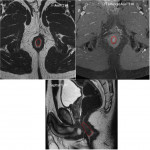
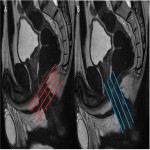
1ST Step: Locate inner Opening
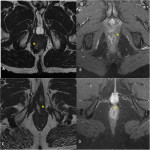
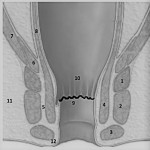
- The inner opening is the origin of the fistula. It corresponds to the closest point of the fistulous path to the lumen of the anal canal.
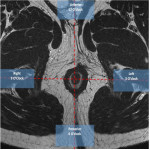
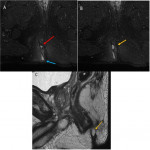
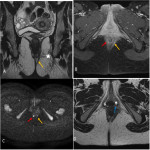
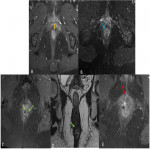
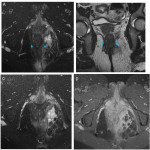
- Axial T2 sequences help to locate it in anal clock (Fig 6), (Fig 7).
- Coronal T2 sequences are used to locate it beyond or above the pelvic floor.
2nd Step: Assess the path of perianal fistula
According to the track pattern of the fistula, it is possible to distinguish:
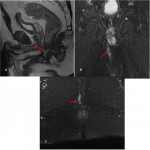
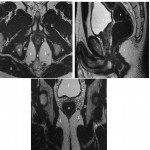
1/ Simple perianal fistula (Fig 8), (Fig 9):
It is a fistula with a unique track linking an inner opening to a unique external orifice.
2/ Complex perianal fistula:
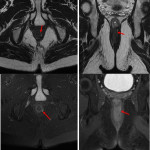
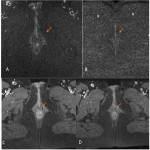
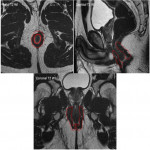
- Horseshoe perianal fistula: Secondary tracks cross the midline around the anal canal in the intersphincteric space. It is a Grade 2 fistula having the shape of a horseshoe. It is also possible to find horseshoe perianal abscesses(Fig 10).
- A perianal fistula that combines a main fistulous pathway with blind extensions(Fig 11).
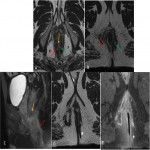
- A perianal fistula that has a main fistulous pathway in association with multiple secondary tracks (Fig 12), (Fig 13), (Fig 14).
It is common to find blind extensions and secondary paths associated with the main track of a perianal fistula in Crohn’s disease. MRI is identified as the modality of choice for an exhaustive preoperative evaluation and cartography of perianal lesions. Failure to recognize secondary tracts and blind extensions can result in relapsing and recurrent sepsis.
3rd STEP: Locate External Opening
The secondary orifices are the mucocutaneous orifices through which the fistula exits. Locating them is easy and fundamental for treatment management. (Fig 15)
4th Step: Assessing Disease activity
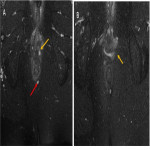
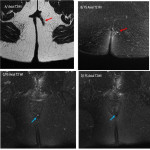
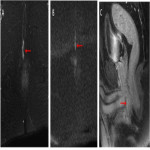
The active fistula tract appears as a hypointense linear structure on T1-weighted imaging and hyperintense on T2-weighted imaging. It enhances in fat-suppressed GRE T1WI after Gadolinium material injection. Tissues surrounding the fistula may show hyperintensity on T2WI related to inflammation(Fig 16).
Inactive tracts are hypointense on T1 and T2 weighted imaging and there is no contrast enhancement. (Fig 17)
MRI is the best modality to assess treatment response: loss of hyperintense signal on T2WI associated with lack of enhancement are considered as good response criteria to therapy(Fig 17).
5th Step: Search for abscesses in the perineum
An abscess is a walled-off collection in the perineum connected to the fistulous tract and whose size exceeds 3mm. It contains liquid and air with a peripheral enhancement (Fig 18 ).
Search for abscesses in the assessment of anoperineal fistulas is essential. It is a prerequisite for therapeutic management, particularly before the use of anti-TNF drugs.
6th Step: Assessing muscular trophicity of the pelvic floor and the anal canal
MRI is the modality of choice to evaluate the muscular atrophy of the perineum and the anal canal to prevent risks of fecal incontinence, especially after surgical treatment.
Surgical options include fistulectomy, fistulotomy, noncutting seton, mucosal advancement flap repair, proctectomy. T1WI is good to assess muscular atrophy and fat infiltration.