The recommended CT protocol for renal infections includes a nephrographic phase and an excretory phase if there is obstruction [4].
Acute pyelonephritis:
Focal form
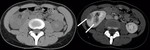
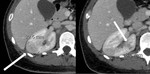
Unenhanced CT scan can shows calculi, gas, hemorrhage, calcifications, obstruction, renal enlargement (Fig.1) and inflammatory masses. Rarely CT may demonstrate some hyperdense areas in hemorrhagic bacterial nephritis, for the presence of bleeding parenchyma [5]. However, oftentimes kidneys appear normal on unenhanced scan [1] and intravenous contrast agent injection is needed to demonstrate acute nephritis (Fig. 2) [5].
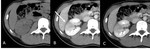
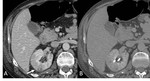
On parenchymal phase, focal pyelonephritis is characterized by a poorly-defined triangular area of hypoattenuation that extents from the papilla in the medulla to the cortical surface, with or without swelling and reduced corticomedullary differentiation [4] (Figs. 3, 4).
These typical areas are probably due to reduced fuction of parenchyma for vasospasm, tubular obstruction and/or interstitial edema [6,7], tends to have a lobar distribution and can be unifocal, bilateral or multifocal[5].
Differential diagnosis: masses, renal infarction, tumors or scarring. The hypoattenuating areas caused by infarcts and tumors persist after antibiotic whereas pyelonephritis resolves after treatment [4]. The cortical rim sign – which describes the thin, viable rim of subcapsular cortex seen on contrast-enhanced imaging – may be helpful for differential diagnosis with acute pyelonephritis: in acute pyelonephritis the abnormal areas involve a complete wedge of renal parenchyma, extending from medulla peripherally to the capsule, while in up to 50% of segmental renal infarcts there is relative sparing of the cortex where perfusion may be preserved and enhances normally (Fig. 5).
Striated CT nephrogram
Striated CT nephrogram refers to a typical appearance on delayed phase of high and low attenuation alternate linear areas parallel to the axis of the tubules and collecting ducts (Fig. 6). This pattern is not specific for pyelonephritis but it can occur in acute urinary obstruction, renal vein thrombosis, renal contusion, hypotension, medullary sponge kidney, or tubular obstruction due to myoglobinuria.
In acute tubulointerstitial infection, inflammatory cellular infiltrate increases parenchymal pressure within the affected medullary or cortex. These areas demonstrate decreased enhancement initially, and increased attenuation on delayed images compared to the adjacent normal tissue. This nephrographic reversal sign is probably due to cellular accumulation in tubules [8].
Diffuse form
Diffuse form of acute pyelonephritis may cause global enlargement, decreased enhancement of the kidney, lack of contrast excretion, thickening of Gerota’s fascia, stranding of perinephric fat and obliteration of perirenal space. [3, 4] (Fig. 7) Bulging of parenchyma may produce compression of calyces; thickening of wall of pelvis and calices could also be seen [9].
Chronic pyelonephritis
Chronic pyelonephritis is usually caused by recurrent episodes of vescicoureteral and infrarenal infected urine reflux in childhood, but it can also be due to other risk factors like calculi and chronic obstruction, neurogenic bladder, urinary diversions and other causes of stasis [1].
The typical radiologic findings of chronic pyelonephritis are focal depressions in the polar regions of the kidney with caliceal distortion, pelvicalyceal dilatation and global atrophy caused by reduced growth of the kidney due to chronic disease; compensatory hypertrophy of contralateral kidney is frequent; sometimes calculi can be find.
Differential diagnosis: Fetal lobulations are described like depressions lying between calyces rather than overlying calyces [3]. Lobar infarcts can be differentiated because of the typical cortical involvement with caliceal sparing. [2].
Subtypes and complications
Renal abscess
Acute pyelonephritis can heal with time or progress to abscess formation if it is not treated properly or the patient is immunocompromised. Lobar nephronia refers to an intermediate stage between acute pyelonephritis and renal abscess (Fig. 8).
Early abscess is characterized by an ill-defining hypodense area. A mature abscess appears as a well-defined zone of hypoattenuation with a thick, irregular wall or pseudocapsule, that demonstrate a peripheral rim enhancement after contrast injection (Fig. 9). The suspicion of an abscess is also suggested by presence of gas into a low-attenuating or cystic mass [3, 2]. Some small collections can coalesce into a single larger cavity. If there is not obstruction, the drainage of the abscess normally occurs into the calyces and ureter [1].
Perinephric abscess
A perinephric abscess may be the consequence of the rupture of a renal abscess into the perirenal space or the extra renal extension of acute pyelonephritis. Perirenal abscesses are contained within Gerota’s fascia. Risk factors are diabetes and septic emboli.
Perinephric abscesses’ appearance is a fluid or sovrafluid collection in the perirenal space with or without gas (Fig 10). Percutaneous or surgical drainage is recommended [2].
Emphysematous pyelonephritis
Emphysematous pyelonephritis is a severe necrotizing infection of the renal parenchyma usually unilateral and occurring more often in women. Risk factors are diabetes and immunocompromised status.
CT is the best modality to detect gas and define disease extension [10, 11]. CT usually demonstrates multiple small bubbles or linear bands radiating from the papilla. Large gas collections, perirenal fluid, gas–fluid levels, abscesses and parenchymal destruction can be detected [12] (Fig.11).
Emphysematous pyelonephritis can be classified in two forms with different severity, prognosis and management:
-Type 1: with severe parenchymal destruction, presence of gas and reduced pus collection for a deficient immune response. Nephrectomy is usually indicated. This type has a high mortality (80%).
-Type 2: with less parenchymal destruction, pus collections in renal parenchyma and in perirenal space and lower mortality (20%).
The main differential diagnosis that must be done by radiologists is between emphysematous pyelitis and pyelonephritis: indeed, emphysematous pyelitis (Fig. 12) is characterized by the presence of air only in the pyelocaliceal system and nephrectomy is not necessary [3].
Xanthogranulomatous pyelonephritis
Xanthogranulomatous pyelonephritis (XPG) is a rare form of chronic destructive granulomatous process of renal parenchyma associated with long-term urinary tract obstruction, infection and staghorn calculi [3]. It usually occurs in middle-aged women and it is rarely bilateral.
Symptoms are often not specific and CT is indicated for diagnosis. On CT XPG can manifest as diffuse (80%) or focal (15%) forms. Typical CT findings of the diffuse form are renal enlargement, calcifications filling the renal pelvis, and replacement of the renal parenchyma by multiple hypodense dilated calices and abscess cavities filled with pus and debris. These cavities typically present strong enhanced walls after contrast injection, due to the high vascularity of the granulation tissue and thinning of normal parenchyma (Figs. 13 and 14).
Differential diagnosis: sometimes focal XGP may present the morphology of a tumor- like cystic lesion similar to renal cell carcinoma or another renal tumor. [13]