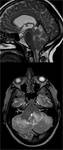
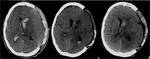
CT and MR are imaging technique of choice for identifying the brain structures and direction and entity of displacement, and are also pivotal for detecting indirect signs of herniation, such as obliteration of liquor spaces and loss of normal anatomical relationships of the involved structures.
Brain herniation can be classified into two broad categories: intracranial and extracranial.
The cranial cavity is compartmented by bony structures and by dural reflections; the major of them are the falx cerebri and the cerebellar tentorium, which define two supratentorial spaces (left and right) and the infra-tentorial space. This anatomy explains the further classification of the intracranial hernias:
- Subfalcine hernia;
- Transtentorial hernia, which can be ascending or descending (lateral and central)
- Tonsillar hernia
Subfalcine hernia
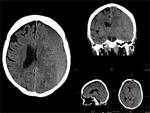
This form is more frequently secondary to a unilateral pathologic condition located in frontal, parietal, or temporal lobe that creates a mass effect, with medial direction compressing on the ipsilateral cingulate gyrus that is shifted down under the falx cerebri.
The septum pellucidum deviates at the level of the foramen of Monro, which serves as a landmark for quantification of the degree of midline shift.
The entity of the midline shift correlates with the prognosis: less than 5 mm deviation has a good prognosis, whereas a shift of more than 15 mm is related to a poor outcome.
If there is a sufficient mass effect there can be an associated displacement of the anterior falx.
Secondary effects: the compression of the ipsilateral ventricle and both foramina of Monro, causing diltatation of the contralateral ventricle; focal necrosis of the cingulated gyrus due to direct compression à it presents clinically with hypobulia, apathy and indifference.
Complications: compression of the anterior cerebral artery, specifically the pericallosal artery, with infarction of the corresponding vascular territoryà the most common clinical manifestation is contralateral leg weakness.
Subfalcine hernias are best demonstrated at coronal MRI.
Transtentorial hernia
Descending transtentorial hernia
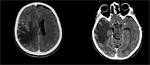
It consists of displacement of brain tissue downward the tentorial notch.
It can be classified into two types: lateral (anterior and posterior) and central hernias.
Lateral: involves the medial temporal lobe.
In the anterior subtype, the uncus is herniated downward into the ipsilateral crural cistern.
It is usually caused by a unilateral supratentorial lesion of the middle cranial fossa producing an inferior and medial mass effect that pushes the uncus over the free edge of the tentorium.
It is usually followed by herniation of more posteriorly located brain tissue.
Typical finding is the effacement of the suprasellar cistern; as the herniation progresses the midbrain and opposite cerebral peduncle are compressed against the tentorial edge.
Secondary effects: compression of corticospinal and corticobulbar tracts above the medullary decussation resulting in motor weakness on the same side as the lesion, known as the Kernohan notch phenomenon (false localizing sign).
Compression of the posterior cerebral artery, third cranial nerve, and aqueduct of Sylvius may result in medial temporal and occipital lobe infarcts with blown pupil, hemiparesis, and hydrocephalus.
The posterior subtype is characterized by medial temporal lobe displacement downward into the posterolateral part of the tentorial incisura, caused by an occipital or posterior temporal disease.
It may involve the tectum at the level of the superior colliculus, resulting in Parinaud syndrome
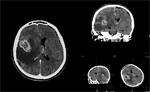
Central hernias: characterized by the descent of midline structures: diencephalon, midbrain, and pons.
It may be caused by a mass effect produced by a midline masse, severe brain edema, supratentorial hydrocephalus.
Typical finding: effacement of the perimesencephalic cisterns (others are caudal displacement of the basilar artery and pineal gland, flattening of the pons against the clivus, and inferior and posterior displacement of the quadrigeminal plate).
Third cranial nerve, posterior cerebral artery, and midbrain can be affected and hydrocephalus develops because of the compression of the cerebral aqueduct
Symptoms associated: progressive central herniation can lead to oculomotor palsy, progressive alteration of consciousness, decerebrate posturing, coma, and eventually death.
The extention to the cerebellar peduncles produces venous congestion along with stretching and tearing of small perforators leading to “Duret hemorrhage”, with poor prognosis, usually death.
Ascending Transtentorial Hernia
It is characterized by the superior displacement of the cerebellar vermis and hemispheres through the tentorial incisura due to mass effect coming from the posterior cranial fossa.
Another possible cause is sudden relief of supratentorial intracranial hypertension.
When the tentorial opening is large, upward herniation of the superior cerebellar vermis will
Typical findings: the distortion of quadrigeminal plate cistern, taking on a flat or convex morphology; "spinning top" appearance of  midbrain due to bilateral compression of the posterior aspect of the midbrain.
midbrain due to bilateral compression of the posterior aspect of the midbrain.
Secondary effects: hydrocephaly due to compression of the aqueduct.
Compression of hemispheric branches of the superior cerebellar arteries and posterior cerebral that causes ischemic infarction of the superior portion of the cerebellar hemispheres and occipital cerebral lobeà nausea, vomiting; rapid progression toward a decreased level of consciousness and, eventually, death.
Tonsillar Hernia
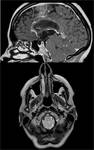
Tonsillar hernia is inferior displacement of the cerebellar tonsils through the foramen magnum. It may be congenital (Chiari spectrum) or acquired.
The McRae line is used as a reference for this measurement. It is obtained by drawing a line from the basion to the opisthion.
The most common cause is an infratentorial mass, creating a downward mass effect, or also a supratentorial mass, in
which case it is usually associated with a DTH.
Typical findings: visualization of tonsils extending below the foramen magnum, anterior brainstem displacement,
and loss of CSF.
Secondary effects: compression of the fourth ventricle producing obstructive supratentorial hydrocephalus; compression of the posterior inferior cerebellar artery with consequent cerebellar infarcts.
The most severe neurologic effect is sudden respiratory arrest.
Transalar Hernia
Transalar hernia is uncommon.and usually associated with subfalcine and transtentorial hernias.
There are a descending type, characterize by the displacement of the frontal lobe posteriorly and inferiorly over the sphenoid wing.
Secondary effects: compression of the middle cerebral artery against the sphenoid ridge with a middle cerebral artery infarction.
With ascending transalar hernia, there is the displacement of the temporal lobe superiorly and anteriorly across the sphenoid ridge.
Secondary effects: compression of the supraclinoid internal carotid artery against the anterior clinoid process with infarction of the anterior and middle cerebral arteries territories.
The most useful finding is the anterior or posterior displacement of the middle cerebral artery.
Extracranial Hernia
External hernias are less common than other types of hernias. They are most frequently caused by post-traumatic cranial defects or secondary to craniectomy performed to decompress intracranial contents in patients with intracranial hypertension after uneffective medical management.
Brain edema is common after decompressive craniectomy.A large craniectomy defect allows the brain to expand without constriction. If the defect is too small, swollen brain may herniate with a “mushroom cap” appearance. This can result in compression of cortical veins and lead to venous infarction and contusion of the brain at the craniectomy margins.
Both CT and MRI are effective in depicting this hernia.
Paradoxical hernia is a rare and potentially fatal complication of decompressive craniectomy, and a neurosurgical emergency. Atmospheric pressure exceeding intracranial pressure at the site of the craniectomy causes a pressure imbalance and consequent subfalcine and/or transtentorial hernia.
It is often triggered by an acute imbalance of ICP secondary to CSF drainage or lumbar puncture
Symptoms include a depressed level of consciousness, autonomic instability, signs of brainstem release, and focal neurologic deficits.
Intracranial hypotension is another cause of cerebral herniation; it is caused by iatrogenic or spontaneous CSF leak that results in downward descent of the brain secondary to a negative pressure gradient between the cranial and spinal compartments.
It must be suspected in patients without an intracranial mass or edema.