Case #1:
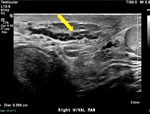
48-year-old male with history of human immunodeficiency virus infection currently undergoing therapy presented to our outpatient facility with chronic hematospermia. Scrotal ultrasound demonstrated normal bilateral testes and epididymi. Evaluation of the right inguinal canal demonstrated right varicocele with curvilinear tubular hypoechoic structure with internal low-level echoes (Fig. 1) and no internal flow on color doppler imaging (Fig. 2). A diagnosis of right spermatic vein thrombosis was made and patient was recommended to follow-up with his primary care physician. No intraabdominal pathology was seen on follow-up outpatient imaging.
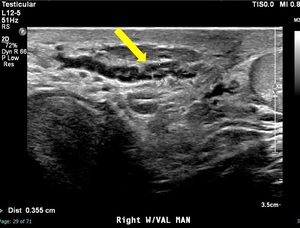
Fig. 1: There is a curvilinear hypoechoic tubular structure with internal low-level echoes in the right inguinal region on grayscale image. This image demonstrates a dilated vein with an intraluminal thrombus - 'Sonographic caterpillar sign' of the testicular ultrasound (yellow arrow).

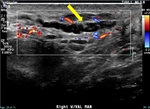
Fig. 2: Dilated right varicocele does not demonstrate flow on color doppler image (yellow arrow).
Case #2:
63-year-old male with no significant medical history presented with new onset left testicular pain. An emergent scrotal ultrasound done to rule out testicular torsion demonstrated normal bilateral testes and epididymi. Additionally, patient had left varicocele with a curvilinear hypoechoic tubular structure in the left inguinal canal with internal low-level echoes (Fig. 3) and no internal flow on color doppler imaging (Fig. 4). Patient was recommended to follow-up with his primary care physician, no additional imaging was obtained at our institution.

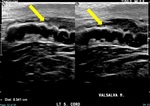
Fig. 3: There is a 3.4 mm curvilinear hypoechoic tubular structure in the left spermatic cord on grayscale image - 'Sonographic caterpillar sign' of the testicular ultrasound (yellow arrow).
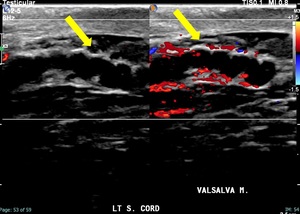
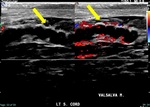
Fig. 4: Dilated left spermatic cord vein without internal flow on color doppler image consistent with thrombosis (yellow arrow).
Case #3:
59-year-old male with history of hypertension, hypercholesterolemia, and diabetes mellitus presented with new onset left testicular pain. An emergent scrotal ultrasound done to rule out testicular torsion demonstrated normal bilateral testes and epididymi. Ultrasound of the spermatic cord demonstrated a curvilinear hypoechoic tubular structure with internal low-level echoes (Fig. 5), no internal flow on color doppler and spectral display (Fig. 6 and 7). Patient was recommended to follow-up with his primary care physician. No additional imaging was obtained at our institution.

Fig. 5: There is a curvilinear hypoechoic tubular structure with internal low-level echoes in the left spermatic cord on grayscale image - 'Sonographic caterpillar sign' of the testicular ultrasound (yellow arrow).

Fig. 6: The left spermatic cord vein without internal flow on color doppler image (yellow arrow).

Fig. 7: The left spermatic vein does not demonstrate spectral flow (yellow arrow).
Pathology:
Spermatic vein or pampiniform plexus vein thrombosis, a less common cause of acute scrotal pain has rarely been encountered in daily practice with fewer than 25 reported cases in literature. There are many etiologies for venous thrombosis, including a combination of virchow’s triad: stasis of blood, increased coagulation factors, and mural factors. In addition, increased intraabdominal pressure can result in compression of the venous plexus in the inguinal canal against the ileopubic ramus.
In general, the left spermatic vein has a higher propensity to thrombose secondary to nutcracker syndrome, where the left renal vein is compressed between the aorta and the superior mesenteric artery resulting in back pressure into the left spermatic vein. This can lead to slow flow, and eventually thrombosis. However, isolated right renal vein thrombosis is extremely rare and can be seen secondary to intraabdominal malignancy that can cause external compression of the vein or inferior vena cava thrombosis.
We present an ideal sonographic sign that can be used for identifying a spermatic vein or pampiniform plexus vein thrombosis utilizing the hypoechoic “millipede sign” in the spermatic cord. This can allow prompt recognition and appropriate management of spermatic venous thrombosis.
Management:
Management of spermatic vein thrombosis is controversial and is primarily dependent on patient presentation and the underlying pathology. A left sided varicocele or vein thrombosis can be managed with regular outpatient follow-up. A right sided varicocele requires further work-up to exclude an occult intraabdominal tumor. Additionally, if the thrombus extends through the external inguinal ring into a deeper vessel or the renal vein, it could result in a pulmonary embolus and management with anticoagulation is recommended.