Type:
Educational Exhibit
Keywords:
Interventional non-vascular, Thorax, Ultrasound physics, Experimental, Ultrasound, Biopsy, Cost-effectiveness, Education and training, Infection, Neoplasia
Authors:
A. B. Llanos Gonzalez, N. Arteaga Marrero, E. Villa, M. E. Gómez Gil, O. Acosta Fernández, J. B. Ruiz Alzola, J. González Fernández
DOI:
10.26044/ecr2022/C-12753
Background
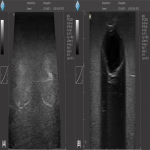
The phantom structure consisted of a rectangular volume fabricated with a 10% mimicking the healthy parenchyma (Figure 1(A)). Pathologies of interest were reproduced as inclusions containing gaseous, liquid or solid materials. The solid inclusions were also replicated with PVA-C using 3D printed molds with spherical and irregular shapes (Figure 1(B) and 1(C)). The other inclusions were assembled creating a polydimethylsiloxane and cellulose as a bubble shape film. The gaseous inclusions were filled with air during the fabrication process, whereas the liquid ones were subsequently filled with a saline solution, although other liquids can be employed. The ribs were 3D printed using polyethylene terephthalate, and embedded into the phantom at approximately 5 mm depth from the upper surface, spaced at roughly 30 mm in between. The phantom’s assembly offers flexibility regarding the number and location of inclusions as well as the insertion of the ribs, which can be easily removed if required.