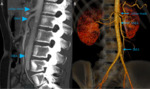
Intestinal ischemia is a general term for an inadequate blood flow to the gas-filled abdominal viscera. The condition can be subclassified depending on the duration of symptoms, etiology, or the part of the bowel involved (Fig. 2.).
Acute mesenteric ischemia (AMI) is an uncommon but life-threatening condition, accounting for approximately 0.1% - 0.01% of all hospital admissions (Fig. 3.).
Despite progress in diagnostic and treatment options, the mortality rate has not changed significantly during the past decade and remains high at 50% to 70% [3].
Vascular anatomy and pathophysiology.
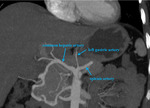
There are three major arteries (Tab. 1.; Fig. 4-5) that supply the small and large bowel.
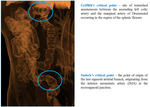
Arterial branches further divide and form anastomotic arcades (Fig. 6.) of smaller arteries along the mesenteric border. These arcades give rise to vasa recta that supply the small bowel wall. The proximal vascular territory of the IMA overlaps the distal SMA territory, creating a watershed zone of perfusion susceptible to ischemia (Fig. 7.).
There are numerous mesenteric collateral pathways allowing for a rich blood supply to the bowel:
- the gastrodudoenal artery provides a collateral pathway between the celiac artery and the SMA,
- the marginal artery of Drummond and arc of Riolan (Fig. 8.) connect the SMA and IMA,
- four anastomotic arcades are formed between the IMA and lumbar arteries arising from the aorta, sacral, and internal iliac arteries.
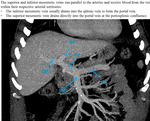
AMI is caused not only by an inadequate mesenteric arterial blood flow but also by the obstruction of mesenteric veins (Fig. 9.) or intestinal hypoperfusion in the absence of vascular occlusion.
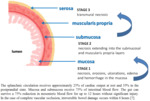
Ischemic injury starts at the mucosa and extends towards to the serosa. Based on the extent of bowel wall involvement, three stages of AMI are recognized [8] (Fig. 10.).
Etiology and clinical manifestation.
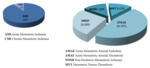
Mesenteric ischaemia can be of acute (90%) or chronic type (10%) [1]. Acute mesenteric ischemia can be categorized into four different etiological subtypes (Fig. 2). The most common cause of AMI, responsible for 40–50% of cases (Fig. 11.), is mesenteric arterial embolism (MAE) [10].
Clinical manifestation of mesenteric ischemia can be acute or chronic (Fig. 12.). The key to early and accurate diagnosis AMI is a high level of clinical suspicion. Diagnosis is challenging due to non-specific clinical manifestations (Fig. 13.) and the rarity of disease. There is no specific laboratory test (Fig. 14.) that can be routinely used for early detection of AMI. Even when mesenteric infarction is suspected, diagnosis takes 7.9 hours on average, while a warm ischemia time of 6 hours leads to the destruction of the mucosal barrier and causes irreversible damage [3].
Acute mesenteric ischemia should be suspected in patients with acute abdominal pain, especially when the pain is disproportionate to physical examination findings and in the elderly with a history of cardiovascular diseases.
The four etiological subtypes of AMI are associated with different patient characteristics and risk factors (Tab. 2.).