal tubercles may be identified at CT.(Fig 2).
Ascites, especially interbowel ascites, is common in SEP, and loculated fluid collections can be demonstrated and quantified.CT can be used to identify complications of SEP such as bowel gangrene (lack of normal bowel enhancement)and bowel perforation(pneumoperitoneum, oral contrast material extravasation).
These complications are relatively rare because the thickened peritoneal membrane encapsulates and compresses the bowel from the exterior, with preservation of the central vascular pedicle (as opposed to mimics such as internal hernia, in which the pedicle is twisted, leading to early ischemia). CT can reliably depict these complications when they occur and can help determine management. Owing to its excellent depiction of the anatomic abnormality and the complications, contrast-enhanced CT is regarded as the modality of choice in the imaging of SEP. Often, a combination of modalities is used to raise suspicion regarding SEP and to arrive at the diagnosis before surgery (Fig 9).
Management
Based on the imaging findings, conservative medical treatment and surgical therapy early in the course of EPS have been used for management of the condition. Often, Sclerosing encapsulating peritonitis has a vague clinical presentation leading to a delay in diagnosis and treatment. CECT has a relatively short study time and can be key in making a diagnosis. Since surgery is often needed to decompress the encased obstructed small bowel loops, CT imaging can
lead to prompt diagnosis, treatment, and improved patient outcomes.
Treatment plan includes surgery, bowel rest and nutritional support, lysis of adhesions, corticosteroids, tamoxifen, and immunosuppressants. Resection of the bowel is unnecessary if bowel is viable on imaging, avoiding the risk of increased morbidity and mortality associated.
Sclerosing encapsulating peritonitis can lead to serious complications such as severe malnutrition, sepsis, and death if not promptly diagnosed and treated