It is essential to know the ventricles basic anatomy to understand the different entities that can occur in the cerebral ventricles and understand the symptoms that cause these neoplasms.
The imaging findings of different intraventricular neoplasms types can be similar. Therefore, it is crucial to know not only the main CT or MRI imaging findings but also, location of these neoplasms and patient’s age and gender, to narrow the differential diagnosis.
Presenting symptoms depend on the location: the lesions that occur in the fourth ventricle typically manifest symptoms of increased intracranial pressure (ataxia or paresis), and the supratentorial lesions manifest as headache, focal neurologic deficit or seizure.
We review the basic anatomy of the ventricles and provide the main imaging features of the most common intraventricular tumors.
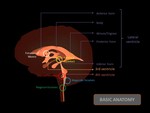
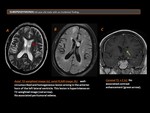
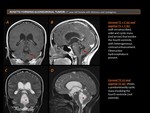
Basic anatomy (Figure 1)
The ventricular system is a set of communicating cavities within the brain, and it is responsible for the production, transport, and removal of cerebrospinal fluid (CSF).
The ventricular system is composed of:
- Lateral ventricles: are located in the right and the left cerebral hemispheres, and it has different parts: the anterior horn (in the frontal lobe), the posterior horn (in the occipital lobe), the inferior horn (in the temporal lobe), the body and the atrium. The lateral ventricles are divided into each other by the septum pellucidum, situated in the midline.
- Third ventricle: is located between the thalamus, and it is connected with the lateral ventricle by the foramen of Monro, and with the fourth ventricle by the cerebral aqueduct.
- Fourth ventricle: is located within the brainstem and the CSF drain from this structure to the central canal, trough the magnum foramen, and to the subarachnoid space through the foramen of Magendie (central and posterior aperture) and trough the foramina of Luschka (anterior laterals apertures).
The ventricles are surrounded by two layers:
- Ependymal cells layer: where the ependymoma originates.
- Subependymal layer: composed of glial cells. It gives rise to tumors like subependymoma and subependymal giant cell tumors (SGCT).
The septum pellucidum is also lined by glial cells and residual neuronal precursor cells, and it gives rise to the central neurocytoma.
The choroid plexus is responsible for producing CSF, and it is distributed throughout the ventricular system, predominantly in the atria (where the choroid plexus neoplasms are most frequently located).
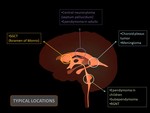
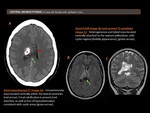
Intraventricular tumors (Figure 2), (Figure 3)
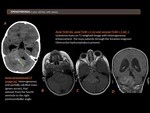
Ependymomas are common neoplasms. They constitute 3-5% of intracranial neoplasms and are the third most common brain neoplasm in children (behind medulloblastoma and astrocytic tumors).
These tumors may manifest at any age group but are more common in younger patients and there is no gender predilection. Those that occur in the posterior fossa (60% of cases) are more common in children (6 years), whereas supratentorial lesions (40% of cases) are more common in young adults (18-24 years).
Ependymomas involving the fourth ventricle tend to fill the ventricle and may extend through the foramen of Luschka, the foramen of Magendie, or the magnum foramen. This finding is highly suggestive but is not pathognomonic of an ependymoma.
NECT (nonenhanced computed tomographic): hypo or isoattenuating, partially calcified mass, and occasionally intratumoral hemorrhage may be seen.
MRI: iso to hypointense on T1-weighted images (T1WI) and iso to hyperintense on T2-weighted images (T2WI).
Enhancement: Heterogeneous.
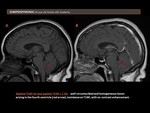
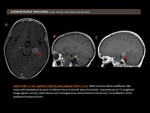
- Subependymoma (Figure 5), (Figure 6)
Subependymomas account for 0,2 % - 0,7% of intracranial neoplasms; however, this may be an underestimate, because these neoplasms are often asymptomatic and found incidentally. These neoplasms are more common in patients older than 15 years, and males are more commonly affected.
The most frequent location of these lesions is the fourth ventricle (50%), followed by the lateral ventricle.
NECT: well-circumscribed, usually small (<2 cm), lobulated intraventricular mass that is predominantly hypo- to isoattenuateding. Hydrocephalus is present in 85% of cases. Calcification and cystic degeneration are common.
MRI: hypointense on T1WI and hyperintense on T2WI.
Enhancement: is variable, but most lesions demonstrating no or minimal enhancement.
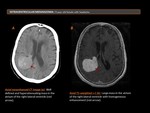
- Central neurocytoma (Figure 7)
Central neurocytoma constitute approximately 0,25%-0,5% of intracranial tumors. The location most common is in the lateral ventricle (usually near the foramen of Monro), and arise from the septum pellucidum or ventricular wall. The mean patient age is 29 years, and there is no gender preference.
NECT: well-circumscribed, heavily lobulated intraventricular masses that frequently have numerous cystlike areas and attached to the septum pellucidum. Calcification is frequent (50%-70% of cases). These lesions are hyperattenuated compared with brain parenchyma. Hydrocephalus is common.
MRI: isointense to gray matter on T1WI and hyperintense on T2WI. These lesions may have a “bubbly” appearance due to the presence of multiple cysts.
Enhancement: is variable, but substantial enhancement is typically seen.
- Subependymal giant cell tumor (SGCT).
SGCT is the most common cerebral neoplasm in patients with tuberous sclerosis, developing in up to 15% of cases. Still, the SGCT is an uncommon tumor. Most cases occur in the 1st and 2nd decades.
The most typical location of these lesions is near the foramen of Monro, and it has been proposed that they arise from a subependymal nodule. SGCT is characterized by slow growth and benign behavior.
NECT: hypo to isoattenuated intraventricular mass near the foramen of Monro. Well-circumscribed and typically larger than 1 cm. Other subependymal nodules may be seen. Calcification is common.
MRI: hypo to isointense to gray matter on T1WI and iso to hyperintense on T2WI.
Enhancement: intense homogeneous enhancement. This enhancement distinguishes an SGCT from a subependymal nodule, which does not enhance.
- Choroid plexus neoplasms: papilloma (CPP) and carcinoma (CPC) (Figure 8)
Choroid plexus neoplasms account for 2%-4% of pediatric brain tumors and 0,5% of adult brain tumors. These tumors arise from the choroid plexus epithelium. Therefore, the most frequent location is in the atrium of the lateral ventricle (50%), which is the location where there is more of this tissue.
Lateral ventricle lesions are common in children (80% of cases) and without gender predilection. Fourth ventricle lesions are distributed among all age groups and are more common in males.
NECT: well-circumscribed cauliflower-like masses with prominent lobulations. Hemorrhage and cyst formation may be seen. Iso to hyperattenuated CPC may present more frequent necrosis and parenchymal invasion. Hydrocephalus is recurring, and its etiology may be due to overproduction or due to a mass effect. CPC tends to be more heterogeneous than CPP.
MRI: iso to hypointense on T1WI and iso to hyperintense on T2WI.
Enhancement: the lesion demonstrates intense enhancement.
- Intraventricular meningioma (Figure 9)
Intraventricular meningiomas account for 1%-2% of intracranial meningiomas. The most common location for these lesions is in the atrium of the lateral ventricles (left more frequent than right atrium). Less commonly, they may arise within the third ventricle. They are most common in females with a peak age range of 30-60 years.
Meningiomas usually have an indolent biologic behavior, but those that affect pediatric age have an increased predilection for sarcomatous changes.
NECT: well-defined hyperattenuating globular mass. Local or diffuse ventricular dilatation is present. Calcification is common (50% of cases), and periventricular edema may also be seen. Cystic areas are common in the pediatric population.
MRI: iso to hypointense on T1WI and iso to hyperintense on T2WI.
Enhancement: Avid enhancement is seen due to the highly vascular nature of these lesions.
- Rosette-forming glioneuronal tumor (RGNT) (Figure 10)
RGNT is a sporadic tumor and typically occurs in young adults. It is a mass located in the fourth ventricle. These lesions usually have indolent biologic behavior.
NECT: well-defined, heterogeneous solid, and cystic mass centered on the fourth ventricle. Intratumoral calcification and hemorrhage may occur. Hydrocephalus may be present.
Enhancement: heterogeneous enhancement is seen.