Imaging is pivotal for detection and preoperative planning of PMP.
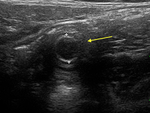
Ultrasound is valuable for the evaluation of the appendicular region: an abnormal fluid distension of the vermiform appendix lumen is suspicious for mucocele (Fig.3).
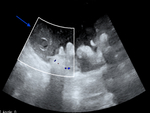
Ascites containing septa, motionless punctuate echoes and floccules into mucinous ascites, honeycomb like lesions, visceral organs surface notches (scalloping) are also recognizable at US examination (Fig.4) [10-11].
CT and MRI represent not only sensitive mapping techniques for proper presurgical planning but also for the staging PMP.
Both imaging modalities allow to detect the typical imaging features of the disease: ascites, peritoneal thickness and implants, “omental cake” and upper abdominal organ “scalloping” (Fig.5) [12].
Due to the presence of fibrotic components, the delayed phase (5-10 minutes after intravenous contrast medium injection) is the best time point on CT for better defining solid peritoneal implants and omental cake (Fig.6).
CT easily demonstrates calcifications that can occur in the peritoneal deposits (Fig.7).
T2w and DWI (Diffusion-Weighted Imaging) sequences on MRI can better demonstrate respectively the distribution of mucinous material in the peritoneal cavity, especially when only a small amount is present (Fig.8), and peritoneal metastases difficult to detect at CT such as mesenteric implants (Fig.9) [13].
Moreover, CT and MRI allow for an accurate preoperative assessment of disease burden in order to avoid nontherapeutic laparotomies using scoring systems such as Peritoneal Cancer Index (PCI; Fig.10) [14].
Although a PCI >20 has been correlated to shorter overall survival in multicentric studies, the definitive cut-off for non-therapeutic surgery is yet not defined [15].
Mesenteric mass> 5 cm, diffuse mesenteric tumor infiltration, mesenteric vascular encasement, diffuse small bowel serosal tumor and hepatoduodenal ligament involvement (Fig.11) are considered negative prognostic factors [13].
A complete removal of PMP is considered achieved when is possible to preserve at least the upper part of the stomach, clear the hepatic pedicle and maintain a sufficient length of small bowel in order to avoid short-bowel syndrome. In a recent study a PCI cut-off of 28 was adequate to define extensive PMP difficult to resect in totality [15].






![Fig. 10: Peritoneal Cancer Index (PCI) [14]. References: Sugarbaker PH. Surgical responsibilities in the management of peritoneal carcinomatosis. J Surg Oncol. 2010 Jun 15;101(8):713-24.](https://epos.myesr.org/posterimage/esr/ecr2020/156196/media/873398?maxheight=150&maxwidth=150)

