ETIOLOGY AND PATHOGENESIS
A review published in 2011 (1) found that the most common cause of acquired BBF are hepatic tumors (primary tumors > metastases) closely followed by bile duct obstruction (due to lithiasis, malignancy, post-operative stricture, etc). They also found that the third most common cause is hepatic hydatidosis, which is still the main etiology in third world countries. Other causes include liver abscess, trauma, iatrogenic fistulas (liver resection, radiofrequency ablation, thoracic drainage, etc.) and chronic pancreatitis (1) (2). Even though it is a rare complication of radiofrequency ablation (RFA), there has been an increase in the number of BBF fistulas reported in the past years due to the wide application of RFA (3)(5).
A summary of the main etiologies is depicted in
.
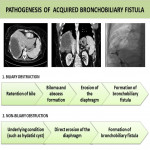
The pathogenesis of BBF (
) is still unclear, but current evidence suggests two possible mechanisms: biliary obstruction and non-biliary obstruction (2). Biliary obstruction can be caused by multiple etiologies, which results in the retention of bile proximal to the obstructive point, biloma formation and subsequently abscess formation (2). The abscess gradually erodes the diaphragm until it reaches the pleural space (pleurobiliary fistula) or lung parenchyma and bronchi (bronchobiliay fistula) (2). In the second case an underlying condition, such as an abscess or hydatid cysts, directly erodes the diaphragm (2). It seems, then, that increased biliary pressure and local inflammation are the two major factors that contribute to this condition (4).
The posteromedial part of the right hemidiaphragm is the most common point for the fistula formation because it is in direct contact with the area nuda hepatis (2).
SIGNS AND SYMPTOMS
The most characteristic symptom, and even considered as pathognomonic, is bilioptysis (1). Other symptoms include irritating cough, fever, jaundice and abdominal pain (mainly right upper quadrant) (1). Chest pain and dyspnea are rare (4).
The most common comorbidity is pneumonia (1).
ROLE OF RADIOLOGISTS IN DIAGNOSIS
The main clinical manifestation that raises suspicion of this condition is bilioptysis, although it is sometimes misdiagnosed as acute pneumonitis or chronic irritable cough producing greenish sputum (1).
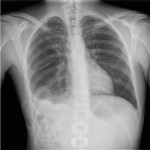
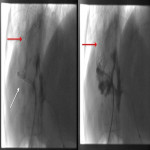
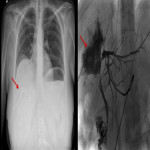
Chest radiograph findings (
) include right hemidiaphragm elevation, shadowing of the pulmonary base, atelectasis, pleural effusion and even pulmonary abscesses (2) (3). Sometimes gas-fluid levels are also present on abdominal radiographs (2).
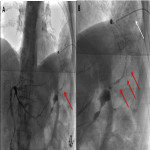
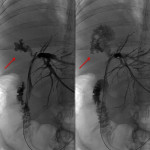
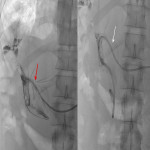
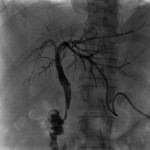
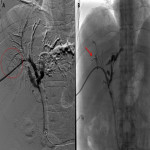
Endoscopic retrograde cholangio-pancreatography (ERCP) and percutaneous transhepatic cholangiography (PTC), the latter performed by interventional radiologists, are invasive techniques that provide direct evidence of the communication between both tracts (1), and are considered to be the more sensitive based on evidence published (2). Some examples are depicted in
. These techniques also allow the treatment of this condition in the case of biliary tract obstruction (2).
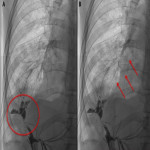
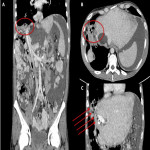
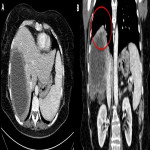
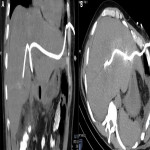
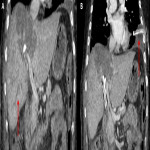
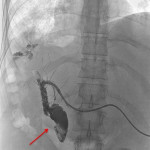
Non-invasive techniques such as hepatobiliary-specific contrast magnetic resonance cholangiopancreatography (MRC) and CT scan can also provide evidence of this connection, even though they are less sensitive methods (1) (2). These techniques usually show indirect manifestations of the BBF such as pneumonia, pleural effusion, liver abscesses or bile duct stones (3)(5), as depicted in
.
shows an iatrogenic BBF.
Nuclear techniques, such as hepatobiliary imino-diacet acid (HIDA) scan have also demonstrated a good sensitivity for this condition (1). It demonstrates the initial tracer activity in the liver that migrates into the thoracic cavity (4). This technique also provides information about liver function and permeability of the bilioenteric system (10).
Techniques such as bronchoscopy and bronchogram are not sensitive enough for directly detecting the fistula (2), even though the presence of bile in the bronchial lavage strongly suggests its presence (3).
The presence of brown bilious crystals surrounded by neutrophils in transbronchial biopsy is also highly suggestive of this entity (3).
ROLE OF RADIOLOGISTS IN TREATMENT
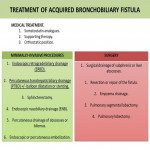
Up until now there has been no published cases in which a patient is cured solely on medical treatment. Somatostatin analogues can be used, as they are thought to reduce the secretion (1)(2). Orthostatic position is recommended to enable the drainage of bile (1). A summary of the main therapeutic options is available in
.
Current therapeutic approach is a matter of discussion between surgery and minimally invasive techniques. In the recent years there has been a tendency to use minimally invasive procedures that have proven to be effective and safe (3). The main techniques used are endoscopic retrograde biliary drainage (ERBD), sphincterotomy, endoscopic nasobiliary drainage (ENBD), percutaneous drainage (abscesses, bilomas…) and percutaneous transhepatic biliary drainage (PTBD) +/- balloon dilatation or stenting (1)(6). Among them, ERBD and PTBD are the most used. The goal of these interventions is to reduce the pressure in the biliary tree by favoring its drainage and thus enabling the indirect healing of the fistula (2).
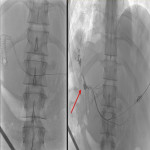
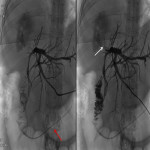
The treatment of the FBB in Fig. 5 with PTBF is shown in
. Another example is shown in
.
Sometimes it might be necessary to drain a biloma or abscess to accelerate indirect healing
.
It is important to consider that other fistulas can be produced as a complication while treating a FBB such as bilioarterial
or bilioportal fistulas.
Surgical procedures are usually used as a final choice when other non-invasive techniques have failed or in specific cases of BBF (1). This includes drainage of subphrenic or liver abscesses, resection or repair of the fistula, and empyema drainage (3). A few patients need pulmonary segmental lobectomy or pulmonary lobectomy (3).
Based on literature, there is still no clear consensus on when one approach is better than the other one, and a multidisciplinary consensus is recommended. It seems, though, that the most recommended treatment for post-traumatic fistulas is surgery.
The combined approach consists of a first step in which biliary drainage (ERCP or PTBD) and percutaneous drainage of abscess are performed. In the second step a delayed surgical intervention is done. This is useful in patients who are not initially candidates for surgery due to the clinical status, and in patients where non-surgical interventions have failed (2).
In the past years more modern techniques have emerged such as histoacryl embolization under bronchoscopy guidance (1).
Coil embolization of the BBF track in combination with bile drainage techniques has been used with success, although the patient finally required surgery due to the persistence of bilioptysis, presumably due to the presence of smaller tracks (6). Authors suggested that microcoils and gel foam could be used to mechanically obstruct these smaller tracks and avoid surgery (6).
Endobronchial embolization using silicon spigots have been also used with success (7). Endoscopic embolization via ERCP with microcoils and cyanoacrylate glue in combination with an ENBD has also been performed with good results (8). A similar approach using vascular plugs has also been performed via percutaneous access (9). In this case, the authors did not use liquid embolic material such as glue because it might cause the migration or expectoration of the vascular plugs.