Keywords:
Performed at one institution, Observational, Retrospective, Multidisciplinary cancer care, Calcifications / Calculi, Vacuum assisted biopsy, Surgery, Biopsy, Ultrasound, Mammography, Management, Breast
Authors:
J. Chalfant1, B. Li2, T. Chan1; 1Los Angeles/US, 2Santa Monica/US
DOI:
10.26044/ecr2020/C-13887
Results
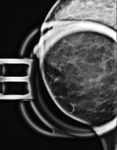
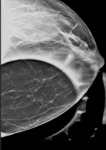
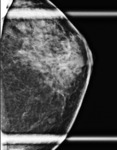
Of the 116 core needle biopsies demonstrating ADH that proceeded to surgical excision, 19 cases (16.4%) were upgraded to malignancy at time of surgical excision (4 invasive ductal carcinoma and 15 ductal carcinoma in situ). Of the upgraded cases at surgery, 57.9% presented with calcifications alone (Figure 1), 15.8% mass (Figure 2), 15.8% architectural distortion, 5.3% focal asymmetry with architectural distortion, and 5.3% architectural distortion with calcifications. Of the benign cases at surgery, 79.4% presented with calcifications alone (Figure 3), 8.2% mass, 5.2% architectural distortion, 3.1% focal asymmetry, 1.0% asymmetry, 1.0% focal asymmetry with architectural distortion, 1.0% architectural distortion with calcifications, and 1.0% mass with calcifications (Table 1).
Of those cases with calcifications alone, calcification distribution in upgraded cases was most frequently segmental (45.5%), whereas 92.2% of benign cases were grouped. This contributes to a significant difference in the span of calcifications for upgraded cases compared to benign cases (25.6 ± 26.8 mm upgraded cases versus 8.8 ± 9.2 mm benign cases, mean ± SD, p <0.0001). Calcification morphology in upgraded cases was coarse heterogeneous (54.5%) or amorphous (45.5%), similar to the most frequent morphologies in benign cases (Table 2).