- NORMAL ANATOMY:
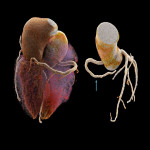
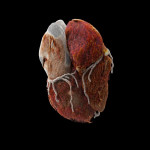
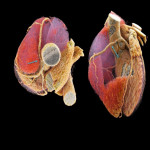
There are four main coronary arteries: the right coronary artery (RCA), Left main coronary artery (LM), left anterior descending artery (LAD) and left circumflex artery (LCX).[1] Coronary arteries are the first aortic branches arising from aortic root at the level of Sinuses of Valsalva.[2]
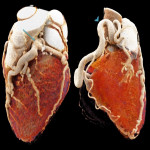
Right Coronary Artery: Arising from the right coronary sinus it runs inferiorly into the right atrioventricular groove toward the posterior interventricular septum.[1,3,4] This gives off the conus branch supplying the right ventricle outflow tract; the sinoatrial node branch for the sinoatrial node and the right atrium; and the acute marginal branch which supplies the RV myocardium; PDA and PLV if dominant.[1,3,5]
Left main coronary artery: Arising from left coronary sinus this runs posterior to the pulmonary truncus before bifurcating into LAD and LCX. [1,3,5]
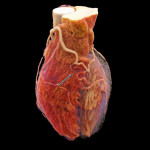
Left anterior descending artery: This runs in the anterior interventricular groove and terminates near the apex of the heart. It gives off diagonal branches for the anterolateral wall of the left ventricle and septal branches for the interventricular septum. [1,3,5]
Left circumflex artery: This descends in the left atrioventricular groove giving off obtuse marginal (OM) branches supplying the lateral wall of the left ventricle. [1,3,5]
- EMBRYOLOGY (4, 8)
In the early embryonic stages the coronary circulation does not exist, instead the blood flows freely through the lumen of the developing heart nourishing the myocardium directly. As the heart size increases a vascular plexus start to develop in the epicardium of the ventricles by the beginning of the third week. This plexus undergoes morphogenesis and expansion and anastomoses with the aorta root in the location of the coronary sinuses. This then provides blood flow to the plexus which differentiates into the arteries, capillaries and veins. A defect at any stage in this process can lead to a coronary anomaly.[2,6]
- ANATOMICAL VARIANTS
Dominance: In 80-85% of the population the distal RCA divides into PDA and PLV branches (right dominant)
. In ~8% the PDA arises from LCX (left dominant system)
and in 7-8% the inferior interventricular septum is perfused by branches from both the RCA and LCX (co-dominant system)
.[3 4]
Ramus intermedius: In ~37% of cases the left main trifurcates into LAD, LCX and intermediate branch which supplies the lateral wall of the left ventricle.[3]
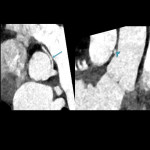
Myocardial bridging: This is where a segment of an artery has an intramuscular course under a bridge of overlying myocardium. This is usually asymptomatic without risk of cardiovascular events.[7] Rarely it can result in vessel compression during systole causing symptoms of angina, arrhythmias, and even sudden cardiac death.[8] The length of the bridged segment and the depth of the course within the myocardium are both markers of increasing risk of flow limitation. [9]
- CORONARY ARTERIES ANOMALIES
There is currently no internationally accepted definition separating coronary variation from coronary anomaly, but it is commonly accepted that variations with a ≤1% prevalence are considered anomalies, while those occurring more frequently are variations. Based on the functional relevance they range from asymptomatic forms that are only recognized post-mortem to ˝malignant˝ causing haemodynamically compromise, associated with shunting, ischaemia and sudden cardiac death.[10,11]
Anomalous origin and course:
Variation in coronary sinus origin and anomalous course: [10–12]
There are four types of anomalous coronary origin from the opposite or non-coronary sinus.
These are associated with anomalous courses defined based on their relationship to the aorta and the pulmonary trunk, with the four most common being:
- interarterial (i.e., between the aorta and the pulmonary artery)
- retro aortic
- prepulmonic
- septal (subpulmonic)
Retro aortic, prepulmonic, and septal (subpulmonic) courses are usually benign, whilst an interarterial course carries a high risk for sudden cardiac death thus classifying it as a malignant course. Interarterial course can also be associated with an intramural segment which means the artery courses within the wall of the aorta itself, further increasing the risk of cardiac events
.[13]
Variation in the location of the coronary ostium outside of aortic root:
- Ascending aorta: this is benign; however, it can result in difficulties in cannulation during coronary angiography.[10]
- Pulmonary artery: most commonly the left coronary artery arises from the PA (ALCAPA)
. Most patients show symptoms in infancy and early childhood, and if left untreated mortality is 90% in the 1st year of life. [10, 14] Treatment of ALCAPA typically requires surgical intervention.[15] Rarely, the RCA (ARCAPA), the circumflex, or both coronary arteries may arise from the pulmonary artery.[11]
Single coronary artery, coronary artery duplication:
- Single coronary artery is an extremely rare anomaly with a prevalence of 0.0024-0.044% of the population. This arises from a single ostium, and may follow the course of the normal RCA or LCA, or have a distribution different from that of the normal coronary arterial tree. Proximal stenosis of a single coronary artery can be life threatening as there is no second vessel from which collateral vessels can form.[10]
- Coronary duplication: Most common is duplication of the LAD artery which has been reported to occur in 0.13%–1% of the general population. [10,16] It is important to recognize this prior to coronary artery bypass graft surgery to ensure successful myocardial revascularization.[17]
Anomalies of intrinsic coronary arterial anatomy
Congenital ostial stenosis or atresia (LCA, LAD, RCA, LCX): Most reported cases describe atresia of the left main coronary artery, which is categorised as a malignant, haemodynamically significant anomaly. Typically there are prominent collateral vessels from the RCA, however these are usually unable to meet the demands of the LV myocardium.[18,19] Ostial atresia is distinguished from single coronary artery by residual beaking' at the site of the expected ostium and extensive collateral formation, while single coronary arteries will have a largely normal course and location of the vessels, with normal tapering from proximal to distal vessel.
Anomalies of coronary termination
Fistulas and AVMs: In fistulas coronary arteries communicate directly with an adjacent cardiac chamber or coronary vein.[11,20] This can cause inadequate blood flow to the myocardium due to the low resistance of the distal communication resulting in preferential flow through these rather than the high resistance myocardial capillaries. This causes a steal phenomenon and can result in symptoms of ischaemia including angina and sudden death.[21]
They are the most common coronary anomaly and can be congenital or acquired, and can be single or multiple.
- IMAGING CORONARY ARTERY ANOMALIES
Approaches to coronary anomaly imaging:
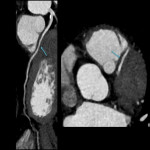
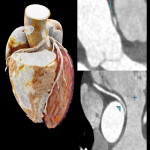
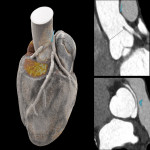
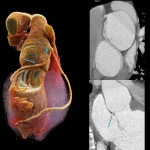
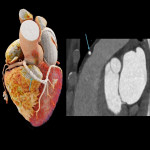
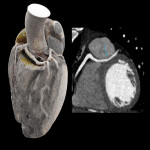
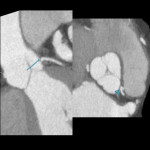
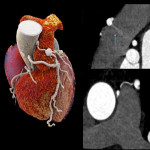
Coronary angiography is still considered the reference standard, however coronary CT has emerged as the diagnostic standard for evaluating coronary anomalies as it offers the best performance in demonstrating aberrant vessels in relation to the surrounding anatomy especially in delineating the ostial origin and proximal path of an anomalous coronary artery.[3,22]
The aim of the cardiac CTA is optimal opacification of coronary arteries with minimisation of cardiac and diaphragmatic motion artefacts which warrants a specific protocol with ECG-gating and patient preparation including optimisation of heart rate and administration of GTN.
Magnetic resonance imaging (MRI) can also demonstrate coronary origin and course without use of ionising radiation, however its spatial resolution is significantly lower that than of CTCA with a long acquisition time.
Functional testing versus anatomical
Functional diagnostic methods, such as myocardial scintigraphy, stress echocardiography and stress cardiac magnetic resonance imaging, can be used to evaluate for ischemia. These methods are complementary to the anatomical assessment and can be helpful in therapeutic decision making in complicated cases.[3] Due to the dynamic interaction between aortic and pulmonary blood flow during increased demand and their effect on the adjacent coronary arteries, exercise stress testing is preferred over vasodilator stress testing.