Imaging Modalities:
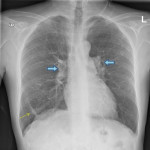
- Plain chest radiograph: May be normal at early CTEPH but bilateral hilar enlargement and cardiomegaly are usual findings. The lung parenchyma may appear normal or if abnormal there may be nonspecific peripheral scarring/atelectasis or more specific peripheral wedge-shaped opacity suggesting infarcts.
- Echocardiogram: Is crucial for initial assessment to estimate systolic pulmonary arterial pressure, right heart changes from the tricuspid regurgitant jet and to evaluate right ventricular function. A firm diagnosis of pulmonary hypertension is only established invasively at right heart catheterisation.
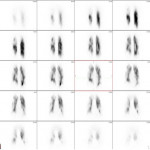
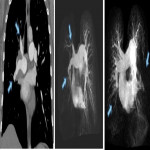
- Ventilation perfusion scintigraphy (V/Q scan): Has a high sensitivity for CTEPH. So, normal V/Q essentially rules out CTEPH. Multiple defects are shown where areas of the lung are ventilated but not perfused. V/Q cannot determine chronicity of the process (acute vs chronic). However, V/Q scan is essential in initial assessment of patients who are allergic to iodinated contrast, severely impaired renal function or pregnant.
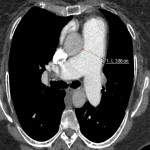
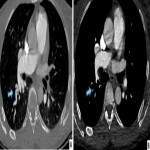
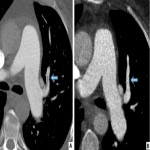
- CT pulmonary angiogram (CTPA): With the advent of improved CT resolution, CTPA has almost completely replaced conventional invasive angiography in the initial evaluation for a cause for pulmonary hypertension. Invasive angiography is routinely performed in the small percentage of cases where balloon angioplasty is being considered to assess the extent of distal disease and for treatment planning.
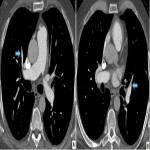
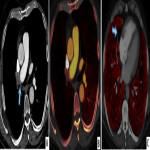
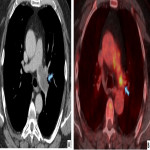
- Dual energy CT pulmonary angiogram: This enables acquisition of iodine perfusion maps at the same time as conventional CTPA and it shows a wedge-shaped perfusion defect. This additional information is useful to correlate the position of any filling defect on CTPA with wedge shaped perfusion defect. The iodine map widely resembles a ventilation/perfusion scan perfusion abnormality. Use of DE CTPA increases the sensitivity of detection of disease.
- Right heart catheterization: Mostly performed in specialist centres. Used for haemodynamic evaluation as more accurate in estimating mean pulmonary arterial pressure and pulmonary vascular resistance. This is essential to select the most eligible patients to offer surgical treatment as it provides ‘prognostic information and an estimate of the relative risk of PEA surgery’.
- MR pulmonary angiography: Is increasingly used particularly in specialist centres. It is useful as a second modality to confirm subtle CT findings. The other probably more important aspect of MR is that it can provide quantitative information about the severity of secondary functional impairment of right heart chambers. It also plays an important role into exclude other differential diagnosis (which were difficult to detect on echocardiogram), treatment planning, and postoperative follow-up.
- Digital subtraction invasive angiography: Although once considered as gold standard for diagnosis of pulmonary embolism, with the advent of modern CT scanners and improving spatial resolution, invasive angiogram is no longer used for initial diagnoses. This investigation is only performed in specialist centres for specific treatment planning for example balloon pulmonary angioplasty.
Common Findings:
- Pulmonary Vascular findings:
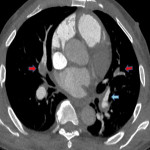
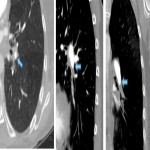
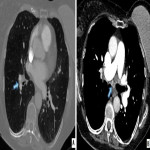
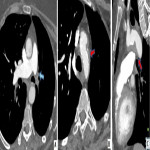
- Pulmonary arterial signs: Variable appearance ranging from more subtle webs, bands, vessel narrowing, intimal irregularity to large calcified thrombi or complete obstruction causing abrupt vessel cut-off.
- Other findings:
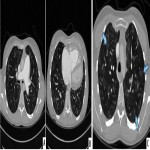
- Lung parenchymal abnormalities:
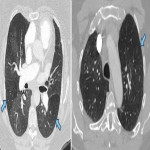
- Mosaic attenuation due to hypo-perfusion
- Peripheral consolidation or scarring from infarctions
- Features of pulmonary hypertension:
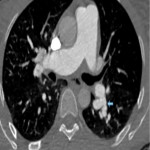
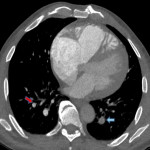
- Enlarged main pulmonary artery
- Dilated right heart chambers
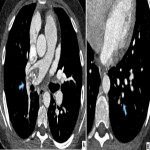
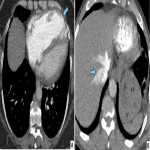
- Tricuspid regurgitation causing contrast reflux to hepatic IVC
- Collateral systemic supply from bronchial arteries
Mimics of CTEPH:
Radiologists should be aware that there are a number of other diseases that may mimic CTEPH.
Disease examples:
- Primary sarcoma of the pulmonary artery
- Idiopathic pulmonary arterial hypertension
- Fibrosing mediastinitis
- Takayasu arteritis involving pulmonary arteries
- Proximal interruption of branch pulmonary artery
Among all modalities of imaging used to search for specific cause of PH, CT pulmonary angiography plays the most important role in differentiating CTEPH from its mimics.
Treatment:
The final decision for appropriate treatment of CTEPH is made in specialist centres at a multidisciplinary team meeting. In the meeting, in the presence of highly experienced clinicians, radiologists and specialist surgeons, the merits and demerits of a specific treatment option along with prognostic benefits are discussed. This is predominantly based at the location and extent of disease in conjunction with individual patient’s clinical symptoms and cardio-pulmonary physiological status.
Treatment options are:
Medical management:
- Anticoagulation: Offered to all CTEPH patients.
- Pulmonary arterial hypertension-targeted therapy: May act as a bridge to the more definite treatment or sole treatment for patients not eligible for surgical intervention.
Intervention:
- Pulmonary endarterectomy (PEA): For more proximal disease.
- Balloon pulmonary angioplasty (BPA): For patients not eligible for surgical treatment or for more distal disease. BPA may require multiple attempts.
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom
Reference: Department of Radiology, Royal Papworth Hospital, Cambridge, United Kingdom