Perinatal stroke is an underestimated entity even though it corresponds to 25% of pediatric stroke patients [1]. It encompasses from 20 gestational weeks up to 28 days of life, most of them being neonatal arterial ischemic strokes (NAIS). Other subtypes comprise hemorrhagic stroke, cerebral sinovenous thrombosis (CSVT), and periventricular venous infarction (PVI), which will not be reviewed here [2, 3]. NAIS has an incidence of 35 per 100,000 live births 2300-5000 births [2-4], shows a male predilection and the left middle cerebral artery (MCA) is the most affected territory [2-4], whilst posterior circulation infarctions are unusual in this age group [1].
Risk factors of NAIS remain unclear and it is thought to be a multifactorial disease, including maternal, placental, or fetal/neonatal risk factors (prothrombotic conditions, pregnancy-related hypercoagulability, and proinflammatory status, infection, asphyxia, placental embolism, trauma, drug abuse during pregnancy…) [1-3] Evidence suggests inflammation has an important role in the high incidence of stroke in fetuses and newborns [1]. Nevertheless, a definitive cause is never found in many cases of NAIS, remaining considered idiopathic [1].
NAIS has a variable clinical presentation depending upon the extension and the region of the brain affected, but neonatal seizures are the most typical presentation. Other symptoms include asymmetrical weakness or hypotonia, decreased level of consciousness, lethargy or poor feeding [1-3].
NAIS can lead to long-term neurological consequences such as cerebral palsy [5].
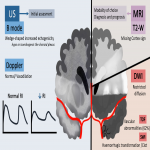
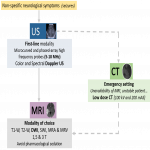
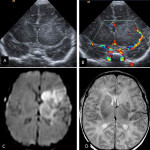
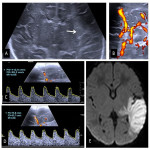
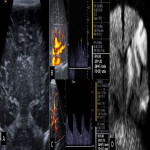
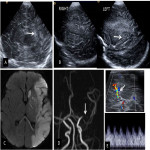
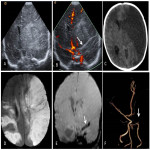
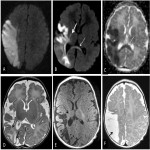
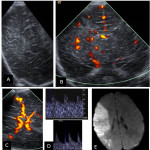
Neuroimaging plays a key role in the diagnosis and management of NAIS, and both Head Ultrasound (US) and cranial MRI are the most important imaging techniques [6].
To illustrate this topic, we reviewed our tertiary-care neonatal referral center perinatal/neonatal ischemic arterial stroke database from 2014 to 2020. All patients had at least one neonatal head ultrasound (US) and MRI.