Pneumoretroperitoneum
- Pathological accumulation of gas/ air in retroperitoneal spaces
- Emergency condition that requires an early diagnosis to ensure optimal management
- Imaging plays important role in early diagnosis as clinical symptoms are often vague and local examination is not easily accessible by clinicians
- Correct identification of its etiology is challenging both because pneumoretroperitoneum is not specific and because its differential diagnosis is broad
A summary of pathologies associated with pneumoretroperitoneum (Table 1 and 2)
TABLE 1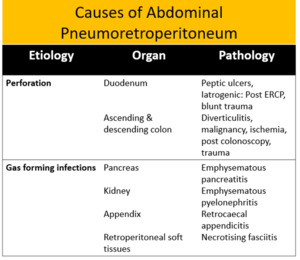
Fig. 22
TABLE 2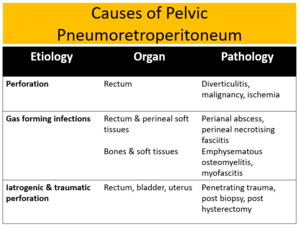
Fig. 23
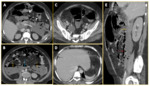
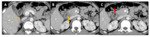
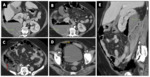
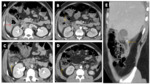
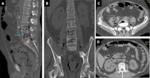
Emphysematous pancreatitis Fig. 4
• Severe complication of acute necrotising pancreatitis
• Etiology:
◊Polymicrobial infection with gas forming organisms
◊ Enteropancreatic fistula
• CT findings : Fig. 4
ο Gas within necrotic pancreatic parenchyma
ο Air containg collections in retroperitoneum
• Management : antibiotic coverage, percutaneous drainage or surgical resection with fistula closure
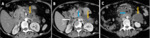
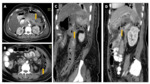
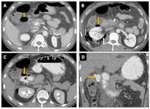
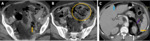
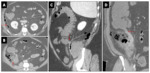
Acute necrotising pancreatitis with entero-pancreatic fistulas
Fig. 5,Fig. 6
• Inflammation & enzymatic destruction spread through connected anatomic compartments to involve the adjacent organs i.e. duodenum
and colon
• Complications range from localised ileus to severe gut ischemia & necrosis with fistula formation
• Colopancreatic fistulas occur in 3-10% of patients with acute necrotizing pancreatitis with splenic flexure being the most common site
• CT findings : Fig. 5,Fig. 6
o Direct signs:
- Visualisation of bowel wall discontinuity
- Extraluminal contrast extravasation
o Indirect signs:
- Free air in peritoneal or retroperitoneal spaces
- Localised air containing collections
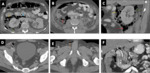
ERCP induced duodenal perforation: Table 3 and Fig. 7
• Retroperitoneal perforation is an uncommon complication of ERCP (0.5-2%)
• Occurs due to tear of the bile duct or the periampullary region
• Leads to diffusion of large amounts of air, which does not correlate with the severity of perforation
TABLE 3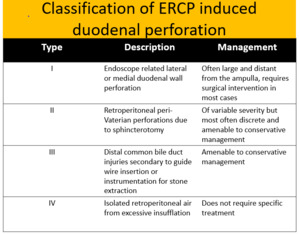
Fig. 24
References: Tonolini M et al. (2015) Cross- sectional imaging of common and unusual complications after endoscopic retrograde cholangiopancreatography. Insights Imaging 6:323-38
Perforated duodenal ulcer Fig. 8
•Usually affects the duodenal bulb
•Perforation of ulcer in second part of duodenum causes pneumoretroperitoneum
Post traumatic duodenal perforation: Fig. 9
• Most common site is D2 and D3 part as these are fixed structures and due to posterior presence of vertebral column
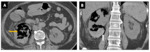
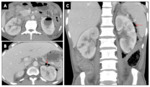
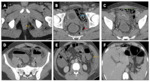
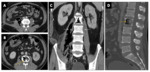
Emphysematous pyelonephritis Fig. 10 and Fig. 11
• Risk factors:
- Uncontrolled diabetes mellitus
- Immunocompromised status
- Urolithiasis
- Neoplasms
- Papillary necrosis
• CT findings : are of two types: Fig. 10 and Fig. 11
ο Type 1
- Greater than one-third renal parenchymal destruction
- Streaky or mottled appearance of gas
- Intra-renal or extra-renal fluid collections are characteristically absent
ο Type 2
- Destruction of less than one-third of the parenchyma
- Renal or extrarenal collections associated with bubbly or loculated gas, or gas within pelvi-calyceal system or ureter
• Management: IV antibiotics, percutaneous catheter drainage of collections or nephrectomy
Ruptured renal abscess: Fig. 12
Retroperitoneal necrotizing fascitis Fig. 13
• Infection of soft tissues characterised by progressive necrosis of muscle fascia and adjacent soft tissue
• Risk factors: diabetes, immunosuppression, vascular disease
• Etiology:
◊ Perianal abscess
◊ Perforated diverticulitis
◊ Gangrenous appendicitis
◊ Emphysematous pyelonephritis
• CT findings: Fig. 13
ο Free gas between fasciae and in the abdominal wall
ο Asymmetrical fascial thickening with enhancement
ο Fluid collections and fat stranding
• Management: antibiotics and surgical debridement
Perforated colon cancer Fig. 14
• Incidence: 2.5 – 10% of patients with colon cancer
• Etiology:
◊ Tumor necrosis
◊ Increased pressure in the colon proximal to obstruction
• Common sites: sigmoid colon & cecum.
• CT findings :Fig. 14
ο Focal defect in colon wall with fluid density abscess
ο Free intraperitoneal &/or extraperitoneal air
Diverticulitis with perforation Fig. 15
• Most common site: left colon
• CT findings: Fig. 15
o Contained perforation :
- Local abscess
- Fistula formation
o Non contained perforation:
- Intraperitoneal free air
- Retroperitoneal free air ( second & third parts of duodenum, posterior aspect of ascending, descending & sigmoid colon)
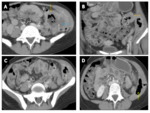
Retrocaecal appendicitis Fig. 16, Fig. 17
• Incidence of retrocaecal appendix : 26-65%
• Atypical clinical presentation
• CT findings: Fig. 16, Fig. 17
ο Inflammatory stranding with air containing fluid collections in retroperitoneal and extraperitoneal spaces upto the bare area of liver
ο May spread along right paracolic gutter to right posterior subhepatic & right subphrenic spaces
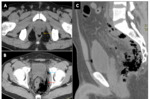
Perianal fistula with abscess Fig. 18, Fig. 19
• Ischiorectal abscesses usually present acutely & require emergency incision & drainage
• Imaging required when abscesses are associated with unusual symptoms like abdominal pain especially in immunocompromised & elderly patients.
• CT findings: Fig. 18, Fig. 19
ο Air & fluid containing collections in the perianal space with extension into pelvic retroperitoneal and extraperitoneal spaces
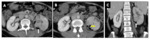
Emphysematous osteomyelitis of spine Fig. 20, Fig. 21
• Etiology:
◊ Hematogenous spread in monomicrobial infections
◊ Contiguous spread in polymicrobial infections
• Risk factor: diabetes mellitus
• Causative organisms: anaerobe
• Blood cultures: positive only in one-third of patients with spinal infections
• CT findings: Fig. 20, Fig. 21
ο Intraosseous gas
ο Air containing paraspinal or intramuscular collection
• Management: antibiotics & surgical drainage