Type:
Educational Exhibit
Keywords:
Oncologic Imaging, Abdomen, Gastrointestinal tract, Peritoneum, CT, MR, Ultrasound, Diagnostic procedure, Metastases, Not applicable
Authors:
C. Sofia, M. A. Marino, A. Cattafi, A. Macri', G. Ascenti, A. Blandino; Messina/IT
DOI:
10.26044/ecr2020/C-15263
Background
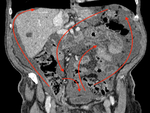
Pseudomyxoma peritonei (PMP) is a progressive disease characterized by gelatinous peritoneal deposits (the so called “Jelly Belly”).
The estimated incidence of PMP is of 1-3 out a million per year and it is usually incidentally discovered in people with ages between 40-55 undergoing imaging for other reasons [1].
It is considered to originate from a mucinous appendicular neoplasia. The key event is the perforation or rupture of the neoplastic appendicular mucocele into the peritoneal cavity [2].
The mucinous material spreads following the peritoneal fluid flow (Fig.1).
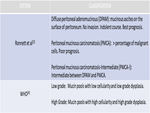
Two different classifications of PMP have been proposed (Table 1) [1,3-4].
PMP has an indolent progression and it is usually discovered at an advanced stage.
Symptoms and Signs are unspecific (Fig.2) [1].
Tumor markers as carcinoembryonic antigens (CEA) and carbohydrate antigen (CA 19.9) are considered diagnostic and prognostic tools also for postoperative follow-up [2].
Cytoreductive surgery (CRS) with hyper-thermic intraperitoneal chemotherapy (HIPEC) are the current adopted treatments [5].
Five years overall survival is 82-83 % for low grade tumors and 68 % for high grade ones [6-7].
Recurrence after surgery is high, up to 28 %, but a second cyto-reductive surgery is feasible, with a five-year overall survival of 79 % [8-9].