Leukemia, lymphoma and myeloproliferative diseases are group of hematological malignancies that make patients susceptible to pulmonary complications (PC). PC of hematological malignancies and their treatments are common causes of morbidity and mortality. Abnormal vital signs (fever, hypoxemia) and respiratory symptoms such as dyspnea, cough, hemoptysis and chest pain bring patients to chest imaging. PC can be broadly categorized as:
A. Infectious (caused by bacteria, viruses, fungi and parasites)
B. Malignant (primary involvement, relapse/ recurrence)
C. Toxic (drug and radiation toxicity)
D. “Others” [1]
Pulmonary complications are radiologicaly manifested on computed tomography as consolidation, ground-glass attenuation, nodules, masses and interstitial infiltrate.
A. INFECTION:
Bacterial infection
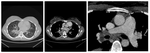
Many bacterial infections arise from the patient’s microbial flora, but are also contracted through exposure to sicking individuals or environmental sources. Agents are various: gram negative rods, gram positive cocci, Mycobacteria, … MDCT showes multifocal consolidations, nodules, and mass lesions (Fig. 1). [1]

Fig. 1: Patient with leukemia and TBC; CT scan of the lung shows consolidation surrounded by tree-in-bud pattern( left), necrosis in consolidation( middle), and lymphadenopathy (right)
Fungal infection
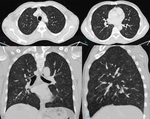
Aspergillosis is most common agent of fungal infection. MDCT shows multiple consolidation surrounded by ground glass opacities forming patognomonic “hallo„ sign, necrotic consolidations with characteristic „crescent sign“. other species that can cause infection are: Candida spp., Pneumocystis, ... (Fig. 2) (Fig. 3).

Fig. 2: Patient with leukemia and pneumocystis jiroveci pneumonia; CT scan of the lung shows diffuse ground-glass lesions in peribronchovascular distribution. (a.-d.)

Fig. 3: Patient with leukemia and pneumocystis jiroveci pneumonia; CT scan of the lung shows very discrete diffuse ground-glass lesions in peribronchovascular distribution.(a.-d.)
Viral infection
Cytomegalovirus infection is most common agent of viral pneumonia. MDCT findings are nespecific, and they include scattered and wide spread of ground glass opacities, consolidation, thickening of bronchovascular bundle and TIB pattern.
B. MALIGNANT (primary involvement, relapce∕recurrence ) (Fig. 4):

Fig. 4: Lung involvement in patients with hematological malignancies
Leukemia
Depending on type of abnormal cells and their maturity there are four major types of leukemia: acute myeloid leukemia, chronic myeloid leukemia, acute lymphoblastic leukemia and chronic lymphocytic leukemia. There are four types of lung involvement. Most common tipe of lung involvement is pulmonary infiltration, defined as extravascular collections of leukemic cells in the lung parenchyma without another apparent cause of their presence. It occurs most commonly in the terminal stage of the disease, but also at other time points including before treatment. CT findings are nonspecific. Leukemic cells have a tendency to involve the perilymphatic interstitium, producing smooth or nodular thickening of the bronchovasular bundles and interlobular septa. Nodules are also common and can be peribronchovascular, centrilobuar or random in distribution. Ground-glass and consolidative opacities are also common, the consolidation may predominate in peribroncial regions, reflecting inflitration of the parenchyma adjacent to the perilymphatic interstitium (Fig. 5). CT finding can be suggestive, but accurate diagnosis usually requires bronchoalveolar lavage or lung biopsy. [2]

Fig. 5: Patient with acute myeloid leukemia. CT scan of the lung shows thickening of septal interstitium (a.), diffuse nodular lesions in peribronchovasular distribution (b., c., f.), micronodular lessions in peribronchovasular distribution, forming "tree in bud" pattern (d.) and mediastinal lymphadneopathy (e.). All this findings suggest leukemic pulmonary infiltrarion.
Pulmonary lymphoma
Pulmonary limphoma is a malignant monoclonal lymphoid proliferation within the lung parenchyma. It can be MALT limphoma, other non- Hodgin lymphoma or Hodgin lymphoma. MALT lymphoma is by far the most common. In this patiens there is invasion of the bronchial epithelium by lymphoid cells, than there is limphangitic spread at the periphery of these lesion ( along pleura, interlobular septa, and bronchovascular bundles), and invasion into the adjacent pleura, vessels and airways can occur. Radiography shows nodules, masses and∕or consolidation. CT shows multiple nodules, masses, and∕or nodular∕mass like areas of ground glass attenuation or consolidation (or both), which tend to be in bronchovascular distribution, and often show air bronhograms, which can be dilated, hilar and mediastinal limphadenopathy, more rarely it manfiests as patchy large areas og gorund-glass. Acurate diagnosis also requires lung biopsy. [3]
Extramedullary myeloma
Extramedulary myeloma (EMM) is a relatively rare disease, the incidence increases over the duration of the disease. While pulmonary findings in Multiple myeloma are relatively common, the overwhelming majority of these are related to an infectious etiology, but it can also be related to interstitial pulmonary infiltration with neoplastic plasma cells. MDCT often shows bilateral patchy alveolar and interstitial opacities, affecting primarily the upper lobes. [4]
C. TOXIC :
Drug toxicity
Numerous agents have potential to cause pulmonary toxicity. The radiologic manifestations reflect the underlying histopatologic processes and include diffuse alveolar damage (DAD), nonspecific interstitial pneumonia (NSIP), bronciolitis obliterans organizing pneumonia (BOOP), obliterative pneumonitis, pulmonary hemorrhage, edema, hypertension or veno-occlusive disease. DAD is common manifestation, and CT shows scatterees or diffuse areas of ground-glass opacities. At NSIP later CT scans can show fibrosis in basal distribution, and in BOOP CT shows nodular consolidation, centrilobular nodules and bronchial dilatation. [5]
Radiation toxicity
Radiation-induced lung disease due to radiation therapy is common. Acute fase typically manifests as ground glass opacity or attenuation or as consolidation, in later fase, it typically manifests as traction bronchiectasis, volume loss and scarring.
D. "OTHERS" :
There are numerous of conditions that cause PC in patients with hematological malignancies. Some of them are congestive heart failure, transfusion associated circulatory overload, venous thromboemolism, pulmonary veno- occlusive disease, pulmonary hypertension, trombotic microangiopathy, hemophagocytic lymphohistiocytosis, pulmonary alveolar proteinosis, … [1]
Alveolar proteinosis
Is a rare condition characterized by the intra-alveolar deposition of periodic acis-Schiff- positive lipoproteinaceous material. CT shows ground-glass opacities that are associated with interlobular septal thickening, the appearance is known as the “crazy-paving” pattern. [2]
Radiographic findings are subtle and not seen on radiography often, due to special resolution limitations, but they are well depicted by CT. CT is used for initial diagnosis and during follow up of disease treatment. Pet scan can be also useful for the evaluation of pulmonary nodules. Differential diagnosis is challenging. Imaging findings are often overlapping, or are just ill defined, so we need additional information of patients risk factors, clinical presentation, non invasive testing (microbiological and serologic investigation of serum, sputum,...) and invasive testing such as fiberoptic bronchoscopy and biopsy. With all of this information we may narrow differential diagnosis and guide therapy which is very important. [1]