Primary Peritoneal Tumors.
They are defined as tumors whose primary manifestation is peritoneal, in the absence of a visceral origin. They arise from the mesothelial cells and the structures of the subperitoneum tissue.
1.- Mesothelial tumors.
Peritoneal malignant mesothelioma.
It is a rare tumor (1-2 cases per million), very aggressive, derived from the peritoneal mesothelium. 20-30% of mesotheliomas affect only the peritoneum (without thoracic involvement).
They usually occur in men 50 - 70 years. There is an association with asbestos exposure.
Correlation between the clinic and the CT findings has been described:
- Dry-painful type: abdominal pain; peritoneal mass and poor ascites.
- Wet type: abdominal distension and discomfort; ascites and generalized nodules.
- Mixed type: pain and ascites.
Radiological findings.
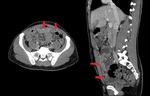
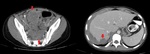
- Nodular thickening that gives rise to plaques (Fig.1). They can have mass effect ("scaloping") and enhance after administration of contrast.
- Invasion of adjacent abdominal organs (colon, liver).
- Uncommon: calcifications, distant metastases, adenopathies, abundant ascites.
Multicystic Peritoneal Mesothelioma.
Rare mesothelial neoplasm, with benign behavior and recurrence tendency (25-50%). It is not related with asbestos exposure.
More frequent in young or middle-aged women (with a history of surgery, endometriosis, pelvic inflammatory disease). It presents as pelvic pain.
Radiological Findings:
- Multilocular cystic mass, multiple unilocular cysts (“grape cluster”) or unilocular cyst, with a thin wall and septa. They generally depend on the pelvic peritoneum.
- It can wrap the ovaries and have polypoid excrescences, or incomplete partitions (DDx: cystic neoplasms of the ovary).
- It usually has no mass effect or calcifications.
The main differential diagnosis (DDx) is cystic lymphangioma (younger patients, without regional or sex predilection).
2.- Epithelial tumors.
Primary peritoneal papillary serous carcinoma (PPPSC).
Rare malignant neoplasm, histologically identical to the tubal and ovarian neoplasia of the same name. It is currently known that PPPSC is more common than previously thought: 15% of "epithelial ovarian carcinomas" are actually PPPSC.
It almost always occurs in postmenopausal women, presenting with abdominal distension and ascites.
Radiological findings.
- Ascites. It can be scarce.
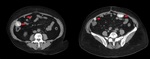
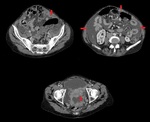
- Peritoneal thickening, nodules / masses in the omentum, with psammomatous calcifications (30%) (Fig.2).
- No ovarian mass. To differentiate PPPSC from ovarian carcinomatosis, pathological anatomy is often necessary.
3.- Mesenchymal tumors.
These are tumors derived from lymphatic, vascular, neuromuscular or fatty tissue. They are less common than retroperitoneals.
Some data can help us to guide the diagnosis: if greater size, heterogeneity and signs of vascular or visceral infiltration, greater probability of malignancy.
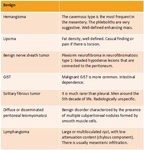
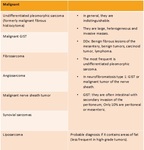
See Table 1 and Table 2.
4.- Other.
Desmoplastic small round cell tumors (DSRCT).
It is a rare neoplasm of histogenesis not well known, which belongs to the family of primitive pediatric tumors.
It is an aggressive tumor with a poor prognosis that occurs predominantly in adolescent boys and young adults (15-25 yo) as a palpable abdominal mass, bloating and abdominal pain.
Radiological findings.
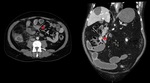
- Rounded soft tissue mass (single or multiple) in omentum, paravesical spaces and rectovesical/rectouterine space, without dependence on intra-abdominal organ (Fig.3).
- Heterogeneous enhancement (necrosis / hemorrhage). There may be calcifications.
- Variable ascites.
- On MRI, the tumors typically have heterogeneous signal intensity, predominantly T1 hypointense and T2 hyperintense.
- Lymphadenopathy, bone, lung and liver metastases at diagnosis (50% cases).
DDx: Sarcomas, neuroblastoma, rhabdomyosarcoma, primitive neuroectodermal tumor, lymphoma, desmoid tumor.
Secondary Peritoneal Tumors.
Metastatic disease, mainly secondary to carcinomas of the gastrointestinal tract and the ovary, is the most common malignant process in the peritoneal cavity.
Peritoneal carcinomatosis (PC).
Many neoplasms can metastasize to the peritoneum, in order of frequency: ovary, colon, stomach, pancreas, uterus, bladder, gallbladder.
In most patients the diagnosis of metastatic disease is obvious because there is evidence of a neoplasm in another location. However, sometimes it may be necessary to distinguish metastatic disease from primary peritoneal tumors --> Percutaneous biopsy.
Radiological findings.
- Ascites: free, or loculated.
- Nodules of soft tissue density in peritoneum and omentum, multifocal, which can form conglomerates or masses (Fig.4). They enhance after contrast and can invade mesentery, viscera or abdominal wall.
- Sometimes they show calcifications (papillary serous carcinoma of the ovary and mucinous carcinomas).
DDx: Malignant peritoneal mesothelioma, sarcomatosis, lymphomatosis and tuberculous peritonitis.
Peritoneal lymphomatosis.
It is the lymphomatous involvement of the peritoneum and subperitoneum (rare). It usually occurs in high-grade lymphomas or in advanced stages, and in immunocompromised patients.
Radiological findings.
- Superimposable to PC.
- Retrocrural and mesenteric adenopathies are more suggestive of lymphomatosis than of carcinomatosis.
Pseudomyxoma peritonei.
Intraperitoneal accumulation of mucinous ascites, due to the rupture of mucin-producing neoplasms (usually appendiceal).
- Benign variant: mucinous adenoma or appendiceal mucinous neoplasms of low grade.
- Malignant variant: Mucinous adenocarcinoma (appendix, colon, ovary,...)
Radiological findings.
- Low-attenuated loculated ascites, with septa that enhance slightly (edges of the mucinous nodules, or the displaced mesentery and omentum). Produces compression and scalloping of the visceral surfaces (liver, spleen).
- Amorphous calcifications.
- The appendiceal tumor can be seen.
- In RM they have intermediate-signal intensity on T1-weighted images, with enhancement after contrast. High-signal intensity on T2 images.
Carcinoid tumor.
Neuroendocrine malignant tumor derived from enterochromaffin cells, which mainly affects the gastrointestinal tract and bronchial tree. The mesentery is affected by direct and lymphatic extension.
Radiological findings.
- Spiculated mesenteric mass, with radial striations towards mesenteric fat (desmoplastic reaction). Enhances significantly after contrast (Fig.5).
- Calcifications (70%).
- Liver, mesenteric and lymph nodes metastases are common.
- Parietal thickening of the adjacent SB loops (infiltration or ischemia).
Infectious and Inflammatory Conditions.
Tuberculous peritonitis.
Uncommon in immunocompetent patients; endemic in North Africa.
It is the most frequent abdominal involvement (by reactivation or hematogenous dissemination).
There are three types:
- Wet variant (90%). Large amount of free fluid or partitioned ascites. High density (20-45 UH) due to its high protein content.
- Dry variant: Mesenteric and peritoneal thickening with marked enhancement. Caseous nodules, and lymphadenopathy, which can be necrotic and calcified.
- Fibrotic variant: mass that includes omentum, mesentery and the affected intestinal loops.
It may be helpful to find stigmas of tuberculosis in other intra-abdominal regions.
Sclerosing mesenteritis.
It is a rare non-neoplastic inflammatory process of the mesentery, of unknown etiology.
Men aged 60-70 with a history of abdominal surgery.
Radiological findings.
- Soft-tissue mass, with enhancement after administration of contrast and gross calcifications inside. It shows radial extensions (misty pattern) and causes retraction of the mesentery, with fixation of the intestinal loops.
- There is usually no ascites or lymphadenopathy.
DDx: Carcinoid, lymphoma.
Mesenteric fibromatosis (desmoid tumor).
Benign proliferation of fibroblasts with locally aggressive behavior, and tendency to recur.
Usually affects young women, and it is associated with familial adenomatous polyposis, hyperstrogenic states, and previous surgery.
Radiological Findings:
- Solid masses poorly defined, sometimes with cystic areas. It may have whirl appearance.
- If stroma predominates: will be similar to muscle in CT and in T1 weighted sequences. Cellular predominance: greater enhancement and high-signal intensity on T2.
Inflammatory Pseudotumor.
Masses due to myofibroblastic proliferation on a variable inflammatory component. They can also be seen in lung and orbit, and usually affect children and young people.
Its presentation is nonspecific: single mass, solid or mixed, usually well defined, with or without enhancement. It is a diagnosis of exclusion.