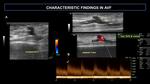
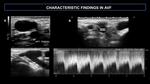
After the creation of an AVF, complications might occur, such as:
-Failing to mature: After the vascular access is created it needs to mature. Four months is the maximum interval for AVF mature. Many fistulas do not mature appropriately for being used in dialysis and may need correction or another intervention.
The objective quantitative criteria to assess the maturation of fistulas are:
-Thrombosis: can be characterized by an enlarged, non-compressible vein with intraluminal organized echogenic material, with partial or absent flow, depending on whether there is or is not recanalization. Dynamic compression maneuvers are very useful in the evaluation of veins with low speed flow.
-Thrombophlebitis: The superficial veins thrombosis can be characterized by the presence of intraluminal organized echogenic material, with partial or absent flow, depending on the presence of recanalization. Dynamic compression maneuvers are very useful in the veins evaluating due to its low speed flow. They are also frequent parietal thickening and caliber reduction, suggesting a sequel to previous thrombophlebitis.
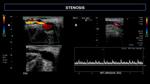
-Arterial Stenosis: In the normal population, upper limbs arterial stenosis is not as frequent as lower limbs arterial stenosis. However, chronic renal patients exhibit upper limbs arterial stenosis more often than the normal population, especially after the confeccion of an arteriovenous fistula. We used as a criteria for stenosis the luminal narrowing at B-mode and Color Doppler mapping, the presence of "Aliasing" at the point of stenosis and an increase of systolic velocity, reaching or exceeding the ratio of 2:1 in relation to the prestenotic bed.
-Stenosis in the efferent vein: may result from manipulation (repeated punctures in the same place), partial intraluminal thrombus or narrowing areas in valve sinus. We use as a criteria for stenosis the luminal narrowing at B-mode and Color Doppler mapping, the presence of "Aliasing" at the point of stenosis and an increase of systolic velocity, reaching or exceeding a ratio of 2:1 in relation to the prestenotic bed.
-Stenosis at the anastomosis: We used as criteria for arteriovenous anastomosis stenosis, besides the luminal narrowing in B-mode, the increase of systolic velocity, reaching or exceeding the ratio of 3:1 in relation to the pre anastomotic arterial bed.
-Arterial occlusions: will be characterized by the absence of flow, both in Color and Pulsed Doppler mapping. It is important to set correctly the parameters of the ultrasound (PRF, wall filter, gain and frequency) in order to avoid false positives diagnosis.
-Collections: Most AVF infections involve perivascular cellulitis, which manifests as localized erythema and edema and is usually easily treated. Much more serious is an infection associated with anatomical abnormalities, such as aneurysms, hematomas or abscesses, which require surgical excision and drainage.
Are particularly feared the infected collections related to the synthetic prostheses, which often evolve with necessity of its withdrawal.
They are characterized by the presence of anechogenic or hypoechogenic content, in some are organized. Correlation with clinical data should be performed.
-Aneurysms: Vascular dilations can occur in both afferent arteries as in efferent veins. It’s usually previously displayed at clinical examination. Ultrasound examination is easy, being related to dilated vascular structure, with or without mural thrombi. It is important to determine if there is any associated venous or arterial obstructive process.
-Steal syndrome: Arteriovenous fistula is a shunt between a high pressure system (arterial) and a low pressure system (venous). Usually the radiocephalic AVF causes no repercussion to the arterial segment distal to the AVF and the ulnar artery. Steal syndrome occurs when the radial artery segment distal to AVF anastomosis, features inversion of its flow. This means the AVF is stealing blood from the hand/palmar arch. It is characterized by marked reduction or reversal of flow through the arterial segment distal to the AVF in both Color and Pulsed mapping. We can also identify a biphasic flow in the ulnar artery (instead of a normal triphasic flow).
-
If the palmar arch is incomplete patient might present ischemic symptoms in the hand.
-
If the palmar arch is complete, the patient might present no ischemic symptoms, since the ulnar artery can supply adequate blood to the hand.
-
We can analyse the patency of palmar arch by performing Allen test.
-Synthetic prostheses (PTFE): It is important to recognize possible collections, obstructions and synthetic graft stenosis. We use as standard the following parameters:
- Flow below 1,300 ml/min.
- Stenosis > 50% at B-mode
- Systolic peak speed > 400 cm/s