ANAMNESTIC AND CLINICAL EVALUATION
Knowledge of needles' shape, dimension and material, as well as reconstruction of clinical history, is important to set the most appropriate diagnostic workup.
According to the mechanism of retention three possible patterns are distinguishable: ingestion, iatrogenic retention and penetration [1].
Ingestion
Ingestion is a rare event, more common in children than in adults. A special attention is required for particular categories: patients with behavioral or mental disorders, or healthy adults and children with predisposing factors or injurious situational problems (drugs abuse, criminal activities, child or spousal abuse) [1,2].
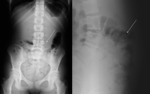
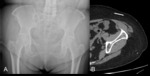
Sewing needles representing 2.4% of all ingested foreign bodies [3]. Once ingested, needles may wedge at areas of narrowing or anatomical acute angulation (duodenal loop, Treitz angle, appendix and ileocecal valve) [2,4] (Figure 1).
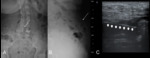
In 64% of cases symptoms occur after 48 hours; epigastric pain is the most common one [4]. Complications such as ulcers, lacerations, erosions, and perforation are not rare [5]. Needle migration through the intestinal walls is infrequent (1% of all ingestions) [2,3] but when occurs, multiple anatomical structures can be involved [3] (Figure 2).
Iatrogenic retention
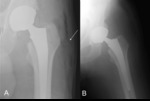
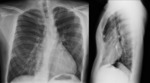
Necessity for needles intraoperative counting is sometime an unavoidable occurrence in the operating room [6] (Figure 3). Several iatrogenic retention risk factors have been reported (Table 1) [7,8]. As the consequence of poor literature evidence, it is reasonable to consider underestimated the real incidence of iatrogenic retention that probably ranges from 1/1.000 to 1/1.500 procedures [6]. In addiction, sometimes missing needles remain asymptomatic in the post-operative period and could be an incidental finding years later (Figure 4).
More often, the needle become painful and may be confused with normal post-operative pain, with delayed diagnosis (Figure 5). Intravenous migration of a fragmented needle is a rare but described occurrence [9–11]; once in the systemic circulation, the needle could potentially migrate through the veins to the heart and pulmonary circulation, with high risk of injuring right cardiac chambers or lungs. Intravenous drug abuse with multi-used needles or subcutaneous injection of drugs with very tiny needles (i.e. insulin) (Figure 6, 7) are usually the underlying cause of needle rupture and migration but other events such as iatrogenic surgical needle embolism may occur (Figure 8).
Penetration
Penetration is a well known uncommon mechanism that can lead to a retained needle [1]. Most cases are accidental, often described in a working setting, such as tailoring workers (Figure 9). Less frequently needle penetration could be a voluntary gesture [2] (Figure 10).
Needles, and their fragments, usually lie in the soft tissues and are easily identified because partially surfacing or due to the formation of foreign body granulomas.
Deep penetration in the abdomen or thorax is not described in the literature but is a potentially possible event. If a perforation occur, they may lodge in the retroperitoneal tissues, induce localized contained abscesses, lie free within the peritoneum, or even travel to distant sites in the body (Figure 10).
RADIOLOGICAL TECHNIQUE
X-Ray
X-ray is usually the first radiological test performed and often allows the identification of the needle and visible complications such as pneumothorax or free gas in abdomen [12]. X-ray advantages consist on its availability (also intra-operative), relatively low radiation dose and panoramic visualization of the district of interest. Double-projection should always be performed because anatomical structures, such as bones and soft tissues (Figure 6), and/or other radiopaque devices (Figure 3) could prevent needle visualization in a single-projection. Double-projection also allows the correct anatomical location of the needle (Figure 6, 7). When feasible, X-rays should be performed with a static machine in a radiological room because of the higher quality of the images provided in comparison with a mobile machine. If the scan is performed in the operative room, some authors suggest that a C-arm is more useful than a mobile machine for detecting needles [13]. Limitations associated with intraoperative radiographs are show in table 2 [7].
Needles could have different shapes and dimensions; on this basis, a X-ray scan performed with standard “diagnostic” voltage and milliamperage parameters could fail the needles identification, in particular smaller ones, due to their poor conspicuity. For this reason, a more penetrating scan could be performed. Surgical needles smaller than 5-0 are faintly visualized on X-ray [14,15] and it was demonstrate that the detection sensitivity rate of imaging studies inside the operative room is strongly correlated with the size of the needle with 29% of sensibility with needles from 4 to 10 mm in size [16].
Computed Tomography (CT)
CT is considered a second level examination and plays an important role due to its higher sensitivity and specificity for both identification (Figure 5) and proper localization (Figure 8, 11) when compared to X-ray [17]. CT is usually performed to confirm the retained needle suspect after X-ray examination, if diagnosis is not clearly assured, and to provide more elements about possible complications and treatment planning [3,17]. Use of contrast medium is not usually necessary for needle identification but a post-contrast examination may be useful to define the needle relationships with surrounding structures and to better characterize possible complications (Figure 10) [3,17].
Ultrasonography (US)
US has a marginal role in the evaluation of patients with retained needles.
A possible application could be the needle search in the superficial soft tissue [18]. In our experience (Figure 2), US identification of a needle into the gastric wall was made possible by the lack of depth from the skin plane. It is our opinion to use US in pediatric subjects in order to reduce exposure to ionizing radiation.
MANAGEMENT
Some protocols based on multistep approach have been proposed for needles lost during surgical procedures [7,12], but there is no evidence in literature about radiological management for ingested and penetrated needles. In figure 12, 13, and 14 a possible workup is proposed according to the time of onset of the suspicion and the possible localization of the needle for each epidemiology.